In-Situ Direct 3D Bone Grafting: The Future of Bone Repair
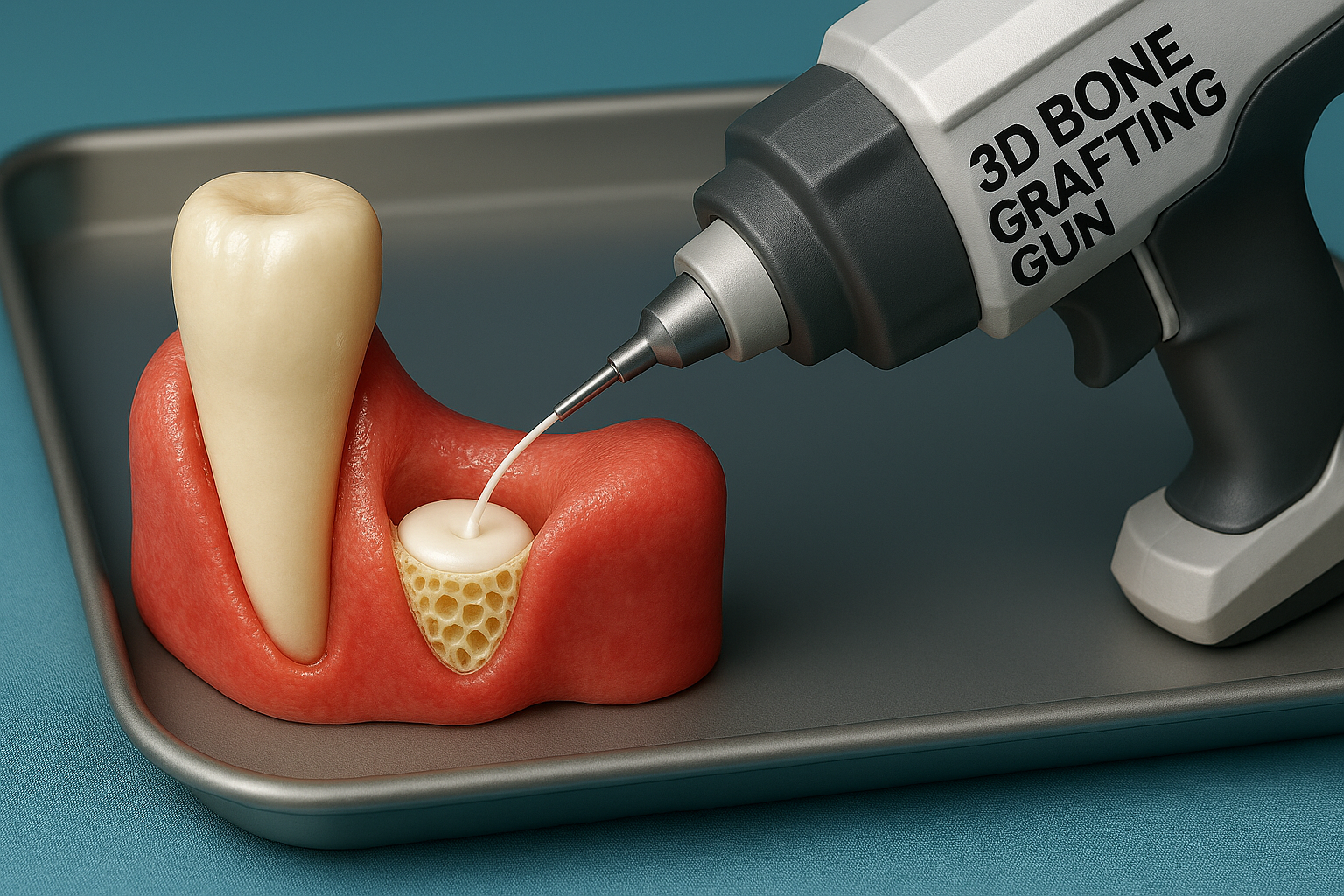
A groundbreaking innovation from researchers at Sungkyunkwan University in South Korea is revolutionizing bone repair. The team has developed a handheld 3D printing device—often described as a “medical hot glue gun”—capable of performing in-situ direct 3D bone grafting right inside the operating room.
This cutting-edge technique allows surgeons to print bone-like scaffolds directly into damaged areas during surgery, dramatically reducing healing time and infection risks. If clinical trials confirm its safety and efficacy, this advancement could become one of the most transformative milestones in orthopedic surgery since the advent of titanium implants.
