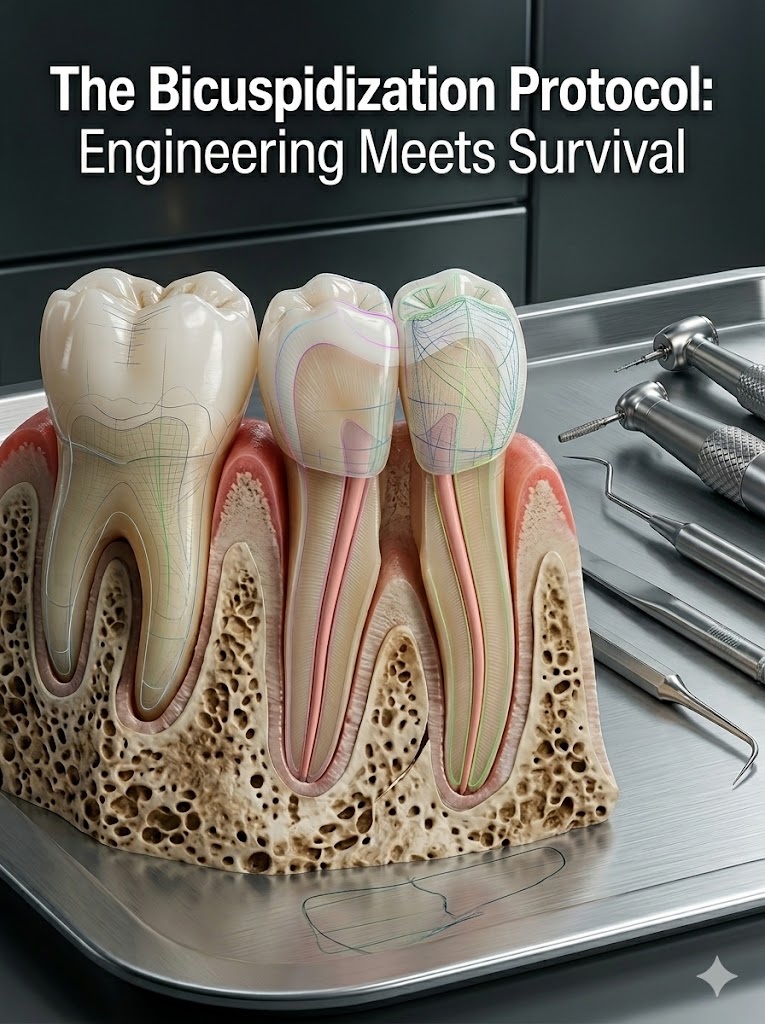
The Bicuspidization Protocol: Engineering Meets Survival
Modern restorative dentistry is no longer limited to extraction and replacement. In the era of conservative and biologically driven treatment planning, clinicians are increasingly focused on preserving natural dentition whenever possible. One of the most advanced examples of this philosophy is bicuspidization, a highly specialized procedure that transforms a compromised molar into two independent functional units. Rather than viewing severe furcation involvement as the inevitable end of a tooth, bicuspidization reframes the problem as a biomechanical engineering challenge.
The bicuspidization protocol combines surgical precision, endodontic expertise, and prosthetic rehabilitation into one coordinated treatment approach. Although technically demanding, the procedure offers a valuable option for preserving strategic molars that would otherwise be extracted. For patients, this means maintaining alveolar bone, preserving occlusal stability, and avoiding more invasive prosthetic alternatives such as implants or bridges.
As periodontal disease, root anatomy complications, and structural fractures continue to challenge clinicians worldwide, bicuspidization stands at the intersection of science, innovation, and survival. Understanding when and how to apply this protocol is essential for modern restorative and periodontal practitioners.
Understanding Bicuspidization and Its Clinical Philosophy
Bicuspidization is a surgical and restorative dental procedure in which a mandibular molar is divided into two separate sections, allowing each root and its corresponding crown portion to function independently. The concept is rooted in the preservation of natural tooth structure, particularly in cases where furcation involvement has compromised the integrity of the tooth but individual roots remain healthy enough to support function.
