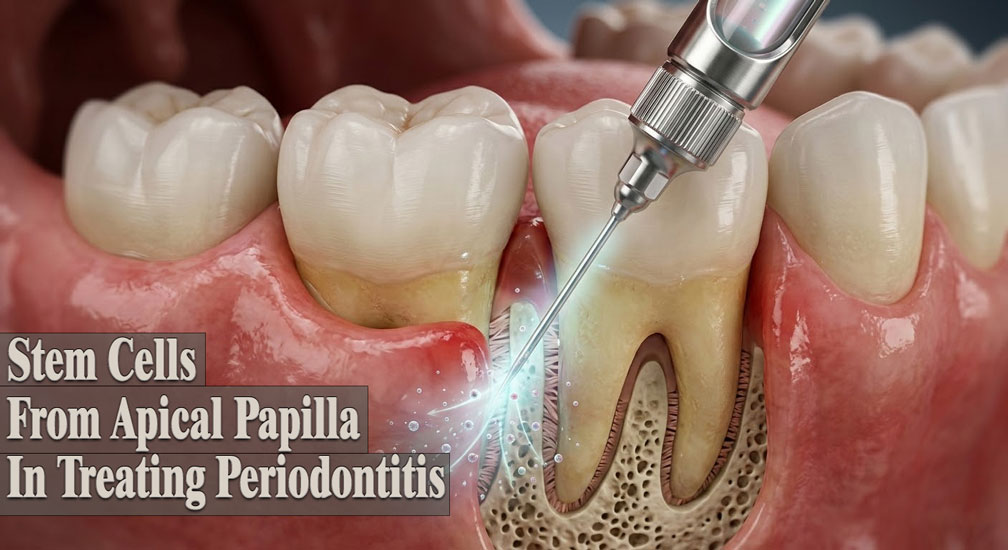
Stem Cells from Apical Papilla in Treating Periodontitis
Introduction
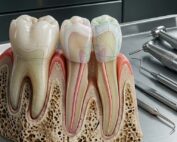
Periodontitis remains one of the most prevalent chronic inflammatory diseases affecting the oral cavity. Characterized by progressive destruction of the periodontal ligament, cementum, gingiva, and alveolar bone, the disease ultimately leads to tooth mobility and tooth loss if left untreated. Conventional periodontal therapies—such as scaling and root planing, surgical flap procedures, and regenerative grafting techniques—aim to control infection and repair damaged tissues. However, complete regeneration of the periodontal apparatus remains difficult to achieve with traditional methods.
In recent years, regenerative dentistry has focused on the use of mesenchymal stem cells (MSCs) as a promising therapeutic approach. Among various MSC sources, Stem Cells from Apical Papilla (SCAPs) have emerged as a particularly promising candidate for periodontal tissue regeneration. These cells originate from the apical papilla of immature permanent teeth and exhibit remarkable proliferative and differentiation capabilities.
Recent experimental research suggests that local injection of SCAPs can significantly improve periodontal tissue regeneration, including alveolar bone formation, periodontal ligament restoration, and cementum regeneration. This article explores the biological properties of SCAPs, their advantages over other stem cell sources, and the experimental evidence supporting their use in treating periodontitis.
Understanding Stem Cells from Apical Papilla (SCAPs)
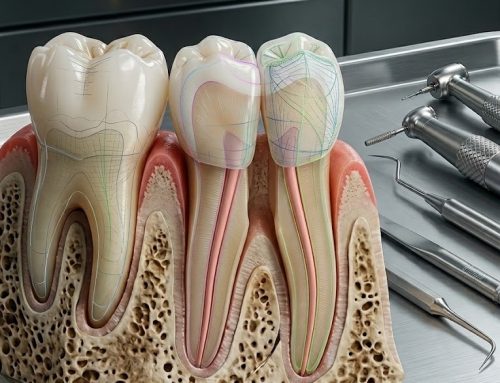
Stem Cells from Apical Papilla are a specialized type of dental-derived mesenchymal stem cell located in the apical papilla tissue of immature permanent teeth, particularly developing third molars.