How In-Situ Direct 3D Bone Grafting Works
Unlike traditional bone implants, in-situ direct 3D bone grafting uses a compact, handheld device that functions similarly to a hot glue gun—but with far more precision. The device extrudes a bio-ink composed of advanced materials designed to replicate the properties of natural bone.
This bio-ink typically includes:
- Hydroxyapatite – the mineral that provides rigidity and structure in human bone.
- Biocompatible polymers – adding flexibility and mechanical stability for better healing.
- Antibacterial agents – reducing the risk of post-surgical infections.
Surgeons can “print” customized bone scaffolds directly at the injury site. The printed matrix acts as a temporary framework, guiding the body’s natural bone cells to regenerate around it. Over time, the artificial scaffold is replaced by natural bone tissue, offering a seamless and permanent repair.
Why In-Situ Bone Grafting Is a Medical Breakthrough
For decades, bone repair has been one of the most complex challenges in modern medicine. Traditional methods rely on metal plates, screws, or donor grafts—each with notable drawbacks. Metal implants can loosen or cause inflammation, while donor grafts are limited in supply and may lead to immune rejection.
In contrast, in-situ direct 3D bone grafting offers a personalized, low-risk alternative. By allowing bone structures to be printed directly during surgery:
- Healing becomes faster, as the printed scaffold integrates with living cells immediately.
- The risk of infection is minimized thanks to built-in antibacterial components.
- Custom geometries can be created for complex fractures in the skull, spine, or jaw—areas where conventional implants often fail.
This level of precision and adaptability marks a shift toward truly personalized regenerative medicine.
The Rise of 3D Printing in Regenerative Medicine
The success of in-situ direct 3D bone grafting builds upon the growing use of additive manufacturing in healthcare. Over the last decade, 3D printing has become a cornerstone of biomedical engineering, enabling innovations such as:
- Custom prosthetic limbs designed for perfect ergonomic fit.
- Dental implants and crowns printed with micrometer accuracy.
- Bio-scaffolds for regenerating skin, cartilage, and even liver tissue.
Direct bone printing takes this concept to the next level—allowing surgeons to fabricate living scaffolds inside the body instead of relying on pre-made implants. This is a crucial step toward a future where regenerative procedures can be tailored not just to a condition, but to each patient’s unique anatomy.
Applications of In-Situ Direct 3D Bone Grafting
The versatility of this technology extends far beyond routine orthopedic surgeries. Some of its most promising applications include:
1. Trauma and Emergency Medicine
In disaster zones or battlefield environments, rapid bone repair can save lives. Portable in-situ bone printers could enable medics to stabilize fractures immediately, reducing complications and improving survival rates without waiting for advanced hospital care.
2. Pediatric Bone Reconstruction
Children often outgrow traditional implants, requiring multiple surgeries. In-situ printed scaffolds grow naturally with the child’s bone, reducing the need for future operations and minimizing long-term trauma.
3. Complex Facial and Spinal Surgeries
Jaw, skull, and spine reconstructions involve intricate geometries that are difficult to match with standard implants. 3D bone printing enables fully customized, patient-specific grafts that fit precisely and promote faster recovery.
Material Science Behind the Innovation
At the core of in-situ direct 3D bone grafting lies advanced material science. The challenge has always been finding a formula that balances printability, strength, and biocompatibility. The South Korean team achieved this by developing a hybrid material blend based on hydroxyapatite and specialized polymers that can be extruded at controlled temperatures.
Key scientific challenges addressed include:
- Printability: Ensuring the bio-ink can flow smoothly through the nozzle without clogging or degrading its biological components.
- Mechanical strength: Balancing rigidity and flexibility to match the mechanical behavior of natural bone.
- Biocompatibility: Encouraging bone cell adhesion and growth without triggering immune rejection.
Early laboratory and animal trials have shown promising results, with printed scaffolds demonstrating excellent integration into living bone and significantly lower infection rates compared to conventional grafts.
Challenges and the Road Ahead
Despite its promise, in-situ direct 3D bone grafting remains at an experimental stage. Several challenges must be overcome before it becomes a standard surgical practice:
- Clinical validation: Large-scale human trials are needed to confirm safety, durability, and long-term outcomes.
- Regulatory approval: New standards must be established to certify printed biomaterials for use in hospitals worldwide.
- Surgeon training: Operating with a bio-printer requires new skills and real-time precision under surgical conditions.