The procedure is most commonly indicated in mandibular molars with Grade II or Grade III furcation involvement. Instead of extracting the tooth entirely, the clinician strategically separates the mesial and distal roots. Once divided, each segment can receive independent restorative treatment, effectively converting one failing molar into two premolar-like units.
The philosophy behind bicuspidization is deeply connected to minimally invasive dentistry and long-term biomechanical preservation. Extraction often leads to alveolar bone resorption, occlusal instability, drifting of adjacent teeth, and the need for complex prosthetic rehabilitation. By preserving viable root structures, clinicians maintain periodontal ligament function and distribute occlusal forces more naturally.
Successful bicuspidization depends heavily on proper case selection. Teeth with adequate root divergence, sufficient bone support, and manageable periodontal defects tend to demonstrate the best long-term outcomes. Conversely, fused roots, severe mobility, or vertical root fractures significantly reduce the prognosis.
Clinicians increasingly recognize that bicuspidization is not merely a salvage procedure. Instead, it represents a sophisticated interdisciplinary solution that integrates periodontics, endodontics, and prosthodontics into one comprehensive protocol. This engineering-oriented perspective transforms tooth preservation into a calculated structural reconstruction rather than a temporary compromise.
Furcation Involvement: The Structural Crisis Behind the Procedure
Furcation involvement represents one of the most difficult periodontal challenges in clinical dentistry. The furcation area, where the roots of a multirooted tooth diverge, is anatomically complex and notoriously difficult to clean or restore once disease progression occurs. When periodontal destruction extends into this region, traditional scaling and root planing often become insufficient.
In mandibular molars, furcation defects can rapidly compromise tooth stability because the loss of supporting bone weakens the structural integrity of the tooth. Plaque accumulation, calculus retention, and bacterial colonization accelerate tissue breakdown in these inaccessible areas. As attachment loss increases, patients frequently experience mobility, food impaction, chronic inflammation, and recurrent periodontal abscesses.
Bicuspidization directly addresses this structural crisis by eliminating the furcation as a plaque-retentive anatomical problem. Once the molar is separated into two units, each root can be independently maintained through improved oral hygiene access. This dramatically changes the periodontal prognosis in selected cases.
However, the decision to proceed with bicuspidization requires careful diagnostic analysis. Cone beam computed tomography, periodontal charting, vitality testing, and occlusal evaluation all contribute to determining whether the tooth is restorable. The remaining bone support around each root must be sufficient to withstand functional forces after separation.
Root morphology also plays a critical role. Widely separated roots with minimal curvature provide better surgical accessibility and prosthetic adaptability. Additionally, crown-root ratio becomes a major determinant of long-term survival. If one root demonstrates significantly compromised support, hemisection or extraction of the weaker root may be more appropriate than full bicuspidization.
Ultimately, furcation involvement should not automatically condemn a molar to extraction. With appropriate diagnosis and interdisciplinary coordination, clinicians can transform a structurally compromised tooth into a maintainable and functional restorative solution.
Strategic Hemisection: Surgical Precision in Tooth Division
The surgical phase of bicuspidization begins with strategic hemisection, a delicate procedure requiring exceptional precision and anatomical awareness. During this stage, the clinician divides the molar crown and root complex into two independent segments while preserving maximum periodontal support and minimizing trauma to surrounding tissues.
Preoperative planning is critical for success. Radiographic analysis helps determine root anatomy, root divergence, and the extent of furcation destruction. Local anesthesia is administered, and a full-thickness flap may be reflected to improve visibility and access. Using a long-shank fissure bur under copious irrigation, the tooth is sectioned vertically through the occlusal table and furcation area.
The goal is to create complete separation without damaging adjacent root surfaces or compromising remaining bone. Precision during sectioning directly affects the long-term prognosis because uneven cuts or excessive removal of tooth structure can weaken the resulting segments.