The apical papilla is a soft tissue structure located at the root apex during tooth development. It plays a critical role in root formation and contains highly undifferentiated cells capable of extensive proliferation and differentiation.
SCAPs possess several defining biological characteristics:
High proliferative capacity
Strong osteogenic and odontogenic differentiation potential
Ability to form dentin-like structures
Immunomodulatory properties
Capability to generate pulp-like tissues
These properties make SCAPs particularly suitable for regenerative dental therapies, including pulp regeneration, bone regeneration, and periodontal tissue engineering.
Compared to other dental stem cells, such as:
Periodontal ligament stem cells (PDLSCs)
Dental pulp stem cells (DPSCs)
SCAPs demonstrate higher proliferation rates and greater mineralization potential, making them highly attractive for regenerative applications.
Periodontitis and the Need for Regenerative Therapies
Periodontitis is a complex disease driven by microbial biofilms and host immune responses. Over time, chronic inflammation leads to the progressive destruction of supporting structures around the tooth, including:
Alveolar bone
Periodontal ligament
Cementum
Gingival connective tissue
Traditional periodontal treatments focus on:
Eliminating infection
Reducing inflammation
Preventing further tissue destruction
However, true regeneration of the entire periodontal apparatus remains challenging.
Regenerative procedures such as:
Guided tissue regeneration (GTR)
Bone grafting
Enamel matrix derivatives
can stimulate partial regeneration, but the results are often inconsistent.
Stem cell-based therapies represent a biological solution capable of restoring the lost architecture of periodontal tissues through cellular regeneration rather than simple repair.
Advantages of SCAPs for Periodontal Regeneration
SCAPs offer several advantages compared with other stem cell sources used in periodontal regeneration.
1. High Proliferation Rate
SCAPs show greater population-doubling capacity than many other dental stem cells. This high proliferative ability allows for efficient expansion in laboratory culture before therapeutic use.
2. Strong Osteogenic Potential
Studies have demonstrated that SCAPs exhibit strong osteogenic and dentinogenic differentiation, meaning they can readily form:
Bone tissue
Dentin-like structures
Cementum-like tissue
These properties are essential for reconstructing the complex structure of periodontal tissues.
3. Accessibility of the Cell Source
SCAPs can be obtained from extracted immature wisdom teeth, which are frequently removed in routine dental procedures. This provides an accessible and minimally invasive source of stem cells.
4. Immunomodulatory Effects
SCAPs also demonstrate immunosuppressive properties, particularly by suppressing T-cell proliferation. This feature may reduce immune rejection and allow for allogeneic transplantation in future clinical applications.
5. Enhanced Regenerative Potential
Compared with bone marrow mesenchymal stem cells (BMMSCs), SCAPs demonstrate:
Comparable osteogenic differentiation
Higher proliferation rates
Easier isolation
These advantages make SCAPs an attractive cell source for periodontal tissue engineering.
Experimental Study: SCAPs in Periodontitis Treatment
To evaluate the regenerative potential of SCAPs in periodontal defects, researchers conducted a controlled experimental study using minipig models of periodontitis. Swine are frequently used in dental research because their periodontal anatomy closely resembles that of humans.
Creation of Periodontal Defects
Researchers surgically created standardized periodontal defects measuring:
3 mm width
5 mm depth
7 mm length
These defects were generated near the mandibular first molars of six miniature pigs to simulate advanced periodontitis.
After four weeks, the animals were divided into two groups:
Control Group: Received injections of saline solution (0.9% NaCl)
SCAP Treatment Group: Received injections of SCAPs suspended in saline
Each treatment site received approximately 2 × 10⁶ SCAP cells, injected subperiosteally around the periodontal defect.
The regenerative outcomes were evaluated 12 weeks after treatment using clinical measurements, CT imaging, and histological analysis.
Clinical Improvements After SCAP Treatment
Clinical periodontal parameters showed significant improvement in the SCAP-treated sites.
Probing Depth Reduction
Probing depth (PD) decreased significantly in the SCAP group:
SCAP group: 5.44 ± 0.77 mm
Control group: 7.33 ± 1.0 mm
This reduction indicates improved periodontal attachment and reduced pocket depth.