- Affordability and scalability: The technology must be cost-effective for hospitals globally, not just elite research centers.
However, ongoing research suggests that with refinement, portable bone printers could soon be deployed in field hospitals, trauma centers, and operating rooms across the world.
What the Future Holds
The future of in-situ direct 3D bone grafting is bright. Researchers are already exploring hybrid bio-inks that incorporate growth factors or stem cells to further accelerate bone regeneration. Portable versions of the printer are being designed for emergency response units and military medics.
If regulatory and clinical milestones are met, early adoption could begin within the next decade—potentially replacing a large percentage of traditional metal-based implants. Over time, this could lead to a new era in surgery where bones, tissues, and perhaps even organs are printed directly within the patient’s body.
Conclusion
The handheld 3D bone printer from South Korea represents a monumental leap in regenerative medicine. By merging materials science, bioengineering, and surgical innovation, it makes in-situ direct 3D bone grafting a real possibility—transforming how fractures and bone loss are treated.
From pediatric care to trauma surgery, this innovation promises faster healing, reduced infection risks, and personalized precision unmatched by conventional methods. As the technology matures, it may well redefine the boundaries of modern orthopedics and open the door to fully patient-specific, regenerative healthcare for future generations.
Recent Articles
A groundbreaking innovation from researchers at Sungkyunkwan University in South Korea is revolutionizing bone repair. The team has developed a handheld 3D printing device—often described as a “medical hot glue gun”—capable of performing in-situ direct 3D bone grafting right inside the operating room.
This cutting-edge technique allows surgeons to print bone-like scaffolds directly into damaged areas during surgery, dramatically reducing healing time and infection risks. If clinical trials confirm its safety and efficacy, this advancement could become one of the most transformative milestones in orthopedic surgery since the advent of titanium implants.
How In-Situ Direct 3D Bone Grafting Works
Unlike traditional bone implants, in-situ direct 3D bone grafting uses a compact, handheld device that functions similarly to a hot glue gun—but with far more precision. The device extrudes a bio-ink composed of advanced materials designed to replicate the properties of natural bone.
This bio-ink typically includes:
- Hydroxyapatite – the mineral that provides rigidity and structure in human bone.
- Biocompatible polymers – adding flexibility and mechanical stability for better healing.
- Antibacterial agents – reducing the risk of post-surgical infections.
Surgeons can “print” customized bone scaffolds directly at the injury site. The printed matrix acts as a temporary framework, guiding the body’s natural bone cells to regenerate around it. Over time, the artificial scaffold is replaced by natural bone tissue, offering a seamless and permanent repair.
Why In-Situ Bone Grafting Is a Medical Breakthrough
For decades, bone repair has been one of the most complex challenges in modern medicine. Traditional methods rely on metal plates, screws, or donor grafts—each with notable drawbacks. Metal implants can loosen or cause inflammation, while donor grafts are limited in supply and may lead to immune rejection.
In contrast, in-situ direct 3D bone grafting offers a personalized, low-risk alternative. By allowing bone structures to be printed directly during surgery:
- Healing becomes faster, as the printed scaffold integrates with living cells immediately.
- The risk of infection is minimized thanks to built-in antibacterial components.
- Custom geometries can be created for complex fractures in the skull, spine, or jaw—areas where conventional implants often fail.
This level of precision and adaptability marks a shift toward truly personalized regenerative medicine.
The Rise of 3D Printing in Regenerative Medicine
The success of in-situ direct 3D bone grafting builds upon the growing use of additive manufacturing in healthcare. Over the last decade, 3D printing has become a cornerstone of biomedical engineering, enabling innovations such as:
- Custom prosthetic limbs designed for perfect ergonomic fit.
- Dental implants and crowns printed with micrometer accuracy.
- Bio-scaffolds for regenerating skin, cartilage, and even liver tissue.
Direct bone printing takes this concept to the next level—allowing surgeons to fabricate living scaffolds inside the body instead of relying on pre-made implants. This is a crucial step toward a future where regenerative procedures can be tailored not just to a condition, but to each patient’s unique anatomy.
Applications of In-Situ Direct 3D Bone Grafting
The versatility of this technology extends far beyond routine orthopedic surgeries. Some of its most promising applications include:
1. Trauma and Emergency Medicine
In disaster zones or battlefield environments, rapid bone repair can save lives. Portable in-situ bone printers could enable medics to stabilize fractures immediately, reducing complications and improving survival rates without waiting for advanced hospital care.
