The Rise of Self‑Healing Dental Biomaterials
Introduction
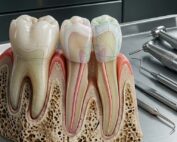
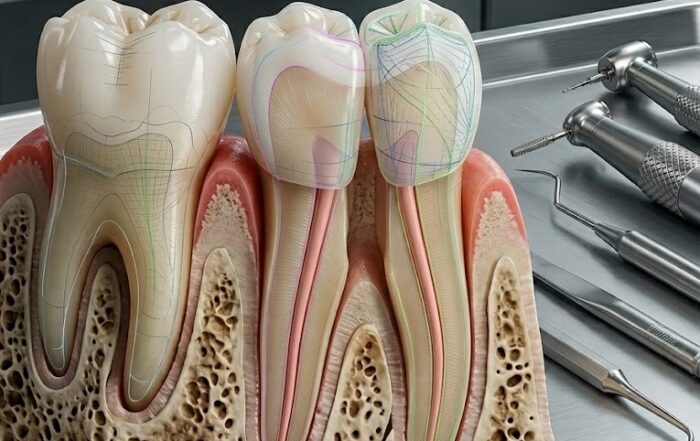
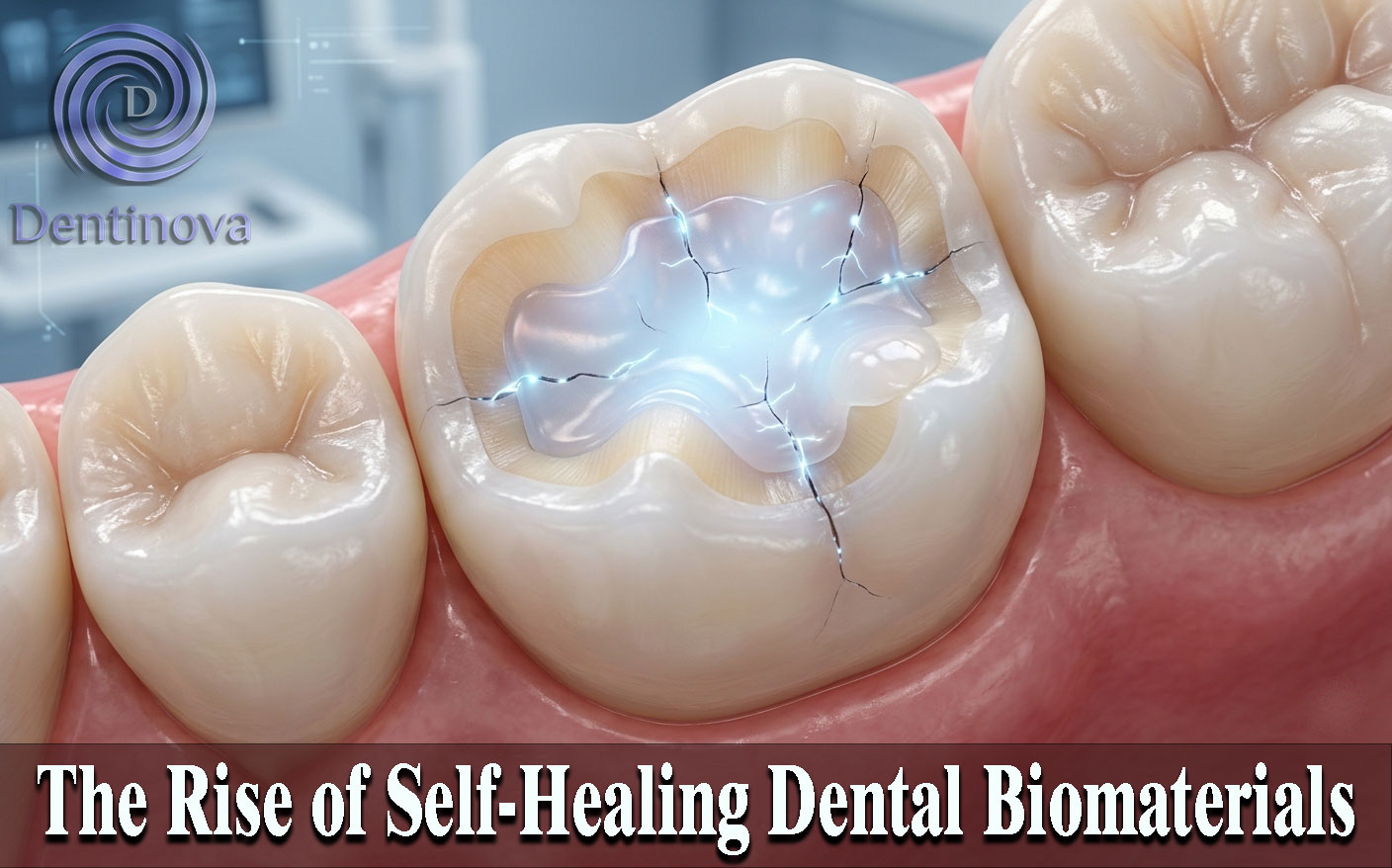
In modern restorative dentistry, durability and longevity of materials remain among the greatest clinical challenges. Traditional dental composites and cements often fail due to microcracks, mechanical fatigue, hydrolytic breakdown, and degradation at resin‑to‑tooth interfaces, leading to recurrent procedures and increased patient costs. Innovative self‑healing dental biomaterials seek to address this problem by enabling materials to autonomously repair damage, potentially extending restoration life and improving clinical outcomes. This article explores the mechanisms, clinical implications, current research, and future prospects of self‑healing dental biomaterials — including resin composites, adhesives, and multifunctional restorative systems — based on multiple peer‑reviewed scientific sources.
1. Fundamentals of Self‑Healing Dental Biomaterials
Self‑healing biomaterials in dentistry are engineered restorative materials designed to detect damage such as microcracks and then autonomously activate repair mechanisms without operator intervention. The self‑healing dental biomaterials concept draws inspiration from natural biological processes, such as dentin regeneration and bone remodeling, where living tissues repair themselves in response to stimuli.
What Makes a Dental Material “Self‑Healing”?
Fundamentally, self‑healing dental biomaterials incorporate mechanisms that either:
- Release healing agents upon damage (extrinsic systems), or
- Allow dynamic reformation of chemical bonds within the material (intrinsic systems).
Extrinsic healing systems are typically microcapsule‑based: tiny embedded capsules filled with reactive monomers that are released when a crack propagates, initiating polymerization and sealing it. Intrinsic self‑healing systems rely on reversible chemical bonds — such as supramolecular hydrogen bonds or dynamic covalent networks — that reform after mechanical disruption.