Attachment Loss Improvement
Attachment loss (AL) also improved significantly:
SCAP group: 7.78 ± 0.84 mm
Control group: 9.44 ± 1.07 mm
These results demonstrate that SCAP therapy helped restore periodontal attachment structures.
Gingival Recession
Interestingly, gingival recession showed no statistically significant difference between the groups, suggesting that SCAPs primarily affected deeper periodontal structures rather than superficial gingival position.
Overall, these findings indicate that SCAP injection promotes functional periodontal recovery.
CT Evidence of Alveolar Bone Regeneration
Three-dimensional CT imaging provided strong evidence of significant alveolar bone regeneration in the SCAP-treated sites.
Quantitative analysis revealed:
SCAP group bone regeneration: 22.73 ± 4.94 mm³
Control group bone regeneration: 9.87 ± 3.53 mm³
This represents a substantial increase in newly formed bone volume in the SCAP group.
Three-dimensional reconstructions demonstrated that SCAP treatment produced nearly complete regeneration of the alveolar bone defect, while the control group showed only limited bone formation.
These findings highlight the strong osteogenic capacity of SCAPs in periodontal regeneration.
Histological Evidence of Periodontal Tissue Regeneration
Histopathological examination further confirmed the regenerative potential of SCAP therapy.
In the control group, typical features of periodontitis were still present, including:
Deep periodontal pockets
Inflammatory cell infiltration
Absence of an organized periodontal ligament
Lack of Sharpey’s fibers
In contrast, the SCAP-treated group showed remarkable regeneration, including:
Formation of new periodontal ligament fibers
Presence of Sharpey’s fibers
Reduced inflammatory infiltration
Formation of thicker and more mature cementum
Quantitative analysis revealed that newly formed cementum in the SCAP group was significantly thicker:
SCAP group: 158.1 ± 16.3 μm
Control group: 91.4 ± 7.9 μm
These histological findings confirm that SCAP therapy can regenerate multiple components of the periodontal complex, including bone, ligament, and cementum.
Minimally Invasive Delivery via Local Injection
One particularly important aspect of this study was the delivery technique used for SCAP therapy.
Traditional stem cell-based tissue engineering often requires:
Biomaterial scaffolds
Surgical flap procedures
Complex transplantation methods
However, this study utilized simple local cell injection, which offers several advantages:
Minimally invasive procedure
Reduced surgical trauma
Faster clinical application
Lower cost and complexity
The results demonstrate that cell injection alone can effectively stimulate periodontal regeneration, making the approach highly attractive for future clinical therapies.
Future Perspectives in Periodontal Regenerative Medicine
Although the experimental results are promising, further research is necessary before SCAP therapy becomes widely available in clinical practice.
Future studies will likely focus on:
Understanding the Regenerative Mechanisms
Researchers still need to fully understand how SCAPs mediate tissue regeneration, including their interactions with:
Host cells
Growth factors
Immune responses
Extracellular matrix components
Combining SCAPs with Growth Factors
Combining SCAPs with bioactive molecules such as:
BMPs
VEGF
PDGF
may further enhance regenerative outcomes.
Gene Modification Strategies
Gene-editing techniques could improve SCAP survival, proliferation, and differentiation in periodontal defects.
Clinical Trials
Human clinical trials will be essential to confirm the safety and effectiveness of SCAP-based therapies in treating periodontal disease.
Conclusion
Stem Cells from the apical papilla represent one of the most promising tools in periodontal regenerative medicine. Their high proliferative capacity, strong osteogenic potential, and immunomodulatory properties make them ideal candidates for regenerating damaged periodontal tissues.
Experimental research in animal models demonstrates that local injection of SCAPs can significantly improve periodontal healing, promoting regeneration of alveolar bone, periodontal ligament, and cementum. Clinical parameters such as probing depth and attachment loss also show significant improvement following treatment.
Perhaps most importantly, SCAP therapy can be delivered through minimally invasive injection techniques, which may simplify future clinical applications.
As research in regenerative dentistry continues to advance, SCAP-based therapies may soon offer a biological solution for restoring periodontal tissues, potentially transforming the way clinicians treat advanced periodontitis.
