Dental X-Rays and Brain Tumors
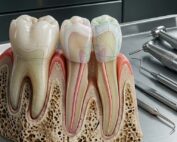
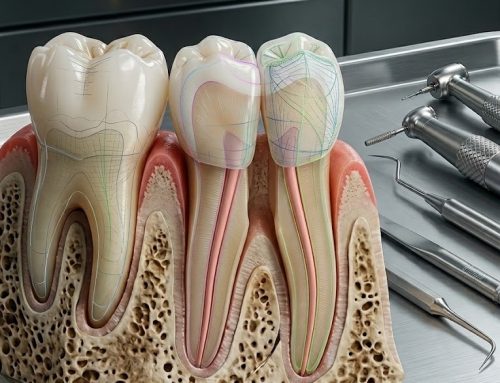
Dental radiography is a cornerstone of modern dentistry, enabling clinicians to diagnose caries, periodontal disease, and periapical pathology with precision. However, increasing public awareness about radiation exposure has raised a critical and often controversial question: Do dental X-rays and brain tumors have a direct connection?
With millions of patients undergoing dental imaging annually, understanding the radiation risk associated with dental X-rays is essential for both clinicians and patients. This article explores current evidence, examines the link with meningioma, and provides a balanced, evidence-based perspective.
Understanding Ionizing Radiation Exposure From Dental Imaging Procedures
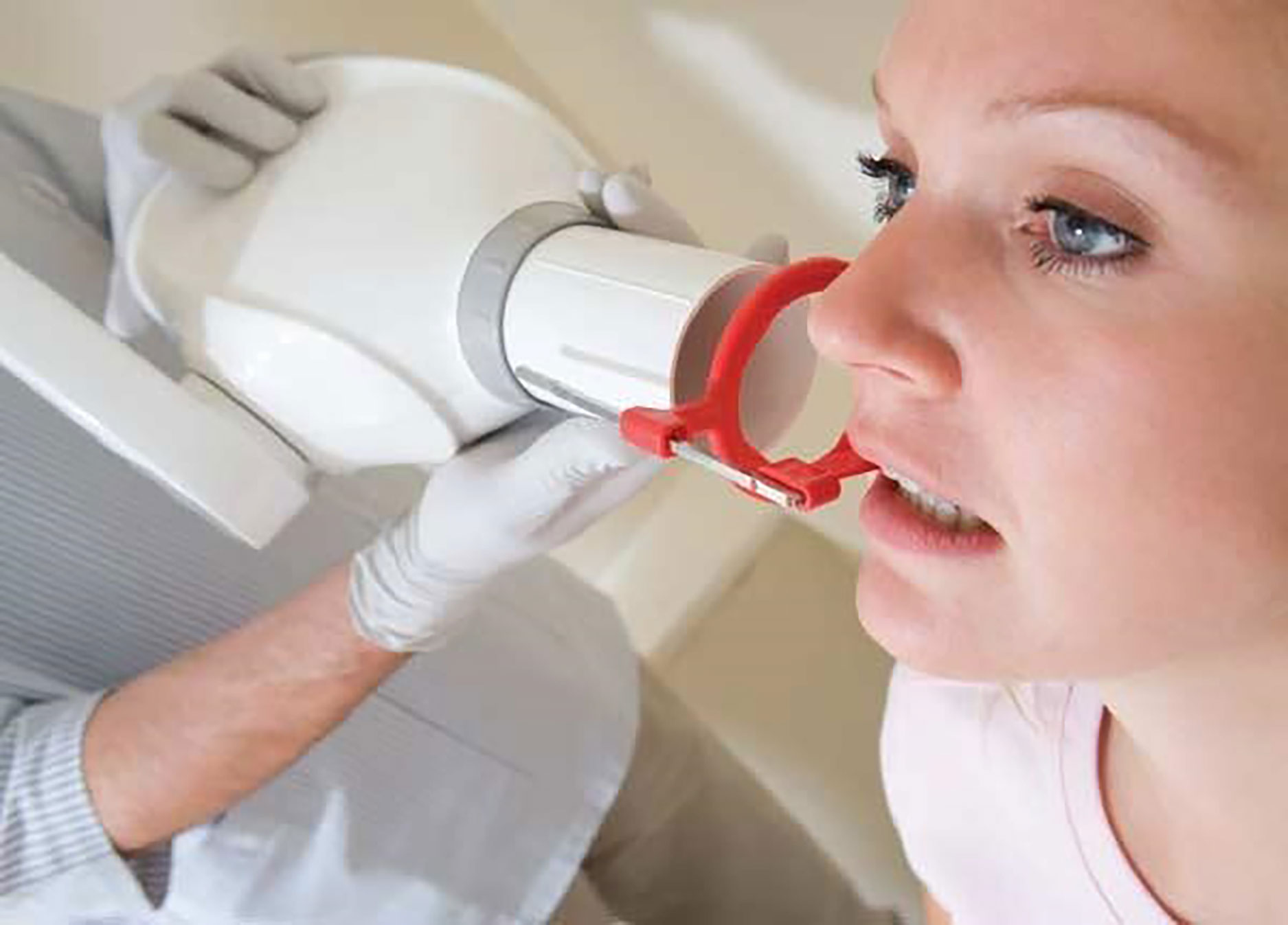
Dental X-rays are among the most common sources of artificial ionizing radiation in healthcare. In the United States alone, tens of millions of dental radiographs are taken annually, making them a significant contributor to cumulative radiation exposure.