Why Self‑Healing Matters in Dentistry
Dental restorations are exposed to a complex, dynamic oral environment with repeated mechanical loads from chewing, thermal cycling, pH fluctuations, and bacterial activity. These conditions accelerate material degradation and microcrack formation, often leading to restoration failure in as little as 6–10 years. By enabling autonomous repair, self‑healing biomaterials aim to:
- Prolong restoration lifespan
- Reduce healthcare costs
- Minimize secondary caries and tooth structure loss
- Support sustainable dental practice by reducing waste and resource use
This shift from repair‑and‑replace towards durable and adaptive restorative materials is a major evolutionary step in biomaterials research with significant clinical implications.
2. Mechanisms of Self‑Healing in Dental Biomaterials
To design and implement self‑healing properties in dental restoratives, researchers investigate a range of mechanisms rooted in material science and polymer chemistry.
Extrinsic Healing: Microcapsule‑Based Systems
Microcapsule‑based self‑healing dental composites embed tiny capsules containing a healing agent within a resin matrix. When stress or a developing crack ruptures these capsules, the healing agent is released into the crack plane, initiating polymerization and sealing the defect.
Key advantages:
- Autonomous activation without external stimuli
- Compatibility with existing composite resin formulations
Challenges:
- Ensuring sufficient mechanical strength after healing
- Preventing premature capsule rupture during handling
Intrinsic Healing: Dynamic and Reversible Chemistry
Intrinsic self‑healing mechanisms exploit reversible chemical interactions. Examples include:
- Dynamic covalent bonds (e.g., Diels–Alder reactions) that break and reform under ambient conditions
- Supramolecular hydrogen bonding that enables polymer segments to reattach after disruption
These intrinsic systems allow repeated healing throughout the lifespan of the restoration, rather than only once or twice as with microcapsule systems.