FAQ: Stem Cells from Apical Papilla in Treating Periodontitis
1. What are Stem Cells from Apical Papilla (SCAPs)?
Stem Cells from Apical Papilla (SCAPs) are a type of dental-derived mesenchymal stem cell located in the apical papilla, the soft tissue found at the tip of developing tooth roots. These cells are typically harvested from immature wisdom teeth that are extracted for clinical reasons. SCAPs possess strong regenerative capabilities, including the ability to proliferate rapidly and differentiate into various cell types such as odontoblast-like cells, bone-forming cells, and periodontal ligament cells. Because of these properties, SCAPs are considered promising candidates for regenerative dentistry, particularly for rebuilding tissues destroyed by periodontitis.
2. Why are SCAPs considered promising for periodontal regeneration?
SCAPs demonstrate several biological advantages compared with other dental stem cells. Research shows they have higher proliferation rates, stronger mineralization capacity, and greater osteogenic differentiation potential than periodontal ligament stem cells (PDLSCs) and dental pulp stem cells (DPSCs). These characteristics allow them to contribute effectively to the regeneration of alveolar bone, cementum, and periodontal ligament, which are the key tissues damaged in periodontitis.
3. How are SCAPs obtained for research or therapeutic use?
SCAPs are typically isolated from the apical papilla tissue of immature third molars (wisdom teeth). After extraction, the apical papilla is carefully separated from the root tip and enzymatically digested to release the stem cells. The cells are then cultured in specialized growth media under controlled laboratory conditions. In the referenced study, SCAPs were expanded in culture and used between passages 3–5 for experimental periodontal regeneration.
4. How were SCAPs used to treat periodontitis in the study?
In the study model, periodontitis defects were surgically created in miniature pigs to simulate periodontal tissue destruction. Researchers treated these defects by locally injecting SCAPs suspended in saline solution into the tissues surrounding the periodontal defect. The injections were delivered at three points around each defect—mesial, distal, and central areas—allowing the stem cells to interact directly with the damaged periodontal structures.
5. What clinical improvements were observed after SCAP treatment?
Twelve weeks after treatment, animals that received SCAP injections showed significant improvements in key periodontal parameters compared with the control group. The probing depth decreased from 7.33 mm to 5.44 mm, and attachment loss improved from 9.44 mm to 7.78 mm. These improvements indicate enhanced healing and regeneration of the supporting structures around the teeth.
6. Did SCAPs promote bone regeneration in periodontal defects?
Yes. Three-dimensional CT scans demonstrated significantly greater alveolar bone regeneration in the SCAP-treated group. Quantitative analysis showed approximately 22.73 mm³ of new bone formation compared with 9.87 mm³ in the control group treated with saline alone. This suggests that SCAP therapy can stimulate substantial bone regeneration in periodontal defects.
7. What did histological analysis reveal about periodontal tissue regeneration?
Microscopic histological examination revealed clear differences between treated and untreated defects. In the SCAP-treated sites, researchers observed new periodontal ligament formation, newly formed Sharpey’s fibers, thicker regenerated cementum, and reduced inflammatory infiltration. In contrast, untreated sites showed persistent periodontal pockets, inflammatory cells, and little evidence of structural regeneration.
8. How does SCAP therapy compare with other stem cell therapies in dentistry?
SCAPs have several advantages compared with other mesenchymal stem cells used in dentistry. Compared with bone marrow mesenchymal stem cells (BMMSCs), SCAPs are easier to obtain and show higher proliferation rates. Compared with PDLSCs and DPSCs, SCAPs exhibit greater differentiation capacity and mineralization potential. These advantages make SCAPs a highly promising cell source for periodontal tissue engineering.
9. Why is local cell injection considered a useful technique for periodontal regeneration?
Traditional stem cell-based regenerative approaches often rely on scaffolds or surgical transplantation procedures, which may involve complications such as immune reactions or surgical trauma. Local injection of stem cells provides a minimally invasive alternative that allows cells to be delivered directly into periodontal defects. This technique simplifies the treatment process and may improve clinical feasibility in future regenerative periodontal therapies.
