Bone and Tooth Regeneration: Advances in Dental Medicine
Introduction: Regenerative Medicine Enters A New Dental Era
Regenerative medicine has moved from theoretical research into early-stage clinical reality, fundamentally changing how lost or damaged tissues may be restored. While soft-tissue regeneration has seen significant progress over the past two decades, attention is now rapidly shifting toward the regeneration of hard tissues, particularly bone and teeth—two structures of critical importance to dental and maxillofacial practice.
For decades, dentistry has relied on prosthetic solutions such as implants, bone grafts, and alloplastic materials to compensate for tissue loss. However, emerging research now aims to biologically regenerate bone and teeth, rather than merely replace them. This paradigm shift has profound implications for implantology, orthodontics, pediatric dentistry, and oral surgery.
This article reviews the latest scientific developments in bone substitute biomaterials and tooth regrowth pharmacology, examining how these innovations may redefine future dental treatment protocols.

More Articles About Dr Katsu Takahashi and His Brilliant Work:
The Biological Challenge of Regenerating Hard Tissues
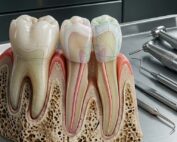
Unlike soft tissues, bones and teeth are characterized by high mineral content, hierarchical microstructures, and complex cellular signaling pathways. Bone is a dynamic tissue, continuously undergoing remodeling through osteoclastic resorption and osteoblastic formation. Teeth, by contrast, exhibit limited regenerative capacity once permanent dentition is established.
From a clinical perspective, the difficulty lies not only in recreating hardness but also in restoring functional architecture, including vascularization, innervation, and biomechanical integration with surrounding tissues.
Recent research suggests that successful regeneration depends on leveraging endogenous biological mechanisms, rather than relying solely on artificial replacements.

Bone Regeneration and Advanced Bone Substitute Materials
Bone Remodeling and Clinical Limitations
In healthy individuals, bone regeneration occurs naturally following fractures when adequate stability and blood supply are present. However, critical-sized bone defects, caused by trauma, tumor resection, periodontal disease, or congenital abnormalities, exceed the body’s intrinsic regenerative capacity.
Traditionally, these defects are managed using:
Autogenous bone grafts
Allogeneic or xenogeneic graft materials
Synthetic substitutes
Each approach carries limitations, including donor site morbidity, resorption unpredictability, infection risk, and incomplete integration.
More Articles About Teeth Regeneration:

Next-Generation Bone Substitute Materials
Recent advancements in material science have led to the development of bioactive bone substitute materials designed to mimic the micro- and nano-structure of natural bone.
Key characteristics of modern bone regenerative materials include:
High porosity to support vascular ingrowth
Osteoconductive scaffolding
Gradual bioresorption synchronized with new bone formation
Biochemical signaling that promotes osteogenesis
Unlike traditional inert materials, these next-generation substitutes are fully resorbable, allowing them to be replaced entirely by newly formed host bone over time.
Clinical Implications for Dentistry and Implantology
For dental professionals, these developments have direct relevance to:
Ridge preservation
Sinus lift procedures
Peri-implant bone regeneration
Management of periodontal bone defects
Improved handling properties and predictable remodeling behavior are making these materials increasingly attractive alternatives to conventional grafts. Ongoing research focuses on improving injectability, setting time, and surgical adaptability, further enhancing chairside usability.

Tooth Regeneration: From Biological Theory to Pharmacological Reality
The Traditional Limitation of Human Dentition
Human dentition is traditionally considered non-regenerative beyond the eruption of permanent teeth. Once lost due to caries, trauma, or periodontal disease, teeth are typically replaced using prosthetic or implant-based solutions.
This long-standing assumption is now being challenged by groundbreaking research in tooth development biology.
The Concept of a Tooth-Regrowth Drug
Scientists have identified molecular pathways that suppress additional tooth formation after permanent dentition is established. By selectively inhibiting these pathways, researchers have successfully stimulated new tooth development in animal models.
In controlled studies, experimental pharmacological agents triggered the formation of additional incisors in mice, demonstrating that latent odontogenic potential remains present in mammals.
This discovery suggests that tooth loss may not be an irreversible condition, but rather a biologically suppressed capability.
Targeting Congenital Anodontia
The primary clinical target for early application is congenital anodontia or oligodontia, conditions characterized by the absence of multiple teeth from birth.