Multifunctional Systems
A new generation of dental biomaterials integrates self‑healing with antibacterial and remineralizing functions. These advanced resin composites can:
- Inhibit bacterial colonization
- Promote mineral deposition to counteract demineralization
- Autonomously repair cracks
This multifunctional approach aims to create dental restorations that are not only durable but also biologically active and resistant to common failure modes.
3. Self‑Healing Dental Composites: From Research to Practice
Dental composites represent one of the most widely investigated platforms for self‑healing functionality due to their prevalence in restorative procedures and susceptibility to microcrack formation.
Microcapsule‑Based Self‑Healing Dental Composites
Researchers review how microcapsule‑based systems have evolved, noting that microcapsules containing reactive monomers can be incorporated into conventional dental resin composites. Upon crack formation, these capsules rupture and release healing agents that polymerize upon contact with embedded catalysts — effectively sealing the microcrack and slowing crack propagation.
Such systems show promise in laboratory settings, demonstrating enhanced mechanical recovery compared to traditional composites and maintaining esthetic and handling properties desirable to clinicians.
Multifunctional Self‑Healing Composites
The trend in restorative dental research is moving toward multifunctional composites that combine self‑healing with antibacterial and remineralizing properties. These materials not only repair mechanical damage but also actively resist biofilm formation and promote mineral regeneration at restoration margins.
Clinical Translation and Challenges
Despite significant progress, self‑healing dental composites are still predominantly at the research stage. Major hurdles to clinical translation include:
- Ensuring complete biocompatibility of all healing agents and byproducts
- Regulatory approval processes
- Maintaining mechanical properties equivalent to established materials
- Cost‑effective large‑scale production
Future directions in research, however, suggest that combining inherently biocompatible components with advanced polymer networks may bring clinically viable self‑healing composites closer to routine use.
4. Integrating Self‑Healing in Dental Adhesives and Cements
While composites have been the primary focus, self‑healing strategies are also being investigated in dental adhesives and cements — two additional material classes heavily used in restorative and prosthetic dentistry.
Self‑Healing Dental Adhesives
Dental adhesives are susceptible to degradation at the resin‑tooth interface due to hydrolysis and mechanical stress. Integrating dynamic bonding mechanisms or microcapsules into adhesive formulations may allow interfaces to repair minor defects before they propagate into failures.
Self‑Healing Dental Cements
Self‑healing dental cements could extend the lifespan of crowns, bridges, and implant prosthetics by repairing microcracks caused by occlusal forces or thermal expansion mismatches. Research indicates that microcapsule‑based and dynamic polymer systems might be adapted for these applications, although further work is needed to optimize cement flow, curing behavior, and long‑term stability.
Benefits Beyond Cracks
In addition to sealing microdamage, future self‑healing adhesives and cements might also:
- Reduce secondary caries at the restoration margin
- Lower rates of debonding in prosthetic applications
- Improve longevity of indirect restorations
Optimizing these materials demands interdisciplinary collaboration among polymer chemists, material scientists, and clinical researchers to ensure both functional performance and safety.
5. Advantages of Self‑Healing Biomaterials in the Dental Field
The integration of self‑healing biomaterials in the dental field offers significant clinical, economic, and environmental benefits compared to conventional restorative materials.
Enhanced Durability and Reduced Failure Rates
Self‑healing materials can autonomously repair early microcracks and defects, slowing or even preventing progression to macroscopic failure. This enhancement can significantly extend restoration life, reducing replacement frequency and associated costs.
Sustainable and Eco‑Friendly Dentistry
Extended restoration longevity reduces material consumption, clinical time, and waste generation — aligning with the principles of sustainable dentistry. Reducing the need for repeated interventions contributes to:
- Lower environmental burden from dental consumables
- Reduced energy usage and clinical resource demands
- Improved patient satisfaction and comfort
Potential for Multifunctional Therapies
By combining self‑healing with antibacterial and remineralization functions, next‑generation biomaterials could:
- Reduce secondary caries
- Promote tissue regeneration
- Provide adaptive responses to the oral environment
This multifunctionality presents a paradigm shift toward holistic and preventive dentistry.