Although the radiation risk from dental X-rays is relatively low compared to medical imaging such as CT scans, it is not entirely negligible. Bitewing, periapical, and panoramic radiographs all expose patients to small doses of ionizing radiation, which has the theoretical potential to damage DNA and increase cancer risk over time.
Protective measures such as lead aprons and thyroid collars are routinely used in dental practice to reduce exposure to vital organs. However, one important limitation remains: the brain is not directly shielded during most dental X-ray procedures. This has fueled ongoing debate about the possible relationship between dental X-rays and brain tumors, particularly in cases of repeated exposure over many years.
Epidemiological Evidence Linking Dental X-Rays And Brain Tumor Risk
A widely discussed epidemiological study examined the association between dental X-rays and brain tumors, focusing specifically on intracranial meningioma, the most common benign brain tumor.
The findings were notable:
- Individuals who had ever undergone bitewing dental X-rays showed approximately twice the odds of developing meningioma.
- Patients exposed to panoramic dental X-rays before the age of 10 demonstrated nearly a fivefold increase in risk.
These results sparked widespread concern regarding the long-term radiation risk of dental imaging, especially in children who are more sensitive to ionizing radiation.
However, while the association between dental X-rays and meningioma appears statistically significant, it is crucial to interpret these findings with caution and scientific rigor.

Correlation Versus Causation In Dental Radiology Risk Assessment Studies
One of the most important principles in epidemiology is distinguishing between correlation and causation. The observed relationship between dental X-rays and brain tumors does not necessarily mean that dental radiography directly causes tumor development.
Several alternative explanations must be considered:
- Reverse causation: Early symptoms of a brain tumor, such as facial pain or neurological discomfort, may lead patients to seek dental care, resulting in X-ray exposure.
- Confounding variables: Factors like genetics, environmental exposure, or prior medical conditions may influence both tumor risk and the likelihood of undergoing dental imaging.
- Recall bias: Patients diagnosed with meningioma may be more likely to remember or overreport previous exposure to dental X-rays.
Therefore, while the association exists, current evidence does not definitively prove that dental X-rays cause brain tumors.
Potential Confounding Factors Including Head Trauma And Diagnostic Bias
Another key factor complicating the relationship between dental X-rays and brain tumors is the presence of confounding variables such as head trauma.
Research suggests that childhood head injuries may increase the likelihood of developing brain tumors later in life. At the same time, dental trauma often requires radiographic evaluation, increasing exposure to dental X-rays.
This creates a dual pathway:
- Head trauma → Increased meningioma risk
- Head trauma → Increased need for dental X-rays
Without proper adjustment for these variables, studies may overestimate the role of dental radiography in tumor development.
Additionally, diagnostic bias may occur when symptomatic individuals undergo more frequent imaging, artificially inflating the association between radiation exposure and brain tumors.

Clinical Guidelines Emphasizing Judicious Use Of Dental Radiographic Imaging
Professional bodies such as the American Dental Association strongly emphasize a risk-based approach when prescribing dental X-rays.
Current guidelines clearly state that dentists should not recommend routine dental X-rays at fixed intervals for all patients, such as every six months or annually. Instead, imaging should be based on individual patient needs and clinical indications.