10. Can SCAP-based therapies become a future treatment for periodontitis?
Current evidence from preclinical studies suggests that SCAP therapy has significant potential for regenerative periodontal treatment. Their strong regenerative capacity, immunomodulatory properties, and accessibility from extracted teeth make them an attractive therapeutic option. However, before widespread clinical adoption, further human clinical trials, safety assessments, and standardized treatment protocols will be necessary to confirm their effectiveness in routine periodontal therapy.
Reference:
Recent Articles
Introduction
Periodontitis remains one of the most prevalent chronic inflammatory diseases affecting the oral cavity. Characterized by progressive destruction of the periodontal ligament, cementum, gingiva, and alveolar bone, the disease ultimately leads to tooth mobility and tooth loss if left untreated. Conventional periodontal therapies—such as scaling and root planing, surgical flap procedures, and regenerative grafting techniques—aim to control infection and repair damaged tissues. However, complete regeneration of the periodontal apparatus remains difficult to achieve with traditional methods.
In recent years, regenerative dentistry has focused on the use of mesenchymal stem cells (MSCs) as a promising therapeutic approach. Among various MSC sources, Stem Cells from Apical Papilla (SCAPs) have emerged as a particularly promising candidate for periodontal tissue regeneration. These cells originate from the apical papilla of immature permanent teeth and exhibit remarkable proliferative and differentiation capabilities.
Recent experimental research suggests that local injection of SCAPs can significantly improve periodontal tissue regeneration, including alveolar bone formation, periodontal ligament restoration, and cementum regeneration. This article explores the biological properties of SCAPs, their advantages over other stem cell sources, and the experimental evidence supporting their use in treating periodontitis.
Understanding Stem Cells from Apical Papilla (SCAPs)
Stem Cells from Apical Papilla are a specialized type of dental-derived mesenchymal stem cell located in the apical papilla tissue of immature permanent teeth, particularly developing third molars.
The apical papilla is a soft tissue structure located at the root apex during tooth development. It plays a critical role in root formation and contains highly undifferentiated cells capable of extensive proliferation and differentiation.
SCAPs possess several defining biological characteristics:
High proliferative capacity
Strong osteogenic and odontogenic differentiation potential
Ability to form dentin-like structures
Immunomodulatory properties
Capability to generate pulp-like tissues
These properties make SCAPs particularly suitable for regenerative dental therapies, including pulp regeneration, bone regeneration, and periodontal tissue engineering.
Compared to other dental stem cells, such as:
Periodontal ligament stem cells (PDLSCs)
Dental pulp stem cells (DPSCs)
SCAPs demonstrate higher proliferation rates and greater mineralization potential, making them highly attractive for regenerative applications.
Periodontitis and the Need for Regenerative Therapies
Periodontitis is a complex disease driven by microbial biofilms and host immune responses. Over time, chronic inflammation leads to the progressive destruction of supporting structures around the tooth, including:
Alveolar bone
Periodontal ligament
Cementum
Gingival connective tissue
Traditional periodontal treatments focus on:
Eliminating infection
Reducing inflammation
Preventing further tissue destruction
However, true regeneration of the entire periodontal apparatus remains challenging.
Regenerative procedures such as:
Guided tissue regeneration (GTR)
Bone grafting
Enamel matrix derivatives
can stimulate partial regeneration, but the results are often inconsistent.
Stem cell-based therapies represent a biological solution capable of restoring the lost architecture of periodontal tissues through cellular regeneration rather than simple repair.
Advantages of SCAPs for Periodontal Regeneration
SCAPs offer several advantages compared with other stem cell sources used in periodontal regeneration.
1. High Proliferation Rate
SCAPs show greater population-doubling capacity than many other dental stem cells. This high proliferative ability allows for efficient expansion in laboratory culture before therapeutic use.
2. Strong Osteogenic Potential
Studies have demonstrated that SCAPs exhibit strong osteogenic and dentinogenic differentiation, meaning they can readily form:
Bone tissue
Dentin-like structures
Cementum-like tissue
These properties are essential for reconstructing the complex structure of periodontal tissues.