6. Future Directions and Research Opportunities
Although the concept of self‑healing biomaterials in dentistry is well established in research, clinical application remains nascent. Continued innovation is needed across several fronts:
Biocompatible Healing Agents
Developing healing chemistries that are derived from or closely related to established dental monomers (e.g., Bis‑GMA, UDMA, TEGDMA) may mitigate cytotoxicity concerns and facilitate regulatory approval.
Dynamic Polymer Networks
Intrinsic self‑healing systems leveraging reversible covalent or supramolecular interactions could enable repeated healing cycles throughout the lifetime of a restoration.
Standardized Testing Models
Robust in vitro and in vivo models are needed to comprehensively assess healing efficiency under simulated oral conditions, including cyclic loading, thermal changes, and microbial challenges.
Commercial Translation
Bridging the gap between laboratory prototypes and marketable products will require collaboration among academia, industry, and regulatory bodies.
The potential benefits of self‑healing dental biomaterials — from improved clinical outcomes to sustainable practice — make this research an exciting and meaningful frontier.
What Has Been Accomplished So Far
1. Patented Self‑Healing Composite Technology
There are United States patents and technology descriptions (e.g., US9931281B2) covering multi‑functional self‑healing dental composites with embedded microcapsules that can autonomously repair microcracks. These patents describe how such materials would be formulated and used but do not correspond to currently marketed products. They instead represent licensed technologies or prototypes that could be developed into commercial offerings.
2. Research‑Stage Prototypes Recognized by Professional Organizations
The American Dental Association (ADA) Science & Research Institute lists self‑healing dental composites as a technology opportunity (with specifications and patent status), but not as a product you can order and use clinically today. This listing is for licensing, collaboration, or future development, not for marketed restorative materials.
Frequently Asked Questions (FAQ)
Q1: What are self‑healing dental biomaterials?
A1: Self‑healing biomaterials are restorative dental materials designed to autonomously repair microcracks or defects without operator intervention, often using embedded healing agents or dynamic chemical bonds.
Q2: How do microcapsule‑based self‑healing composites work?
A2: Microcapsule‑based composites contain tiny capsules filled with a reactive healing agent that rupture when a crack forms, releasing the agent to polymerize and seal the defect.
Q3: Are self‑healing dental materials currently used in clinical practice?
A3: Most self‑healing dental materials remain in research and prototype stages. Clinical translation is ongoing but not yet widespread.
Q4: What advantages do self‑healing dental biomaterials offer?
A4: They can enhance restoration longevity, reduce replacement frequency, lower healthcare costs, and support eco‑friendly dental practices.
Q5: Can self‑healing dental materials also have antibacterial properties?
A5: Yes — multifunctional restoratives are being developed that combine self‑healing with antibacterial and remineralizing capabilities.
Q6: What are the main challenges for self‑healing dental biomaterials?
A6: Challenges include ensuring biocompatibility, maintaining mechanical properties, regulatory approval, and large‑scale production feasibility.
References
- Xiaoxi Wang & Tian Ding. A Review on the Current State of Microcapsule‑Based Self‑Healing Dental Composites. J Funct Biomater 2024.
- Aftab Ahmed Khan. Self‑healing Dental Biomaterials: Bioinspired Pathways to Sustainable Dentistry. Biomater Investig Dent 2025.
- Jinshuang Zhang et al. A review of new generation of dental restorative resin composites with antibacterial, remineralizing and self‑healing capabilities. Discover Nano 2024.
Recent Articles
Introduction
In modern restorative dentistry, durability and longevity of materials remain among the greatest clinical challenges. Traditional dental composites and cements often fail due to microcracks, mechanical fatigue, hydrolytic breakdown, and degradation at resin‑to‑tooth interfaces, leading to recurrent procedures and increased patient costs. Innovative self‑healing dental biomaterials seek to address this problem by enabling materials to autonomously repair damage, potentially extending restoration life and improving clinical outcomes. This article explores the mechanisms, clinical implications, current research, and future prospects of self‑healing dental biomaterials — including resin composites, adhesives, and multifunctional restorative systems — based on multiple peer‑reviewed scientific sources.