Current treatment options rely heavily on:
Removable prostheses
Long-term orthodontic intervention
Dental implants after skeletal maturity
These approaches are costly, time-intensive, and often psychologically burdensome for pediatric patients.
A tooth-regrowth drug could offer a biological solution, enabling patients to develop their own natural teeth, complete with periodontal ligament integration and alveolar bone stimulation.
Potential Applications Beyond Congenital Conditions
While initial regulatory approval efforts focus on congenital disorders, future applications could extend to:
Tooth loss due to trauma
Advanced caries
Periodontal disease
Age-related tooth loss
For dental professionals, this could dramatically reduce reliance on implants and prosthetics, particularly in younger patients or cases with compromised bone volume.
Impact on Implant Dentistry and Prosthodontics
The emergence of tooth regeneration technologies does not signal the immediate obsolescence of implants. Instead, it suggests a future in which treatment planning becomes more biologically driven, offering patients multiple regenerative pathways.
In the medium term, regenerative dentistry is likely to coexist with traditional restorative solutions, with case selection playing a decisive role.
Regulatory and Clinical Translation Challenges
Despite promising results, several hurdles remain before widespread clinical adoption:
Long-term safety evaluation
Controlled human clinical trials
Ethical and regulatory approval
Predictability of tooth morphology and eruption positioning
Dental professionals should expect a gradual integration of these technologies rather than a rapid disruption.
The Future of Regenerative Dentistry
The convergence of material science, molecular biology, and clinical dentistry is reshaping how practitioners think about tissue loss and restoration. Bone substitute materials that fully remodel into native bone and pharmacological agents capable of stimulating tooth growth represent a fundamental shift from replacement to regeneration.
For clinicians, staying informed about these developments will be essential as regenerative therapies move closer to mainstream practice.
Conclusion
Regenerative medicine is redefining the future of dentistry by targeting the biological foundations of bone and tooth formation. Advances in bioresorbable bone substitute materials are already improving outcomes in oral surgery and implantology, while experimental tooth-regrowth therapies promise to revolutionize how tooth loss is treated.
Although clinical implementation will require time, validation, and regulation, the direction is clear: the next generation of dental care will be regenerative, patient-specific, and biologically integrated.
Dental professionals who understand and adapt to these innovations will be best positioned to lead the future of clinical dentistry.
Frequently Asked Questions (FAQ)
1. What is bone regeneration in dentistry?
Bone regeneration in dentistry refers to biological processes and clinical techniques that stimulate new bone formation to restore lost or deficient alveolar or maxillofacial bone. Modern approaches rely on bioactive bone substitute materials that support osteoconduction and gradual replacement with native bone, rather than permanent artificial structures.
2. How do bone substitute materials differ from traditional bone grafts?
Unlike traditional autogenous or allogenic bone grafts, advanced bone substitute materials are engineered to replicate the microstructure of natural bone. They are designed to be fully resorbable, allowing them to integrate with host tissue and be replaced entirely by newly formed bone over time, reducing donor site morbidity and surgical complexity.
3. Can teeth really be regenerated in humans?
Current research indicates that humans retain dormant biological pathways capable of tooth development. Experimental tooth-regrowth drugs have successfully induced new tooth formation in animal models. While human clinical use is not yet available, early-stage research suggests that tooth regeneration may become a viable treatment option in the future.
4. Who are the ideal candidates for tooth regrowth therapies?
The primary target population for tooth-regrowth therapies is patients with congenital conditions such as anodontia or oligodontia. Future applications may extend to patients who have lost teeth due to trauma, severe caries, or periodontal disease, pending further clinical validation and regulatory approval.
5. Will tooth regeneration replace dental implants?
Tooth regeneration is not expected to fully replace dental implants in the near term. Instead, it will likely complement existing restorative options. Case selection, patient age, bone availability, and systemic factors will determine whether regenerative therapies or implant-based solutions are more appropriate.
6. When might regenerative dental therapies become clinically available?
Bone regenerative materials are already in clinical use and continue to improve. Tooth-regrowth therapies remain in the research and early regulatory phases. Widespread clinical adoption is expected to occur gradually, following long-term safety studies and controlled human trials.
7. What is the USAG-1 protein?
USAG-1 (Uterine Sensitization-Associated Gene-1), also known as SOSTDC1, is a regulatory protein that plays an inhibitory role in tooth and bone development. It functions by suppressing key signaling pathways—primarily the BMP (Bone Morphogenetic Protein) and Wnt signaling pathways—which are essential for odontogenesis and osteogenesis. In normal human development, USAG-1 helps limit the number of teeth that form. Experimental studies have shown that blocking or neutralizing USAG-1 can reactivate latent tooth-forming potential, making it a significant molecular target in tooth regeneration research.