Once separation is complete, the clinician carefully evaluates each root for stability and periodontal viability. Granulation tissue within the furcation defect is removed, and root surfaces are thoroughly debrided. Odontoplasty may also be performed to smooth irregular surfaces and facilitate plaque control.
Occlusal adjustment becomes especially important after hemisection. Excessive occlusal forces can overload the separated units, increasing the risk of fracture or mobility. Selective grinding helps redistribute functional stress and improve biomechanical balance.
Surgical success depends not only on technical execution but also on understanding force distribution within the masticatory system. The separated roots must function harmoniously within the occlusal scheme while maintaining periodontal stability. This is where dental surgery begins to resemble structural engineering, requiring careful planning of load-bearing dynamics and long-term functional integrity.
Endodontic Excellence and Root Canal Integrity
Endodontic treatment is one of the most important components of the bicuspidization protocol. Since each root becomes an independent functional unit after separation, successful root canal therapy is essential to ensure long-term survival and prevent reinfection.
In most cases, endodontic treatment is completed before the surgical phase. This allows the clinician to establish complete canal disinfection and hermetic obturation prior to sectioning the tooth. Preoperative endodontic planning also reduces contamination risks during surgery.
Cleaning and shaping procedures must account for the anatomical complexity commonly found in mandibular molars. Accessory canals, isthmuses, and apical ramifications can compromise treatment outcomes if inadequately disinfected. Modern rotary instrumentation systems, ultrasonic irrigation, and enhanced magnification significantly improve procedural accuracy.
The quality of obturation directly influences prognosis. Any microleakage within the root canal system can lead to persistent infection and eventual failure of the separated segments. Thermoplasticized gutta-percha techniques and bioceramic sealers are increasingly preferred because they provide superior adaptation and sealing properties.
Following hemisection, the exposed cut surfaces require careful management to prevent bacterial infiltration. Restorative sealing materials and core buildups must provide adequate structural reinforcement while protecting endodontic integrity.
Endodontic considerations also extend to biomechanical stability. Excessive removal of dentin during instrumentation can weaken the remaining root structure and increase fracture susceptibility. Conservative shaping techniques therefore play a crucial role in preserving root strength.
When executed properly, endodontic therapy transforms compromised roots into stable foundations capable of supporting independent restorations. This stage exemplifies the interdisciplinary nature of bicuspidization, where microscopic precision and restorative foresight work together to preserve long-term function.
Prosthetic Rehabilitation and Occlusal Engineering
After successful surgical and endodontic management, prosthetic rehabilitation becomes the final stage in restoring function and aesthetics. This phase requires careful occlusal engineering because the separated roots must now behave as independent restorative units capable of withstanding masticatory forces.
Individual crowns are typically fabricated for each section of the bicuspidized molar. These restorations must provide adequate retention, proper marginal adaptation, and optimal contouring to facilitate hygiene maintenance. Overcontoured crowns can create plaque traps that compromise periodontal health, making restorative design critically important.
Occlusal adjustment is equally essential. Since the biomechanics of the tooth have fundamentally changed, force distribution must be carefully controlled. Heavy occlusal contacts, lateral interferences, or parafunctional loading can increase fracture risk and destabilize periodontal support.
Modern digital dentistry has significantly improved prosthetic precision in bicuspidization cases. Intraoral scanners, CAD/CAM systems, and digital occlusal analysis allow clinicians to create highly accurate restorations tailored to the patient’s functional dynamics. Zirconia and high-strength ceramic materials are frequently used because they combine durability with aesthetic performance.
Hygiene accessibility remains one of the primary goals of prosthetic design. The embrasure space between the separated units should allow patients to clean effectively using interdental brushes or floss. Poor hygiene access is one of the leading causes of long-term failure in bicuspidized teeth.