1. Fundamentals of Self‑Healing Dental Biomaterials
Self‑healing biomaterials in dentistry are engineered restorative materials designed to detect damage such as microcracks and then autonomously activate repair mechanisms without operator intervention. The self‑healing dental biomaterials concept draws inspiration from natural biological processes, such as dentin regeneration and bone remodeling, where living tissues repair themselves in response to stimuli.
What Makes a Dental Material “Self‑Healing”?
Fundamentally, self‑healing dental biomaterials incorporate mechanisms that either:
- Release healing agents upon damage (extrinsic systems), or
- Allow dynamic reformation of chemical bonds within the material (intrinsic systems).
Extrinsic healing systems are typically microcapsule‑based: tiny embedded capsules filled with reactive monomers that are released when a crack propagates, initiating polymerization and sealing it. Intrinsic self‑healing systems rely on reversible chemical bonds — such as supramolecular hydrogen bonds or dynamic covalent networks — that reform after mechanical disruption.
Why Self‑Healing Matters in Dentistry
Dental restorations are exposed to a complex, dynamic oral environment with repeated mechanical loads from chewing, thermal cycling, pH fluctuations, and bacterial activity. These conditions accelerate material degradation and microcrack formation, often leading to restoration failure in as little as 6–10 years. By enabling autonomous repair, self‑healing biomaterials aim to:
- Prolong restoration lifespan
- Reduce healthcare costs
- Minimize secondary caries and tooth structure loss
- Support sustainable dental practice by reducing waste and resource use
This shift from repair‑and‑replace towards durable and adaptive restorative materials is a major evolutionary step in biomaterials research with significant clinical implications.
2. Mechanisms of Self‑Healing in Dental Biomaterials
To design and implement self‑healing properties in dental restoratives, researchers investigate a range of mechanisms rooted in material science and polymer chemistry.
Extrinsic Healing: Microcapsule‑Based Systems
Microcapsule‑based self‑healing dental composites embed tiny capsules containing a healing agent within a resin matrix. When stress or a developing crack ruptures these capsules, the healing agent is released into the crack plane, initiating polymerization and sealing the defect.
Key advantages:
- Autonomous activation without external stimuli
- Compatibility with existing composite resin formulations
Challenges:
- Ensuring sufficient mechanical strength after healing
- Preventing premature capsule rupture during handling
Intrinsic Healing: Dynamic and Reversible Chemistry
Intrinsic self‑healing mechanisms exploit reversible chemical interactions. Examples include:
- Dynamic covalent bonds (e.g., Diels–Alder reactions) that break and reform under ambient conditions
- Supramolecular hydrogen bonding that enables polymer segments to reattach after disruption
These intrinsic systems allow repeated healing throughout the lifespan of the restoration, rather than only once or twice as with microcapsule systems.
Multifunctional Systems
A new generation of dental biomaterials integrates self‑healing with antibacterial and remineralizing functions. These advanced resin composites can:
- Inhibit bacterial colonization
- Promote mineral deposition to counteract demineralization
- Autonomously repair cracks
This multifunctional approach aims to create dental restorations that are not only durable but also biologically active and resistant to common failure modes.
3. Self‑Healing Dental Composites: From Research to Practice
Dental composites represent one of the most widely investigated platforms for self‑healing functionality due to their prevalence in restorative procedures and susceptibility to microcrack formation.
Microcapsule‑Based Self‑Healing Dental Composites
Researchers review how microcapsule‑based systems have evolved, noting that microcapsules containing reactive monomers can be incorporated into conventional dental resin composites. Upon crack formation, these capsules rupture and release healing agents that polymerize upon contact with embedded catalysts — effectively sealing the microcrack and slowing crack propagation.
Such systems show promise in laboratory settings, demonstrating enhanced mechanical recovery compared to traditional composites and maintaining esthetic and handling properties desirable to clinicians.
Multifunctional Self‑Healing Composites
The trend in restorative dental research is moving toward multifunctional composites that combine self‑healing with antibacterial and remineralizing properties. These materials not only repair mechanical damage but also actively resist biofilm formation and promote mineral regeneration at restoration margins.
Clinical Translation and Challenges
Despite significant progress, self‑healing dental composites are still predominantly at the research stage. Major hurdles to clinical translation include:
- Ensuring complete biocompatibility of all healing agents and byproducts
- Regulatory approval processes
- Maintaining mechanical properties equivalent to established materials
- Cost‑effective large‑scale production
Future directions in research, however, suggest that combining inherently biocompatible components with advanced polymer networks may bring clinically viable self‑healing composites closer to routine use.