8. What is TRG035?
TRG035 is an experimental monoclonal antibody drug designed to inhibit the activity of the USAG-1 protein. By blocking USAG-1, TRG035 aims to release the suppression on tooth-forming signaling pathways, thereby enabling natural tooth development. The drug has demonstrated promising results in preclinical animal studies, including the induction of additional tooth formation. TRG035 is currently being investigated as a potential treatment for congenital tooth agenesis, and it represents one of the most advanced pharmacological approaches in the emerging field of regenerative dentistry. Clinical use in humans remains subject to regulatory approval and further safety and efficacy trials.
Reference:
Can bones and teeth regenerate: Latest research into creating hard tissue in the human body
BS Nippon Television
Main broadcast: December 4th (Thursday) 22:30 ~ 22:56
Recent Articles
Introduction: Regenerative Medicine Enters A New Dental Era
Regenerative medicine has moved from theoretical research into early-stage clinical reality, fundamentally changing how lost or damaged tissues may be restored. While soft-tissue regeneration has seen significant progress over the past two decades, attention is now rapidly shifting toward the regeneration of hard tissues, particularly bone and teeth—two structures of critical importance to dental and maxillofacial practice.
For decades, dentistry has relied on prosthetic solutions such as implants, bone grafts, and alloplastic materials to compensate for tissue loss. However, emerging research now aims to biologically regenerate bone and teeth, rather than merely replace them. This paradigm shift has profound implications for implantology, orthodontics, pediatric dentistry, and oral surgery.
This article reviews the latest scientific developments in bone substitute biomaterials and tooth regrowth pharmacology, examining how these innovations may redefine future dental treatment protocols.

More Articles About Dr Katsu Takahashi and His Brilliant Work:
The Biological Challenge of Regenerating Hard Tissues
Unlike soft tissues, bones and teeth are characterized by high mineral content, hierarchical microstructures, and complex cellular signaling pathways. Bone is a dynamic tissue, continuously undergoing remodeling through osteoclastic resorption and osteoblastic formation. Teeth, by contrast, exhibit limited regenerative capacity once permanent dentition is established.
From a clinical perspective, the difficulty lies not only in recreating hardness but also in restoring functional architecture, including vascularization, innervation, and biomechanical integration with surrounding tissues.
Recent research suggests that successful regeneration depends on leveraging endogenous biological mechanisms, rather than relying solely on artificial replacements.

Bone Regeneration and Advanced Bone Substitute Materials
Bone Remodeling and Clinical Limitations
In healthy individuals, bone regeneration occurs naturally following fractures when adequate stability and blood supply are present. However, critical-sized bone defects, caused by trauma, tumor resection, periodontal disease, or congenital abnormalities, exceed the body’s intrinsic regenerative capacity.
Traditionally, these defects are managed using:
Autogenous bone grafts
Allogeneic or xenogeneic graft materials
Synthetic substitutes
Each approach carries limitations, including donor site morbidity, resorption unpredictability, infection risk, and incomplete integration.
More Articles About Teeth Regeneration:

Next-Generation Bone Substitute Materials
Recent advancements in material science have led to the development of bioactive bone substitute materials designed to mimic the micro- and nano-structure of natural bone.
Key characteristics of modern bone regenerative materials include:
High porosity to support vascular ingrowth
Osteoconductive scaffolding
Gradual bioresorption synchronized with new bone formation
Biochemical signaling that promotes osteogenesis
Unlike traditional inert materials, these next-generation substitutes are fully resorbable, allowing them to be replaced entirely by newly formed host bone over time.
Clinical Implications for Dentistry and Implantology
For dental professionals, these developments have direct relevance to:
Ridge preservation
Sinus lift procedures
Peri-implant bone regeneration
Management of periodontal bone defects
Improved handling properties and predictable remodeling behavior are making these materials increasingly attractive alternatives to conventional grafts. Ongoing research focuses on improving injectability, setting time, and surgical adaptability, further enhancing chairside usability.

Tooth Regeneration: From Biological Theory to Pharmacological Reality
The Traditional Limitation of Human Dentition
Human dentition is traditionally considered non-regenerative beyond the eruption of permanent teeth. Once lost due to caries, trauma, or periodontal disease, teeth are typically replaced using prosthetic or implant-based solutions.