Key principles include:
- Avoid unnecessary exposure to ionizing radiation
- Prescribe X-rays only when they will influence diagnosis or treatment
- Evaluate patient-specific risk factors, including age and oral health status
This approach aligns with the ALARA principle (As Low As Reasonably Achievable), which is fundamental in minimizing radiation risk in dental practice.
Balancing Diagnostic Benefits Against Theoretical Radiation-Induced Risks Carefully
While concerns about dental X-rays and brain tumors are valid, it is equally important to recognize the substantial diagnostic benefits of dental radiography.
Dental X-rays play a critical role in detecting:
- Interproximal caries is not visible clinically
- Early bone loss associated with periodontal disease
- Impacted or unerupted teeth
- Periapical pathology and infections
Avoiding necessary imaging due to fear of radiation risk may lead to delayed diagnosis, more complex treatments, and poorer patient outcomes.
Thus, clinicians must carefully balance:
- Benefits: Accurate diagnosis and improved treatment outcomes
- Risks: Minimal but cumulative radiation exposure
When used appropriately, the benefits of dental X-rays far outweigh the potential risks.
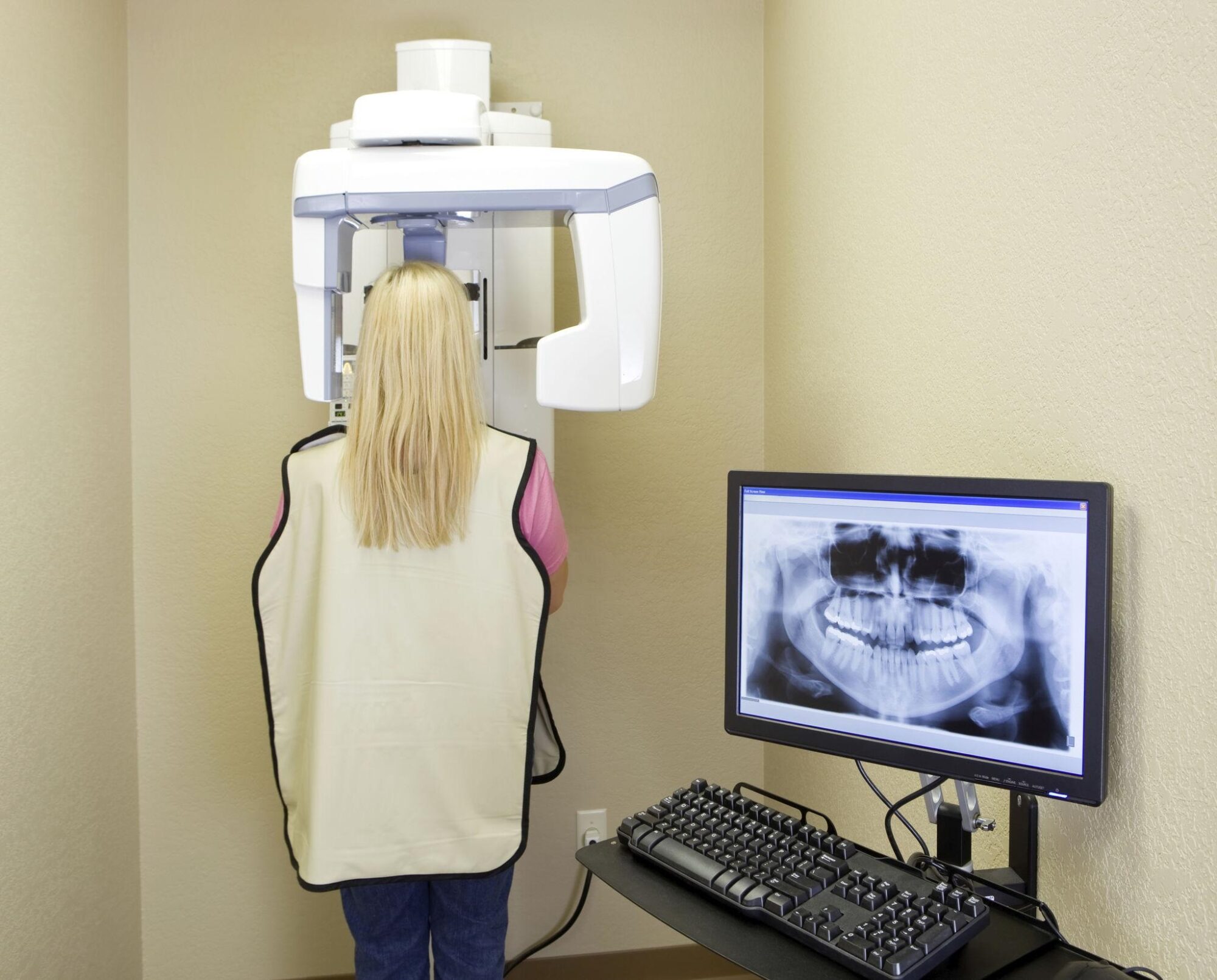
Modern Digital Radiography Significantly Reduces Radiation Dose To Patients
Advancements in dental technology have significantly reduced the radiation risk associated with dental X-rays.