2. Pediatric Bone Reconstruction
Children often outgrow traditional implants, requiring multiple surgeries. In-situ printed scaffolds grow naturally with the child’s bone, reducing the need for future operations and minimizing long-term trauma.
3. Complex Facial and Spinal Surgeries
Jaw, skull, and spine reconstructions involve intricate geometries that are difficult to match with standard implants. 3D bone printing enables fully customized, patient-specific grafts that fit precisely and promote faster recovery.
Material Science Behind the Innovation
At the core of in-situ direct 3D bone grafting lies advanced material science. The challenge has always been finding a formula that balances printability, strength, and biocompatibility. The South Korean team achieved this by developing a hybrid material blend based on hydroxyapatite and specialized polymers that can be extruded at controlled temperatures.
Key scientific challenges addressed include:
- Printability: Ensuring the bio-ink can flow smoothly through the nozzle without clogging or degrading its biological components.
- Mechanical strength: Balancing rigidity and flexibility to match the mechanical behavior of natural bone.
- Biocompatibility: Encouraging bone cell adhesion and growth without triggering immune rejection.
Early laboratory and animal trials have shown promising results, with printed scaffolds demonstrating excellent integration into living bone and significantly lower infection rates compared to conventional grafts.
Challenges and the Road Ahead
Despite its promise, in-situ direct 3D bone grafting remains at an experimental stage. Several challenges must be overcome before it becomes a standard surgical practice:
- Clinical validation: Large-scale human trials are needed to confirm safety, durability, and long-term outcomes.
- Regulatory approval: New standards must be established to certify printed biomaterials for use in hospitals worldwide.
- Surgeon training: Operating with a bio-printer requires new skills and real-time precision under surgical conditions.
- Affordability and scalability: The technology must be cost-effective for hospitals globally, not just elite research centers.
However, ongoing research suggests that with refinement, portable bone printers could soon be deployed in field hospitals, trauma centers, and operating rooms across the world.
What the Future Holds
The future of in-situ direct 3D bone grafting is bright. Researchers are already exploring hybrid bio-inks that incorporate growth factors or stem cells to further accelerate bone regeneration. Portable versions of the printer are being designed for emergency response units and military medics.
If regulatory and clinical milestones are met, early adoption could begin within the next decade—potentially replacing a large percentage of traditional metal-based implants. Over time, this could lead to a new era in surgery where bones, tissues, and perhaps even organs are printed directly within the patient’s body.
Conclusion
The handheld 3D bone printer from South Korea represents a monumental leap in regenerative medicine. By merging materials science, bioengineering, and surgical innovation, it makes in-situ direct 3D bone grafting a real possibility—transforming how fractures and bone loss are treated.
From pediatric care to trauma surgery, this innovation promises faster healing, reduced infection risks, and personalized precision unmatched by conventional methods. As the technology matures, it may well redefine the boundaries of modern orthopedics and open the door to fully patient-specific, regenerative healthcare for future generations.
Recent Articles
Peri-Implantitis Treatment & Prevention Methods
Peri-Implantitis Treatment & Prevention Methods Peri-implantitis remains one of the most significant biological complications affecting dental implants, posing a serious threat to long-term implant [...]
Latest Sinus Lifting Techniques in Modern Implant Dentistry
Latest Sinus Lifting Techniques in Modern Implant Dentistry A Comprehensive Clinical Review Introduction to Sinus Lifting in Implantology Sinus lifting, or maxillary sinus floor [...]
Biomechanics of the Triple Abutment & BOPiT Concept
Dental Biomechanics · Implant Science · Clinical Evidence Biomechanics of the Triple Abutment & BOPiT Concept How a saddle-shaped mathematical surface is rewriting the rules of load distribution [...]
The Woman Who Proved One Implant Could Hold Three Crowns
The Woman Who Proved One Implant Could Hold Three Crowns While the dental establishment looked away, Dr. Luciana Colepícolo spent 12 years building the [...]
ENPP1, The Molecular Brake That Limits Tissue Healing
ENPP1, The Molecular Brake That Limits Tissue Healing Introduction: A New Biological Barrier to Dental Regeneration Meet ENPP1—a protein most dentists have never heard [...]
The Rise of Self‑Healing Dental Biomaterials
The Rise of Self‑Healing Dental Biomaterials Introduction In modern restorative dentistry, durability and longevity of materials remain among the greatest clinical challenges. Traditional dental [...]