From an engineering perspective, prosthetic rehabilitation completes the transformation from failing molar to functional dual-unit system. Every contour, contact point, and occlusal surface contributes to the overall biomechanical balance of the restoration. This stage ultimately determines whether the tooth survives as a durable functional asset or fails under repetitive stress.
Long-Term Prognosis, Maintenance, and Clinical Survival Rates
The long-term success of bicuspidization depends on multiple biological and mechanical factors. While the procedure can produce excellent outcomes in carefully selected cases, it also requires continuous maintenance and patient compliance to ensure lasting stability.
Clinical studies have demonstrated favorable survival rates when periodontal support remains adequate and restorative principles are properly followed. Patients who maintain excellent oral hygiene and attend regular periodontal maintenance appointments generally experience significantly better outcomes than those with poor plaque control.
One of the primary advantages of bicuspidization is preservation of natural proprioception through the periodontal ligament. Unlike implants, preserved roots maintain sensory feedback mechanisms that help regulate occlusal forces during mastication. This contributes to improved functional adaptation and patient comfort.
However, complications can still occur. Root fracture, recurrent periodontal disease, secondary caries, and endodontic failure remain potential risks. Occlusal overload is particularly problematic in patients with bruxism or heavy parafunctional habits. Protective night guards are often recommended to reduce stress on the restored segments.
Regular radiographic monitoring is essential to evaluate bone levels, periodontal stability, and periapical health. Clinicians must also assess mobility, crown integrity, and occlusal wear during follow-up appointments.
Despite its complexity, bicuspidization remains an important treatment option in modern dentistry because it bridges the gap between extraction and full prosthetic replacement. For many patients, preserving a strategically important molar can delay or eliminate the need for implants while maintaining natural oral function.
The protocol ultimately represents a fusion of biology, mechanics, and restorative innovation. In the hands of skilled clinicians, bicuspidization demonstrates that even severely compromised teeth can survive through intelligent structural redesign and interdisciplinary collaboration.
Frequently Asked Questions About Bicuspidization
What is bicuspidization in dentistry?
Bicuspidization is a dental procedure in which a molar tooth is surgically divided into two separate functional units. It is commonly performed on mandibular molars with severe furcation involvement.
When is bicuspidization recommended?
The procedure is typically recommended when a molar has advanced furcation involvement but still possesses adequate root support and periodontal stability for long-term preservation.
Is bicuspidization better than extraction?
In selected cases, bicuspidization can preserve natural tooth structure, maintain bone support, and avoid more invasive restorative procedures such as implants or bridges.
How long does a bicuspidized tooth last?
With proper case selection, excellent oral hygiene, and regular dental maintenance, bicuspidized teeth can remain functional for many years.
Does bicuspidization require root canal treatment?
Yes. Endodontic therapy is usually necessary before the tooth is surgically divided to ensure each root remains infection-free and structurally stable.
What are the risks of bicuspidization?
Potential complications include root fracture, periodontal breakdown, occlusal overload, secondary caries, and endodontic failure if maintenance is inadequate.
Can bicuspidization be performed on upper molars?
Although possible in some cases, bicuspidization is more commonly performed on mandibular molars because their root anatomy is generally more favorable for separation.
Is bicuspidization painful?
The procedure is performed under local anesthesia, and postoperative discomfort is usually manageable with standard pain control measures and proper healing protocols.
References
- American Academy of Periodontology. Glossary of Periodontal Terms.
- Carranza FA, Newman MG. Clinical Periodontology. Elsevier.
- Cohen S, Hargreaves KM. Pathways of the Pulp. Mosby.
- Lindhe J, Lang NP. Clinical Periodontology and Implant Dentistry. Wiley-Blackwell.
- Shillingburg HT. Fundamentals of Fixed Prosthodontics. Quintessence Publishing.
- Grossman LI. Endodontic Practice. Lea & Febiger.
- Peeran SW, et al. Hemisection and bicuspidization in restorative dentistry: A clinical review.