Modern digital radiography systems offer:
- Up to 70–90% lower radiation doses compared to traditional film-based imaging
- Faster image acquisition, reducing exposure time
- Enhanced image clarity for improved diagnostic accuracy
In many cases, the radiation dose from a dental X-ray is comparable to the natural background radiation received in a single day.
These innovations further weaken the argument that dental X-rays significantly contribute to brain tumor risk, particularly when used responsibly.
Practical Recommendations For Dentists To Minimize Unnecessary Radiation Exposure
To ensure patient safety while maintaining diagnostic effectiveness, dental professionals should adopt best practices that minimize unnecessary radiation exposure.
Recommended strategies include:
- Perform thorough clinical examinations before prescribing imaging
- Use selective radiography based on patient-specific risk factors
- Prefer digital X-ray systems to reduce radiation dose
- Apply appropriate shielding techniques, including thyroid collars
- Educate patients about the realistic risks and benefits of dental X-rays
By following these principles, clinicians can reduce the potential link between dental X-rays and brain tumors while maintaining high standards of care.
Frequently Asked Questions About Dental X-Rays And Brain Tumors
1. Do dental X-rays cause brain tumors?
There is no conclusive evidence proving that dental X-rays directly cause brain tumors. Some studies show an association, but causation remains unproven.
2. What is the link between dental X-rays and meningioma?
Certain studies suggest an increased association between dental X-rays and meningioma, but confounding factors make it difficult to establish a direct causal relationship.
3. Are dental X-rays safe for children?
Yes, when used appropriately. However, children are more sensitive to radiation, so imaging should be carefully justified.
4. How can radiation risk from dental X-rays be minimized?
Radiation risk can be reduced by limiting unnecessary imaging, using digital systems, and following ALARA principles.
5. Do lead aprons protect the brain during dental X-rays?
No, lead aprons protect the body but do not shield the brain, which remains exposed during imaging.
6. Should patients avoid dental X-rays due to fear of cancer؟
No, it is not recommended to avoid dental X-rays when they are needed, because the diagnostic benefits significantly outweigh the potential risks.
Conclusion
The potential relationship between dental X-rays and brain tumors, particularly meningioma, remains an area of ongoing scientific investigation. While some studies indicate a statistical association, there is no definitive evidence establishing causation.
For dental professionals, the key lies in applying evidence-based clinical judgment, minimizing unnecessary radiation exposure, and ensuring that every radiograph has a clear diagnostic purpose.
Ultimately, responsible and selective use of dental X-rays—not avoidance—is the most effective strategy to balance patient safety with optimal clinical outcomes.
Reference:
Recent Articles
Dental radiography is a cornerstone of modern dentistry, enabling clinicians to diagnose caries, periodontal disease, and periapical pathology with precision. However, increasing public awareness about radiation exposure has raised a critical and often controversial question: Do dental X-rays and brain tumors have a direct connection?
With millions of patients undergoing dental imaging annually, understanding the radiation risk associated with dental X-rays is essential for both clinicians and patients. This article explores current evidence, examines the link with meningioma, and provides a balanced, evidence-based perspective.

Understanding Ionizing Radiation Exposure From Dental Imaging Procedures
Dental X-rays are among the most common sources of artificial ionizing radiation in healthcare. In the United States alone, tens of millions of dental radiographs are taken annually, making them a significant contributor to cumulative radiation exposure.