This long-standing assumption is now being challenged by groundbreaking research in tooth development biology.
The Concept of a Tooth-Regrowth Drug
Scientists have identified molecular pathways that suppress additional tooth formation after permanent dentition is established. By selectively inhibiting these pathways, researchers have successfully stimulated new tooth development in animal models.
In controlled studies, experimental pharmacological agents triggered the formation of additional incisors in mice, demonstrating that latent odontogenic potential remains present in mammals.
This discovery suggests that tooth loss may not be an irreversible condition, but rather a biologically suppressed capability.
Targeting Congenital Anodontia
The primary clinical target for early application is congenital anodontia or oligodontia, conditions characterized by the absence of multiple teeth from birth.
Current treatment options rely heavily on:
Removable prostheses
Long-term orthodontic intervention
Dental implants after skeletal maturity
These approaches are costly, time-intensive, and often psychologically burdensome for pediatric patients.
A tooth-regrowth drug could offer a biological solution, enabling patients to develop their own natural teeth, complete with periodontal ligament integration and alveolar bone stimulation.
Potential Applications Beyond Congenital Conditions
While initial regulatory approval efforts focus on congenital disorders, future applications could extend to:
Tooth loss due to trauma
Advanced caries
Periodontal disease
Age-related tooth loss
For dental professionals, this could dramatically reduce reliance on implants and prosthetics, particularly in younger patients or cases with compromised bone volume.
Impact on Implant Dentistry and Prosthodontics
The emergence of tooth regeneration technologies does not signal the immediate obsolescence of implants. Instead, it suggests a future in which treatment planning becomes more biologically driven, offering patients multiple regenerative pathways.
In the medium term, regenerative dentistry is likely to coexist with traditional restorative solutions, with case selection playing a decisive role.
Regulatory and Clinical Translation Challenges
Despite promising results, several hurdles remain before widespread clinical adoption:
Long-term safety evaluation
Controlled human clinical trials
Ethical and regulatory approval
Predictability of tooth morphology and eruption positioning
Dental professionals should expect a gradual integration of these technologies rather than a rapid disruption.
The Future of Regenerative Dentistry
The convergence of material science, molecular biology, and clinical dentistry is reshaping how practitioners think about tissue loss and restoration. Bone substitute materials that fully remodel into native bone and pharmacological agents capable of stimulating tooth growth represent a fundamental shift from replacement to regeneration.
For clinicians, staying informed about these developments will be essential as regenerative therapies move closer to mainstream practice.
Conclusion
Regenerative medicine is redefining the future of dentistry by targeting the biological foundations of bone and tooth formation. Advances in bioresorbable bone substitute materials are already improving outcomes in oral surgery and implantology, while experimental tooth-regrowth therapies promise to revolutionize how tooth loss is treated.
Although clinical implementation will require time, validation, and regulation, the direction is clear: the next generation of dental care will be regenerative, patient-specific, and biologically integrated.
Dental professionals who understand and adapt to these innovations will be best positioned to lead the future of clinical dentistry.
Frequently Asked Questions (FAQ)
1. What is bone regeneration in dentistry?
Bone regeneration in dentistry refers to biological processes and clinical techniques that stimulate new bone formation to restore lost or deficient alveolar or maxillofacial bone. Modern approaches rely on bioactive bone substitute materials that support osteoconduction and gradual replacement with native bone, rather than permanent artificial structures.
2. How do bone substitute materials differ from traditional bone grafts?
Unlike traditional autogenous or allogenic bone grafts, advanced bone substitute materials are engineered to replicate the microstructure of natural bone. They are designed to be fully resorbable, allowing them to integrate with host tissue and be replaced entirely by newly formed bone over time, reducing donor site morbidity and surgical complexity.
3. Can teeth really be regenerated in humans?
Current research indicates that humans retain dormant biological pathways capable of tooth development. Experimental tooth-regrowth drugs have successfully induced new tooth formation in animal models. While human clinical use is not yet available, early-stage research suggests that tooth regeneration may become a viable treatment option in the future.
4. Who are the ideal candidates for tooth regrowth therapies?
The primary target population for tooth-regrowth therapies is patients with congenital conditions such as anodontia or oligodontia. Future applications may extend to patients who have lost teeth due to trauma, severe caries, or periodontal disease, pending further clinical validation and regulatory approval.