- Park SY, et al. Long-term outcomes of root resection therapy in molars with furcation involvement.
Recent Articles
Modern restorative dentistry is no longer limited to extraction and replacement. In the era of conservative and biologically driven treatment planning, clinicians are increasingly focused on preserving natural dentition whenever possible. One of the most advanced examples of this philosophy is bicuspidization, a highly specialized procedure that transforms a compromised molar into two independent functional units. Rather than viewing severe furcation involvement as the inevitable end of a tooth, bicuspidization reframes the problem as a biomechanical engineering challenge.
The bicuspidization protocol combines surgical precision, endodontic expertise, and prosthetic rehabilitation into one coordinated treatment approach. Although technically demanding, the procedure offers a valuable option for preserving strategic molars that would otherwise be extracted. For patients, this means maintaining alveolar bone, preserving occlusal stability, and avoiding more invasive prosthetic alternatives such as implants or bridges.
As periodontal disease, root anatomy complications, and structural fractures continue to challenge clinicians worldwide, bicuspidization stands at the intersection of science, innovation, and survival. Understanding when and how to apply this protocol is essential for modern restorative and periodontal practitioners.
Understanding Bicuspidization and Its Clinical Philosophy
Bicuspidization is a surgical and restorative dental procedure in which a mandibular molar is divided into two separate sections, allowing each root and its corresponding crown portion to function independently. The concept is rooted in the preservation of natural tooth structure, particularly in cases where furcation involvement has compromised the integrity of the tooth but individual roots remain healthy enough to support function.
The procedure is most commonly indicated in mandibular molars with Grade II or Grade III furcation involvement. Instead of extracting the tooth entirely, the clinician strategically separates the mesial and distal roots. Once divided, each segment can receive independent restorative treatment, effectively converting one failing molar into two premolar-like units.
The philosophy behind bicuspidization is deeply connected to minimally invasive dentistry and long-term biomechanical preservation. Extraction often leads to alveolar bone resorption, occlusal instability, drifting of adjacent teeth, and the need for complex prosthetic rehabilitation. By preserving viable root structures, clinicians maintain periodontal ligament function and distribute occlusal forces more naturally.
Successful bicuspidization depends heavily on proper case selection. Teeth with adequate root divergence, sufficient bone support, and manageable periodontal defects tend to demonstrate the best long-term outcomes. Conversely, fused roots, severe mobility, or vertical root fractures significantly reduce the prognosis.
Clinicians increasingly recognize that bicuspidization is not merely a salvage procedure. Instead, it represents a sophisticated interdisciplinary solution that integrates periodontics, endodontics, and prosthodontics into one comprehensive protocol. This engineering-oriented perspective transforms tooth preservation into a calculated structural reconstruction rather than a temporary compromise.
Furcation Involvement: The Structural Crisis Behind the Procedure
Furcation involvement represents one of the most difficult periodontal challenges in clinical dentistry. The furcation area, where the roots of a multirooted tooth diverge, is anatomically complex and notoriously difficult to clean or restore once disease progression occurs. When periodontal destruction extends into this region, traditional scaling and root planing often become insufficient.
In mandibular molars, furcation defects can rapidly compromise tooth stability because the loss of supporting bone weakens the structural integrity of the tooth. Plaque accumulation, calculus retention, and bacterial colonization accelerate tissue breakdown in these inaccessible areas. As attachment loss increases, patients frequently experience mobility, food impaction, chronic inflammation, and recurrent periodontal abscesses.
Bicuspidization directly addresses this structural crisis by eliminating the furcation as a plaque-retentive anatomical problem. Once the molar is separated into two units, each root can be independently maintained through improved oral hygiene access. This dramatically changes the periodontal prognosis in selected cases.
However, the decision to proceed with bicuspidization requires careful diagnostic analysis. Cone beam computed tomography, periodontal charting, vitality testing, and occlusal evaluation all contribute to determining whether the tooth is restorable. The remaining bone support around each root must be sufficient to withstand functional forces after separation.