4. Integrating Self‑Healing in Dental Adhesives and Cements
While composites have been the primary focus, self‑healing strategies are also being investigated in dental adhesives and cements — two additional material classes heavily used in restorative and prosthetic dentistry.
Self‑Healing Dental Adhesives
Dental adhesives are susceptible to degradation at the resin‑tooth interface due to hydrolysis and mechanical stress. Integrating dynamic bonding mechanisms or microcapsules into adhesive formulations may allow interfaces to repair minor defects before they propagate into failures.
Self‑Healing Dental Cements
Self‑healing dental cements could extend the lifespan of crowns, bridges, and implant prosthetics by repairing microcracks caused by occlusal forces or thermal expansion mismatches. Research indicates that microcapsule‑based and dynamic polymer systems might be adapted for these applications, although further work is needed to optimize cement flow, curing behavior, and long‑term stability.
Benefits Beyond Cracks
In addition to sealing microdamage, future self‑healing adhesives and cements might also:
- Reduce secondary caries at the restoration margin
- Lower rates of debonding in prosthetic applications
- Improve longevity of indirect restorations
Optimizing these materials demands interdisciplinary collaboration among polymer chemists, material scientists, and clinical researchers to ensure both functional performance and safety.
5. Advantages of Self‑Healing Biomaterials in the Dental Field
The integration of self‑healing biomaterials in the dental field offers significant clinical, economic, and environmental benefits compared to conventional restorative materials.
Enhanced Durability and Reduced Failure Rates
Self‑healing materials can autonomously repair early microcracks and defects, slowing or even preventing progression to macroscopic failure. This enhancement can significantly extend restoration life, reducing replacement frequency and associated costs.
Sustainable and Eco‑Friendly Dentistry
Extended restoration longevity reduces material consumption, clinical time, and waste generation — aligning with the principles of sustainable dentistry. Reducing the need for repeated interventions contributes to:
- Lower environmental burden from dental consumables
- Reduced energy usage and clinical resource demands
- Improved patient satisfaction and comfort
Potential for Multifunctional Therapies
By combining self‑healing with antibacterial and remineralization functions, next‑generation biomaterials could:
- Reduce secondary caries
- Promote tissue regeneration
- Provide adaptive responses to the oral environment
This multifunctionality presents a paradigm shift toward holistic and preventive dentistry.
6. Future Directions and Research Opportunities
Although the concept of self‑healing biomaterials in dentistry is well established in research, clinical application remains nascent. Continued innovation is needed across several fronts:
Biocompatible Healing Agents
Developing healing chemistries that are derived from or closely related to established dental monomers (e.g., Bis‑GMA, UDMA, TEGDMA) may mitigate cytotoxicity concerns and facilitate regulatory approval.
Dynamic Polymer Networks
Intrinsic self‑healing systems leveraging reversible covalent or supramolecular interactions could enable repeated healing cycles throughout the lifetime of a restoration.
Standardized Testing Models
Robust in vitro and in vivo models are needed to comprehensively assess healing efficiency under simulated oral conditions, including cyclic loading, thermal changes, and microbial challenges.
Commercial Translation
Bridging the gap between laboratory prototypes and marketable products will require collaboration among academia, industry, and regulatory bodies.
The potential benefits of self‑healing dental biomaterials — from improved clinical outcomes to sustainable practice — make this research an exciting and meaningful frontier.
What Has Been Accomplished So Far
1. Patented Self‑Healing Composite Technology
There are United States patents and technology descriptions (e.g., US9931281B2) covering multi‑functional self‑healing dental composites with embedded microcapsules that can autonomously repair microcracks. These patents describe how such materials would be formulated and used but do not correspond to currently marketed products. They instead represent licensed technologies or prototypes that could be developed into commercial offerings.
2. Research‑Stage Prototypes Recognized by Professional Organizations
The American Dental Association (ADA) Science & Research Institute lists self‑healing dental composites as a technology opportunity (with specifications and patent status), but not as a product you can order and use clinically today. This listing is for licensing, collaboration, or future development, not for marketed restorative materials.