5. Will tooth regeneration replace dental implants?
Tooth regeneration is not expected to fully replace dental implants in the near term. Instead, it will likely complement existing restorative options. Case selection, patient age, bone availability, and systemic factors will determine whether regenerative therapies or implant-based solutions are more appropriate.
6. When might regenerative dental therapies become clinically available?
Bone regenerative materials are already in clinical use and continue to improve. Tooth-regrowth therapies remain in the research and early regulatory phases. Widespread clinical adoption is expected to occur gradually, following long-term safety studies and controlled human trials.
7. What is the USAG-1 protein?
USAG-1 (Uterine Sensitization-Associated Gene-1), also known as SOSTDC1, is a regulatory protein that plays an inhibitory role in tooth and bone development. It functions by suppressing key signaling pathways—primarily the BMP (Bone Morphogenetic Protein) and Wnt signaling pathways—which are essential for odontogenesis and osteogenesis. In normal human development, USAG-1 helps limit the number of teeth that form. Experimental studies have shown that blocking or neutralizing USAG-1 can reactivate latent tooth-forming potential, making it a significant molecular target in tooth regeneration research.
8. What is TRG035?
TRG035 is an experimental monoclonal antibody drug designed to inhibit the activity of the USAG-1 protein. By blocking USAG-1, TRG035 aims to release the suppression on tooth-forming signaling pathways, thereby enabling natural tooth development. The drug has demonstrated promising results in preclinical animal studies, including the induction of additional tooth formation. TRG035 is currently being investigated as a potential treatment for congenital tooth agenesis, and it represents one of the most advanced pharmacological approaches in the emerging field of regenerative dentistry. Clinical use in humans remains subject to regulatory approval and further safety and efficacy trials.
Reference:
Can bones and teeth regenerate: Latest research into creating hard tissue in the human body
BS Nippon Television
Main broadcast: December 4th (Thursday) 22:30 ~ 22:56
Recent Articles
Pulsed Electromagnetic Field (PEMF) Use in Implant Dentistry
Pulsed Electromagnetic Field (PEMF) Use in Implant Dentistry Abstract and Historical Background Pulsed Electromagnetic Field (PEMF) therapy refers to the application of low-frequency electromagnetic [...]
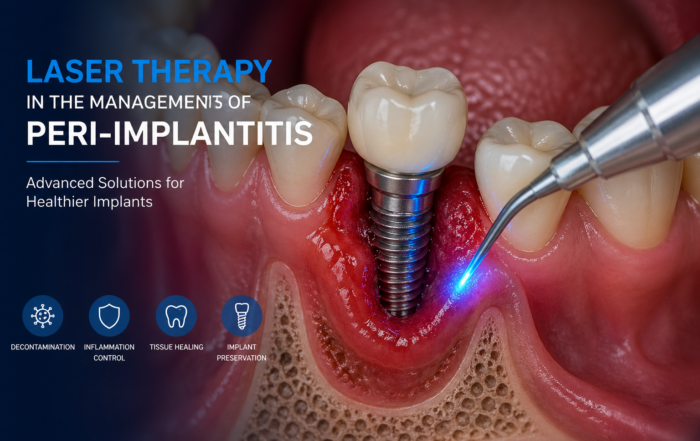
Laser Therapy in the Management of Peri-Implantitis
Laser Therapy in the Management of Peri-Implantitis Laser technology has become an increasingly valuable adjunct in the treatment of peri-implant diseases, particularly peri-implantitis. Its [...]
Magnetically Guided Dental Nanobots (CalBots) Are Real
Magnetically Guided Dental Nanobots (CalBots) Are Real The concept of nanobots in dentistry has long been associated with futuristic speculation. However, recent peer-reviewed research [...]
Peri-Implantitis Treatment & Prevention Methods
Peri-Implantitis Treatment & Prevention Methods Peri-implantitis remains one of the most significant biological complications affecting dental implants, posing a serious threat to long-term implant [...]
Latest Sinus Lifting Techniques in Modern Implant Dentistry
Latest Sinus Lifting Techniques in Modern Implant Dentistry A Comprehensive Clinical Review Introduction to Sinus Lifting in Implantology Sinus lifting, or maxillary sinus floor [...]
Biomechanics of the Triple Abutment & BOPiT Concept
Dental Biomechanics · Implant Science · Clinical Evidence Biomechanics of the Triple Abutment & BOPiT Concept How a saddle-shaped mathematical surface is rewriting the rules of load distribution [...]