Root morphology also plays a critical role. Widely separated roots with minimal curvature provide better surgical accessibility and prosthetic adaptability. Additionally, crown-root ratio becomes a major determinant of long-term survival. If one root demonstrates significantly compromised support, hemisection or extraction of the weaker root may be more appropriate than full bicuspidization.
Ultimately, furcation involvement should not automatically condemn a molar to extraction. With appropriate diagnosis and interdisciplinary coordination, clinicians can transform a structurally compromised tooth into a maintainable and functional restorative solution.
Strategic Hemisection: Surgical Precision in Tooth Division
The surgical phase of bicuspidization begins with strategic hemisection, a delicate procedure requiring exceptional precision and anatomical awareness. During this stage, the clinician divides the molar crown and root complex into two independent segments while preserving maximum periodontal support and minimizing trauma to surrounding tissues.
Preoperative planning is critical for success. Radiographic analysis helps determine root anatomy, root divergence, and the extent of furcation destruction. Local anesthesia is administered, and a full-thickness flap may be reflected to improve visibility and access. Using a long-shank fissure bur under copious irrigation, the tooth is sectioned vertically through the occlusal table and furcation area.
The goal is to create complete separation without damaging adjacent root surfaces or compromising remaining bone. Precision during sectioning directly affects the long-term prognosis because uneven cuts or excessive removal of tooth structure can weaken the resulting segments.
Once separation is complete, the clinician carefully evaluates each root for stability and periodontal viability. Granulation tissue within the furcation defect is removed, and root surfaces are thoroughly debrided. Odontoplasty may also be performed to smooth irregular surfaces and facilitate plaque control.
Occlusal adjustment becomes especially important after hemisection. Excessive occlusal forces can overload the separated units, increasing the risk of fracture or mobility. Selective grinding helps redistribute functional stress and improve biomechanical balance.
Surgical success depends not only on technical execution but also on understanding force distribution within the masticatory system. The separated roots must function harmoniously within the occlusal scheme while maintaining periodontal stability. This is where dental surgery begins to resemble structural engineering, requiring careful planning of load-bearing dynamics and long-term functional integrity.
Endodontic Excellence and Root Canal Integrity
Endodontic treatment is one of the most important components of the bicuspidization protocol. Since each root becomes an independent functional unit after separation, successful root canal therapy is essential to ensure long-term survival and prevent reinfection.
In most cases, endodontic treatment is completed before the surgical phase. This allows the clinician to establish complete canal disinfection and hermetic obturation prior to sectioning the tooth. Preoperative endodontic planning also reduces contamination risks during surgery.
Cleaning and shaping procedures must account for the anatomical complexity commonly found in mandibular molars. Accessory canals, isthmuses, and apical ramifications can compromise treatment outcomes if inadequately disinfected. Modern rotary instrumentation systems, ultrasonic irrigation, and enhanced magnification significantly improve procedural accuracy.
The quality of obturation directly influences prognosis. Any microleakage within the root canal system can lead to persistent infection and eventual failure of the separated segments. Thermoplasticized gutta-percha techniques and bioceramic sealers are increasingly preferred because they provide superior adaptation and sealing properties.
Following hemisection, the exposed cut surfaces require careful management to prevent bacterial infiltration. Restorative sealing materials and core buildups must provide adequate structural reinforcement while protecting endodontic integrity.
Endodontic considerations also extend to biomechanical stability. Excessive removal of dentin during instrumentation can weaken the remaining root structure and increase fracture susceptibility. Conservative shaping techniques therefore play a crucial role in preserving root strength.
When executed properly, endodontic therapy transforms compromised roots into stable foundations capable of supporting independent restorations. This stage exemplifies the interdisciplinary nature of bicuspidization, where microscopic precision and restorative foresight work together to preserve long-term function.