Although the radiation risk from dental X-rays is relatively low compared to medical imaging such as CT scans, it is not entirely negligible. Bitewing, periapical, and panoramic radiographs all expose patients to small doses of ionizing radiation, which has the theoretical potential to damage DNA and increase cancer risk over time.
Protective measures such as lead aprons and thyroid collars are routinely used in dental practice to reduce exposure to vital organs. However, one important limitation remains: the brain is not directly shielded during most dental X-ray procedures. This has fueled ongoing debate about the possible relationship between dental X-rays and brain tumors, particularly in cases of repeated exposure over many years.
Epidemiological Evidence Linking Dental X-Rays And Brain Tumor Risk
A widely discussed epidemiological study examined the association between dental X-rays and brain tumors, focusing specifically on intracranial meningioma, the most common benign brain tumor.
The findings were notable:
- Individuals who had ever undergone bitewing dental X-rays showed approximately twice the odds of developing meningioma.
- Patients exposed to panoramic dental X-rays before the age of 10 demonstrated nearly a fivefold increase in risk.
These results sparked widespread concern regarding the long-term radiation risk of dental imaging, especially in children who are more sensitive to ionizing radiation.
However, while the association between dental X-rays and meningioma appears statistically significant, it is crucial to interpret these findings with caution and scientific rigor.

Correlation Versus Causation In Dental Radiology Risk Assessment Studies
One of the most important principles in epidemiology is distinguishing between correlation and causation. The observed relationship between dental X-rays and brain tumors does not necessarily mean that dental radiography directly causes tumor development.
Several alternative explanations must be considered:
- Reverse causation: Early symptoms of a brain tumor, such as facial pain or neurological discomfort, may lead patients to seek dental care, resulting in X-ray exposure.
- Confounding variables: Factors like genetics, environmental exposure, or prior medical conditions may influence both tumor risk and the likelihood of undergoing dental imaging.
- Recall bias: Patients diagnosed with meningioma may be more likely to remember or overreport previous exposure to dental X-rays.
Therefore, while the association exists, current evidence does not definitively prove that dental X-rays cause brain tumors.
Potential Confounding Factors Including Head Trauma And Diagnostic Bias
Another key factor complicating the relationship between dental X-rays and brain tumors is the presence of confounding variables such as head trauma.
Research suggests that childhood head injuries may increase the likelihood of developing brain tumors later in life. At the same time, dental trauma often requires radiographic evaluation, increasing exposure to dental X-rays.
This creates a dual pathway:
- Head trauma → Increased meningioma risk
- Head trauma → Increased need for dental X-rays
Without proper adjustment for these variables, studies may overestimate the role of dental radiography in tumor development.
Additionally, diagnostic bias may occur when symptomatic individuals undergo more frequent imaging, artificially inflating the association between radiation exposure and brain tumors.

Clinical Guidelines Emphasizing Judicious Use Of Dental Radiographic Imaging
Professional bodies such as the American Dental Association strongly emphasize a risk-based approach when prescribing dental X-rays.
Current guidelines clearly state that dentists should not recommend routine dental X-rays at fixed intervals for all patients, such as every six months or annually. Instead, imaging should be based on individual patient needs and clinical indications.
Key principles include:
- Avoid unnecessary exposure to ionizing radiation
- Prescribe X-rays only when they will influence diagnosis or treatment
- Evaluate patient-specific risk factors, including age and oral health status
This approach aligns with the ALARA principle (As Low As Reasonably Achievable), which is fundamental in minimizing radiation risk in dental practice.
Balancing Diagnostic Benefits Against Theoretical Radiation-Induced Risks Carefully
While concerns about dental X-rays and brain tumors are valid, it is equally important to recognize the substantial diagnostic benefits of dental radiography.
Dental X-rays play a critical role in detecting:
- Interproximal caries is not visible clinically
- Early bone loss associated with periodontal disease
- Impacted or unerupted teeth
- Periapical pathology and infections
Avoiding necessary imaging due to fear of radiation risk may lead to delayed diagnosis, more complex treatments, and poorer patient outcomes.
Thus, clinicians must carefully balance:
- Benefits: Accurate diagnosis and improved treatment outcomes
- Risks: Minimal but cumulative radiation exposure
When used appropriately, the benefits of dental X-rays far outweigh the potential risks.