3. Accessibility of the Cell Source
SCAPs can be obtained from extracted immature wisdom teeth, which are frequently removed in routine dental procedures. This provides an accessible and minimally invasive source of stem cells.
4. Immunomodulatory Effects
SCAPs also demonstrate immunosuppressive properties, particularly by suppressing T-cell proliferation. This feature may reduce immune rejection and allow for allogeneic transplantation in future clinical applications.
5. Enhanced Regenerative Potential
Compared with bone marrow mesenchymal stem cells (BMMSCs), SCAPs demonstrate:
Comparable osteogenic differentiation
Higher proliferation rates
Easier isolation
These advantages make SCAPs an attractive cell source for periodontal tissue engineering.
Experimental Study: SCAPs in Periodontitis Treatment
To evaluate the regenerative potential of SCAPs in periodontal defects, researchers conducted a controlled experimental study using minipig models of periodontitis. Swine are frequently used in dental research because their periodontal anatomy closely resembles that of humans.
Creation of Periodontal Defects
Researchers surgically created standardized periodontal defects measuring:
3 mm width
5 mm depth
7 mm length
These defects were generated near the mandibular first molars of six miniature pigs to simulate advanced periodontitis.
After four weeks, the animals were divided into two groups:
Control Group: Received injections of saline solution (0.9% NaCl)
SCAP Treatment Group: Received injections of SCAPs suspended in saline
Each treatment site received approximately 2 × 10⁶ SCAP cells, injected subperiosteally around the periodontal defect.
The regenerative outcomes were evaluated 12 weeks after treatment using clinical measurements, CT imaging, and histological analysis.
Clinical Improvements After SCAP Treatment
Clinical periodontal parameters showed significant improvement in the SCAP-treated sites.
Probing Depth Reduction
Probing depth (PD) decreased significantly in the SCAP group:
SCAP group: 5.44 ± 0.77 mm
Control group: 7.33 ± 1.0 mm
This reduction indicates improved periodontal attachment and reduced pocket depth.
Attachment Loss Improvement
Attachment loss (AL) also improved significantly:
SCAP group: 7.78 ± 0.84 mm
Control group: 9.44 ± 1.07 mm
These results demonstrate that SCAP therapy helped restore periodontal attachment structures.
Gingival Recession
Interestingly, gingival recession showed no statistically significant difference between the groups, suggesting that SCAPs primarily affected deeper periodontal structures rather than superficial gingival position.
Overall, these findings indicate that SCAP injection promotes functional periodontal recovery.
CT Evidence of Alveolar Bone Regeneration
Three-dimensional CT imaging provided strong evidence of significant alveolar bone regeneration in the SCAP-treated sites.
Quantitative analysis revealed:
SCAP group bone regeneration: 22.73 ± 4.94 mm³
Control group bone regeneration: 9.87 ± 3.53 mm³
This represents a substantial increase in newly formed bone volume in the SCAP group.
Three-dimensional reconstructions demonstrated that SCAP treatment produced nearly complete regeneration of the alveolar bone defect, while the control group showed only limited bone formation.
These findings highlight the strong osteogenic capacity of SCAPs in periodontal regeneration.
Histological Evidence of Periodontal Tissue Regeneration
Histopathological examination further confirmed the regenerative potential of SCAP therapy.
In the control group, typical features of periodontitis were still present, including:
Deep periodontal pockets
Inflammatory cell infiltration
Absence of an organized periodontal ligament
Lack of Sharpey’s fibers
In contrast, the SCAP-treated group showed remarkable regeneration, including:
Formation of new periodontal ligament fibers
Presence of Sharpey’s fibers
Reduced inflammatory infiltration
Formation of thicker and more mature cementum
Quantitative analysis revealed that newly formed cementum in the SCAP group was significantly thicker:
SCAP group: 158.1 ± 16.3 μm
Control group: 91.4 ± 7.9 μm
These histological findings confirm that SCAP therapy can regenerate multiple components of the periodontal complex, including bone, ligament, and cementum.