Prosthetic Rehabilitation and Occlusal Engineering
After successful surgical and endodontic management, prosthetic rehabilitation becomes the final stage in restoring function and aesthetics. This phase requires careful occlusal engineering because the separated roots must now behave as independent restorative units capable of withstanding masticatory forces.
Individual crowns are typically fabricated for each section of the bicuspidized molar. These restorations must provide adequate retention, proper marginal adaptation, and optimal contouring to facilitate hygiene maintenance. Overcontoured crowns can create plaque traps that compromise periodontal health, making restorative design critically important.
Occlusal adjustment is equally essential. Since the biomechanics of the tooth have fundamentally changed, force distribution must be carefully controlled. Heavy occlusal contacts, lateral interferences, or parafunctional loading can increase fracture risk and destabilize periodontal support.
Modern digital dentistry has significantly improved prosthetic precision in bicuspidization cases. Intraoral scanners, CAD/CAM systems, and digital occlusal analysis allow clinicians to create highly accurate restorations tailored to the patient’s functional dynamics. Zirconia and high-strength ceramic materials are frequently used because they combine durability with aesthetic performance.
Hygiene accessibility remains one of the primary goals of prosthetic design. The embrasure space between the separated units should allow patients to clean effectively using interdental brushes or floss. Poor hygiene access is one of the leading causes of long-term failure in bicuspidized teeth.
From an engineering perspective, prosthetic rehabilitation completes the transformation from failing molar to functional dual-unit system. Every contour, contact point, and occlusal surface contributes to the overall biomechanical balance of the restoration. This stage ultimately determines whether the tooth survives as a durable functional asset or fails under repetitive stress.
Long-Term Prognosis, Maintenance, and Clinical Survival Rates
The long-term success of bicuspidization depends on multiple biological and mechanical factors. While the procedure can produce excellent outcomes in carefully selected cases, it also requires continuous maintenance and patient compliance to ensure lasting stability.
Clinical studies have demonstrated favorable survival rates when periodontal support remains adequate and restorative principles are properly followed. Patients who maintain excellent oral hygiene and attend regular periodontal maintenance appointments generally experience significantly better outcomes than those with poor plaque control.
One of the primary advantages of bicuspidization is preservation of natural proprioception through the periodontal ligament. Unlike implants, preserved roots maintain sensory feedback mechanisms that help regulate occlusal forces during mastication. This contributes to improved functional adaptation and patient comfort.
However, complications can still occur. Root fracture, recurrent periodontal disease, secondary caries, and endodontic failure remain potential risks. Occlusal overload is particularly problematic in patients with bruxism or heavy parafunctional habits. Protective night guards are often recommended to reduce stress on the restored segments.
Regular radiographic monitoring is essential to evaluate bone levels, periodontal stability, and periapical health. Clinicians must also assess mobility, crown integrity, and occlusal wear during follow-up appointments.
Despite its complexity, bicuspidization remains an important treatment option in modern dentistry because it bridges the gap between extraction and full prosthetic replacement. For many patients, preserving a strategically important molar can delay or eliminate the need for implants while maintaining natural oral function.
The protocol ultimately represents a fusion of biology, mechanics, and restorative innovation. In the hands of skilled clinicians, bicuspidization demonstrates that even severely compromised teeth can survive through intelligent structural redesign and interdisciplinary collaboration.
Frequently Asked Questions About Bicuspidization
What is bicuspidization in dentistry?
Bicuspidization is a dental procedure in which a molar tooth is surgically divided into two separate functional units. It is commonly performed on mandibular molars with severe furcation involvement.
When is bicuspidization recommended?
The procedure is typically recommended when a molar has advanced furcation involvement but still possesses adequate root support and periodontal stability for long-term preservation.
Is bicuspidization better than extraction?
In selected cases, bicuspidization can preserve natural tooth structure, maintain bone support, and avoid more invasive restorative procedures such as implants or bridges.
How long does a bicuspidized tooth last?
With proper case selection, excellent oral hygiene, and regular dental maintenance, bicuspidized teeth can remain functional for many years.