Modern Digital Radiography Significantly Reduces Radiation Dose To Patients
Advancements in dental technology have significantly reduced the radiation risk associated with dental X-rays.
Modern digital radiography systems offer:
- Up to 70–90% lower radiation doses compared to traditional film-based imaging
- Faster image acquisition, reducing exposure time
- Enhanced image clarity for improved diagnostic accuracy
In many cases, the radiation dose from a dental X-ray is comparable to the natural background radiation received in a single day.
These innovations further weaken the argument that dental X-rays significantly contribute to brain tumor risk, particularly when used responsibly.
Practical Recommendations For Dentists To Minimize Unnecessary Radiation Exposure
To ensure patient safety while maintaining diagnostic effectiveness, dental professionals should adopt best practices that minimize unnecessary radiation exposure.
Recommended strategies include:
- Perform thorough clinical examinations before prescribing imaging
- Use selective radiography based on patient-specific risk factors
- Prefer digital X-ray systems to reduce radiation dose
- Apply appropriate shielding techniques, including thyroid collars
- Educate patients about the realistic risks and benefits of dental X-rays
By following these principles, clinicians can reduce the potential link between dental X-rays and brain tumors while maintaining high standards of care.
Frequently Asked Questions About Dental X-Rays And Brain Tumors
1. Do dental X-rays cause brain tumors?
There is no conclusive evidence proving that dental X-rays directly cause brain tumors. Some studies show an association, but causation remains unproven.
2. What is the link between dental X-rays and meningioma?
Certain studies suggest an increased association between dental X-rays and meningioma, but confounding factors make it difficult to establish a direct causal relationship.
3. Are dental X-rays safe for children?
Yes, when used appropriately. However, children are more sensitive to radiation, so imaging should be carefully justified.
4. How can radiation risk from dental X-rays be minimized?
Radiation risk can be reduced by limiting unnecessary imaging, using digital systems, and following ALARA principles.
5. Do lead aprons protect the brain during dental X-rays?
No, lead aprons protect the body but do not shield the brain, which remains exposed during imaging.
6. Should patients avoid dental X-rays due to fear of cancer؟
No, it is not recommended to avoid dental X-rays when they are needed, because the diagnostic benefits significantly outweigh the potential risks.
Conclusion
The potential relationship between dental X-rays and brain tumors, particularly meningioma, remains an area of ongoing scientific investigation. While some studies indicate a statistical association, there is no definitive evidence establishing causation.
For dental professionals, the key lies in applying evidence-based clinical judgment, minimizing unnecessary radiation exposure, and ensuring that every radiograph has a clear diagnostic purpose.
Ultimately, responsible and selective use of dental X-rays—not avoidance—is the most effective strategy to balance patient safety with optimal clinical outcomes.
Reference:
Recent Articles
Pulsed Electromagnetic Field (PEMF) Use in Implant Dentistry
Pulsed Electromagnetic Field (PEMF) Use in Implant Dentistry Abstract and Historical Background Pulsed Electromagnetic Field (PEMF) therapy refers to the application of low-frequency electromagnetic [...]
Laser Therapy in the Management of Peri-Implantitis
Laser Therapy in the Management of Peri-Implantitis Laser technology has become an increasingly valuable adjunct in the treatment of peri-implant diseases, particularly peri-implantitis. Its [...]
Magnetically Guided Dental Nanobots (CalBots) Are Real
Magnetically Guided Dental Nanobots (CalBots) Are Real The concept of nanobots in dentistry has long been associated with futuristic speculation. However, recent peer-reviewed research [...]
Peri-Implantitis Treatment & Prevention Methods
Peri-Implantitis Treatment & Prevention Methods Peri-implantitis remains one of the most significant biological complications affecting dental implants, posing a serious threat to long-term implant [...]
Latest Sinus Lifting Techniques in Modern Implant Dentistry
Latest Sinus Lifting Techniques in Modern Implant Dentistry A Comprehensive Clinical Review Introduction to Sinus Lifting in Implantology Sinus lifting, or maxillary sinus floor [...]
Biomechanics of the Triple Abutment & BOPiT Concept
Dental Biomechanics · Implant Science · Clinical Evidence Biomechanics of the Triple Abutment & BOPiT Concept How a saddle-shaped mathematical surface is rewriting the rules of load distribution [...]