Minimally Invasive Delivery via Local Injection
One particularly important aspect of this study was the delivery technique used for SCAP therapy.
Traditional stem cell-based tissue engineering often requires:
Biomaterial scaffolds
Surgical flap procedures
Complex transplantation methods
However, this study utilized simple local cell injection, which offers several advantages:
Minimally invasive procedure
Reduced surgical trauma
Faster clinical application
Lower cost and complexity
The results demonstrate that cell injection alone can effectively stimulate periodontal regeneration, making the approach highly attractive for future clinical therapies.
Future Perspectives in Periodontal Regenerative Medicine
Although the experimental results are promising, further research is necessary before SCAP therapy becomes widely available in clinical practice.
Future studies will likely focus on:
Understanding the Regenerative Mechanisms
Researchers still need to fully understand how SCAPs mediate tissue regeneration, including their interactions with:
Host cells
Growth factors
Immune responses
Extracellular matrix components
Combining SCAPs with Growth Factors
Combining SCAPs with bioactive molecules such as:
BMPs
VEGF
PDGF
may further enhance regenerative outcomes.
Gene Modification Strategies
Gene-editing techniques could improve SCAP survival, proliferation, and differentiation in periodontal defects.
Clinical Trials
Human clinical trials will be essential to confirm the safety and effectiveness of SCAP-based therapies in treating periodontal disease.
Conclusion
Stem Cells from the apical papilla represent one of the most promising tools in periodontal regenerative medicine. Their high proliferative capacity, strong osteogenic potential, and immunomodulatory properties make them ideal candidates for regenerating damaged periodontal tissues.
Experimental research in animal models demonstrates that local injection of SCAPs can significantly improve periodontal healing, promoting regeneration of alveolar bone, periodontal ligament, and cementum. Clinical parameters such as probing depth and attachment loss also show significant improvement following treatment.
Perhaps most importantly, SCAP therapy can be delivered through minimally invasive injection techniques, which may simplify future clinical applications.
As research in regenerative dentistry continues to advance, SCAP-based therapies may soon offer a biological solution for restoring periodontal tissues, potentially transforming the way clinicians treat advanced periodontitis.
FAQ: Stem Cells from Apical Papilla in Treating Periodontitis
1. What are Stem Cells from Apical Papilla (SCAPs)?
Stem Cells from Apical Papilla (SCAPs) are a type of dental-derived mesenchymal stem cell located in the apical papilla, the soft tissue found at the tip of developing tooth roots. These cells are typically harvested from immature wisdom teeth that are extracted for clinical reasons. SCAPs possess strong regenerative capabilities, including the ability to proliferate rapidly and differentiate into various cell types such as odontoblast-like cells, bone-forming cells, and periodontal ligament cells. Because of these properties, SCAPs are considered promising candidates for regenerative dentistry, particularly for rebuilding tissues destroyed by periodontitis.
2. Why are SCAPs considered promising for periodontal regeneration?
SCAPs demonstrate several biological advantages compared with other dental stem cells. Research shows they have higher proliferation rates, stronger mineralization capacity, and greater osteogenic differentiation potential than periodontal ligament stem cells (PDLSCs) and dental pulp stem cells (DPSCs). These characteristics allow them to contribute effectively to the regeneration of alveolar bone, cementum, and periodontal ligament, which are the key tissues damaged in periodontitis.
3. How are SCAPs obtained for research or therapeutic use?
SCAPs are typically isolated from the apical papilla tissue of immature third molars (wisdom teeth). After extraction, the apical papilla is carefully separated from the root tip and enzymatically digested to release the stem cells. The cells are then cultured in specialized growth media under controlled laboratory conditions. In the referenced study, SCAPs were expanded in culture and used between passages 3–5 for experimental periodontal regeneration.
4. How were SCAPs used to treat periodontitis in the study?
In the study model, periodontitis defects were surgically created in miniature pigs to simulate periodontal tissue destruction. Researchers treated these defects by locally injecting SCAPs suspended in saline solution into the tissues surrounding the periodontal defect. The injections were delivered at three points around each defect—mesial, distal, and central areas—allowing the stem cells to interact directly with the damaged periodontal structures.