Does bicuspidization require root canal treatment?
Yes. Endodontic therapy is usually necessary before the tooth is surgically divided to ensure each root remains infection-free and structurally stable.
What are the risks of bicuspidization?
Potential complications include root fracture, periodontal breakdown, occlusal overload, secondary caries, and endodontic failure if maintenance is inadequate.
Can bicuspidization be performed on upper molars?
Although possible in some cases, bicuspidization is more commonly performed on mandibular molars because their root anatomy is generally more favorable for separation.
Is bicuspidization painful?
The procedure is performed under local anesthesia, and postoperative discomfort is usually manageable with standard pain control measures and proper healing protocols.
References
- American Academy of Periodontology. Glossary of Periodontal Terms.
- Carranza FA, Newman MG. Clinical Periodontology. Elsevier.
- Cohen S, Hargreaves KM. Pathways of the Pulp. Mosby.
- Lindhe J, Lang NP. Clinical Periodontology and Implant Dentistry. Wiley-Blackwell.
- Shillingburg HT. Fundamentals of Fixed Prosthodontics. Quintessence Publishing.
- Grossman LI. Endodontic Practice. Lea & Febiger.
- Peeran SW, et al. Hemisection and bicuspidization in restorative dentistry: A clinical review.
- Park SY, et al. Long-term outcomes of root resection therapy in molars with furcation involvement.
Recent Articles
Pulsed Electromagnetic Field (PEMF) Use in Implant Dentistry
Pulsed Electromagnetic Field (PEMF) Use in Implant Dentistry Abstract and Historical Background Pulsed Electromagnetic Field (PEMF) therapy refers to the application of low-frequency electromagnetic [...]
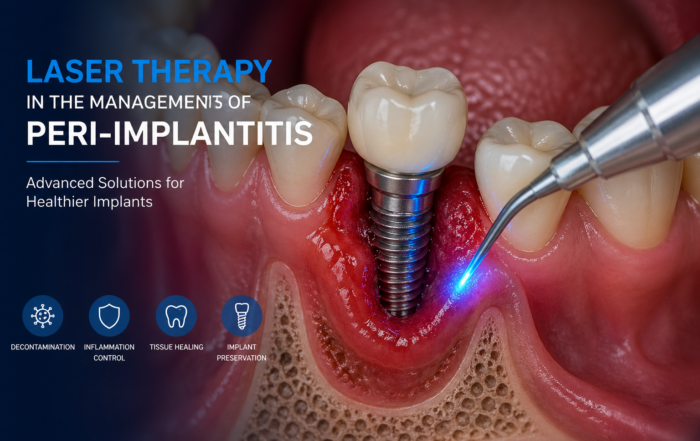
Laser Therapy in the Management of Peri-Implantitis
Laser Therapy in the Management of Peri-Implantitis Laser technology has become an increasingly valuable adjunct in the treatment of peri-implant diseases, particularly peri-implantitis. Its [...]
Magnetically Guided Dental Nanobots (CalBots) Are Real
Magnetically Guided Dental Nanobots (CalBots) Are Real The concept of nanobots in dentistry has long been associated with futuristic speculation. However, recent peer-reviewed research [...]
Peri-Implantitis Treatment & Prevention Methods
Peri-Implantitis Treatment & Prevention Methods Peri-implantitis remains one of the most significant biological complications affecting dental implants, posing a serious threat to long-term implant [...]
Latest Sinus Lifting Techniques in Modern Implant Dentistry
Latest Sinus Lifting Techniques in Modern Implant Dentistry A Comprehensive Clinical Review Introduction to Sinus Lifting in Implantology Sinus lifting, or maxillary sinus floor [...]
Biomechanics of the Triple Abutment & BOPiT Concept
Dental Biomechanics · Implant Science · Clinical Evidence Biomechanics of the Triple Abutment & BOPiT Concept How a saddle-shaped mathematical surface is rewriting the rules of load distribution [...]