Frequently Asked Questions (FAQ)
Q1: What are self‑healing dental biomaterials?
A1: Self‑healing biomaterials are restorative dental materials designed to autonomously repair microcracks or defects without operator intervention, often using embedded healing agents or dynamic chemical bonds.
Q2: How do microcapsule‑based self‑healing composites work?
A2: Microcapsule‑based composites contain tiny capsules filled with a reactive healing agent that rupture when a crack forms, releasing the agent to polymerize and seal the defect.
Q3: Are self‑healing dental materials currently used in clinical practice?
A3: Most self‑healing dental materials remain in research and prototype stages. Clinical translation is ongoing but not yet widespread.
Q4: What advantages do self‑healing dental biomaterials offer?
A4: They can enhance restoration longevity, reduce replacement frequency, lower healthcare costs, and support eco‑friendly dental practices.
Q5: Can self‑healing dental materials also have antibacterial properties?
A5: Yes — multifunctional restoratives are being developed that combine self‑healing with antibacterial and remineralizing capabilities.
Q6: What are the main challenges for self‑healing dental biomaterials?
A6: Challenges include ensuring biocompatibility, maintaining mechanical properties, regulatory approval, and large‑scale production feasibility.
References
- Xiaoxi Wang & Tian Ding. A Review on the Current State of Microcapsule‑Based Self‑Healing Dental Composites. J Funct Biomater 2024.
- Aftab Ahmed Khan. Self‑healing Dental Biomaterials: Bioinspired Pathways to Sustainable Dentistry. Biomater Investig Dent 2025.
- Jinshuang Zhang et al. A review of new generation of dental restorative resin composites with antibacterial, remineralizing and self‑healing capabilities. Discover Nano 2024.
Recent Articles
The Bicuspidization Protocol: Engineering Meets Survival
The Bicuspidization Protocol: Engineering Meets Survival Modern restorative dentistry is no longer limited to extraction and replacement. In the era of conservative and biologically [...]
Pulsed Electromagnetic Field (PEMF) Use in Implant Dentistry
Pulsed Electromagnetic Field (PEMF) Use in Implant Dentistry Abstract and Historical Background Pulsed Electromagnetic Field (PEMF) therapy refers to the application of low-frequency electromagnetic [...]
Laser Therapy in the Management of Peri-Implantitis
Laser Therapy in the Management of Peri-Implantitis Laser technology has become an increasingly valuable adjunct in the treatment of peri-implant diseases, particularly peri-implantitis. Its [...]
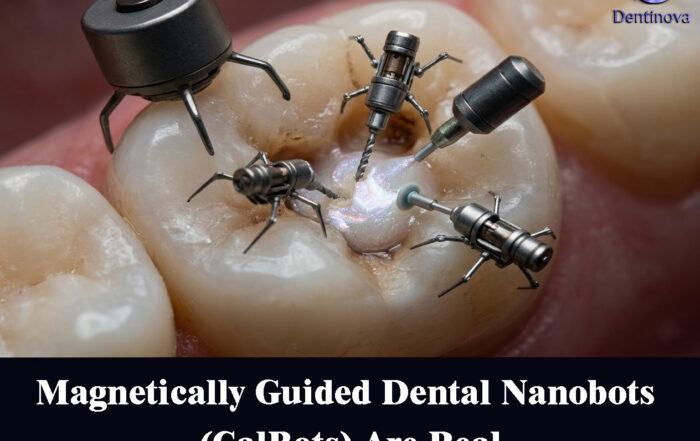
Magnetically Guided Dental Nanobots (CalBots) Are Real
Magnetically Guided Dental Nanobots (CalBots) Are Real The concept of nanobots in dentistry has long been associated with futuristic speculation. However, recent peer-reviewed research [...]
Peri-Implantitis Treatment & Prevention Methods
Peri-Implantitis Treatment & Prevention Methods Peri-implantitis remains one of the most significant biological complications affecting dental implants, posing a serious threat to long-term implant [...]
Latest Sinus Lifting Techniques in Modern Implant Dentistry
Latest Sinus Lifting Techniques in Modern Implant Dentistry A Comprehensive Clinical Review Introduction to Sinus Lifting in Implantology Sinus lifting, or maxillary sinus floor [...]