5. What clinical improvements were observed after SCAP treatment?
Twelve weeks after treatment, animals that received SCAP injections showed significant improvements in key periodontal parameters compared with the control group. The probing depth decreased from 7.33 mm to 5.44 mm, and attachment loss improved from 9.44 mm to 7.78 mm. These improvements indicate enhanced healing and regeneration of the supporting structures around the teeth.
6. Did SCAPs promote bone regeneration in periodontal defects?
Yes. Three-dimensional CT scans demonstrated significantly greater alveolar bone regeneration in the SCAP-treated group. Quantitative analysis showed approximately 22.73 mm³ of new bone formation compared with 9.87 mm³ in the control group treated with saline alone. This suggests that SCAP therapy can stimulate substantial bone regeneration in periodontal defects.
7. What did histological analysis reveal about periodontal tissue regeneration?
Microscopic histological examination revealed clear differences between treated and untreated defects. In the SCAP-treated sites, researchers observed new periodontal ligament formation, newly formed Sharpey’s fibers, thicker regenerated cementum, and reduced inflammatory infiltration. In contrast, untreated sites showed persistent periodontal pockets, inflammatory cells, and little evidence of structural regeneration.
8. How does SCAP therapy compare with other stem cell therapies in dentistry?
SCAPs have several advantages compared with other mesenchymal stem cells used in dentistry. Compared with bone marrow mesenchymal stem cells (BMMSCs), SCAPs are easier to obtain and show higher proliferation rates. Compared with PDLSCs and DPSCs, SCAPs exhibit greater differentiation capacity and mineralization potential. These advantages make SCAPs a highly promising cell source for periodontal tissue engineering.
9. Why is local cell injection considered a useful technique for periodontal regeneration?
Traditional stem cell-based regenerative approaches often rely on scaffolds or surgical transplantation procedures, which may involve complications such as immune reactions or surgical trauma. Local injection of stem cells provides a minimally invasive alternative that allows cells to be delivered directly into periodontal defects. This technique simplifies the treatment process and may improve clinical feasibility in future regenerative periodontal therapies.
10. Can SCAP-based therapies become a future treatment for periodontitis?
Current evidence from preclinical studies suggests that SCAP therapy has significant potential for regenerative periodontal treatment. Their strong regenerative capacity, immunomodulatory properties, and accessibility from extracted teeth make them an attractive therapeutic option. However, before widespread clinical adoption, further human clinical trials, safety assessments, and standardized treatment protocols will be necessary to confirm their effectiveness in routine periodontal therapy.
Reference:
Recent Articles
Pulsed Electromagnetic Field (PEMF) Use in Implant Dentistry
Pulsed Electromagnetic Field (PEMF) Use in Implant Dentistry Abstract and Historical Background Pulsed Electromagnetic Field (PEMF) therapy refers to the application of low-frequency electromagnetic [...]
Laser Therapy in the Management of Peri-Implantitis
Laser Therapy in the Management of Peri-Implantitis Laser technology has become an increasingly valuable adjunct in the treatment of peri-implant diseases, particularly peri-implantitis. Its [...]
Magnetically Guided Dental Nanobots (CalBots) Are Real
Magnetically Guided Dental Nanobots (CalBots) Are Real The concept of nanobots in dentistry has long been associated with futuristic speculation. However, recent peer-reviewed research [...]
Peri-Implantitis Treatment & Prevention Methods
Peri-Implantitis Treatment & Prevention Methods Peri-implantitis remains one of the most significant biological complications affecting dental implants, posing a serious threat to long-term implant [...]
Latest Sinus Lifting Techniques in Modern Implant Dentistry
Latest Sinus Lifting Techniques in Modern Implant Dentistry A Comprehensive Clinical Review Introduction to Sinus Lifting in Implantology Sinus lifting, or maxillary sinus floor [...]
Biomechanics of the Triple Abutment & BOPiT Concept
Dental Biomechanics · Implant Science · Clinical Evidence Biomechanics of the Triple Abutment & BOPiT Concept How a saddle-shaped mathematical surface is rewriting the rules of load distribution [...]