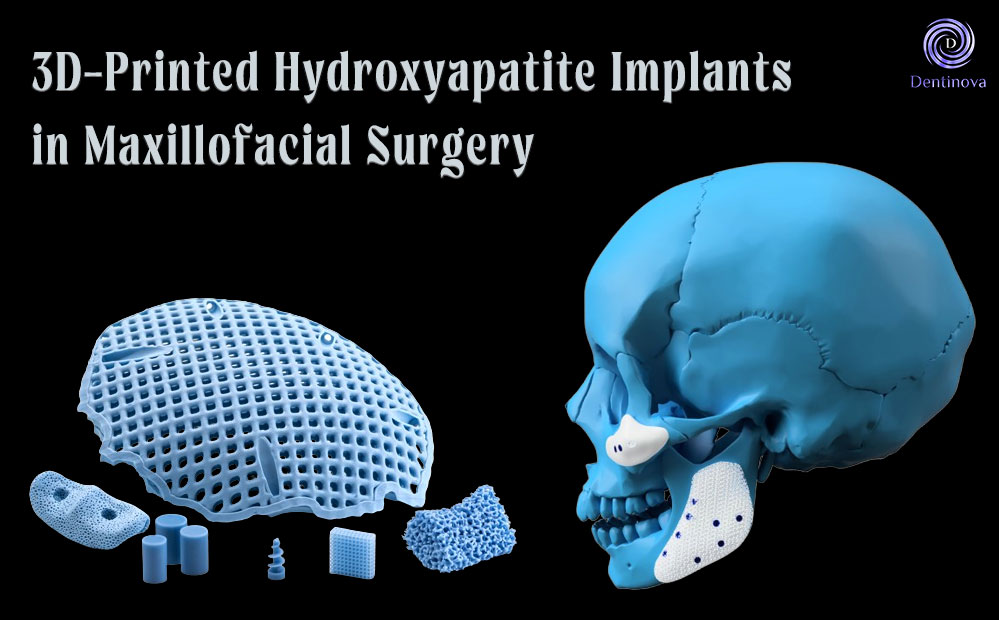
3D-Printed Hydroxyapatite Implants in Maxillofacial Surgery
Introduction
Maxillofacial surgery often involves the reconstruction of complex bone defects caused by trauma, tumor resection, congenital deformities, or severe infections. Traditional reconstruction methods, such as autologous bone grafts, titanium plates, and polymer-based implants, have long been the standard of care. However, these approaches present well-known challenges, including donor site morbidity, limited anatomical precision, risk of long-term foreign body reactions, and suboptimal biological integration.
In recent years, 3D-printed hydroxyapatite (HA) implants have emerged as a promising, biologically driven alternative. By combining additive manufacturing with a bone-mimicking bioceramic, these implants offer patient-specific geometry, enhanced osteointegration, and improved aesthetic and functional outcomes. As clinical evidence grows and regulatory approvals expand, 3D-printed hydroxyapatite implants are increasingly viewed as a next-generation solution for maxillofacial reconstruction.
This article provides a comprehensive, SEO-optimized overview of the technology, material science, clinical applications, commercially available products, advantages and limitations, and future outlook of 3D-printed hydroxyapatite implants in maxillofacial surgery.
Understanding Hydroxyapatite as a Biomaterial
What Is Hydroxyapatite?
Hydroxyapatite (chemical formula: Ca₁₀(PO₄)₆(OH)₂) is a naturally occurring calcium phosphate mineral that constitutes approximately 60–70% of human bone by weight and nearly 90% of dental enamel. Because of this close chemical and structural similarity to native bone, hydroxyapatite has been widely used in orthopedics, dentistry, and cranio-maxillofacial surgery for decades.
Key Biological Properties
Hydroxyapatite is valued in implantology due to several critical characteristics:
Excellent biocompatibility, with minimal inflammatory or immune response
Osteoconductivity, allowing bone cells to migrate along its surface
Bioactivity, enabling direct chemical bonding between the implant and the host bone
Surface affinity for proteins and osteoblasts, promoting bone regeneration
Unlike inert materials such as titanium or PEEK, hydroxyapatite does not simply occupy space; it actively participates in the bone healing process.
The Role of 3D Printing in Maxillofacial Implants
Additive Manufacturing and Patient-Specific Implants
3D printing, also known as additive manufacturing, enables the production of patient-specific implants (PSIs) based on CT or CBCT imaging data. Using digital planning software, surgeons and biomedical engineers can design implants that precisely replicate the patient’s anatomy and defect geometry.
For maxillofacial surgery, where millimeter-level accuracy affects occlusion, facial symmetry, and orbital support, this level of customization represents a major clinical advantage.
Controlled Porosity and Internal Architecture
One of the most important benefits of 3D printing hydroxyapatite is the ability to control internal porosity and pore interconnectivity. These structural features are essential for:
Vascular ingrowth
Nutrient diffusion
Bone cell migration
Long-term osteointegration
Well-designed porous HA implants function as three-dimensional scaffolds, gradually becoming integrated with living bone rather than remaining as isolated foreign bodies.
Clinical Applications in Maxillofacial Surgery
3D-printed hydroxyapatite implants are primarily used in non-load-bearing or moderately load-bearing maxillofacial reconstructions, where biological integration and anatomical accuracy are priorities.
Common Indications
Mandibular and maxillary bone defects following tumor resection
Zygomatic and midface reconstruction after trauma
Orbital floor and orbital wall reconstruction
Facial contour restoration for aesthetic and functional rehabilitation
Bone augmentation before dental implant placement (select cases)
In many of these scenarios, HA implants reduce or eliminate the need for autologous bone harvesting, thereby avoiding donor site complications.
Commercially Available 3D-Printed Hydroxyapatite Implants
Although still an emerging segment of the implant market, several clinically approved products and solutions are already available.
MyBone® Custom Implants (Cerhum, Belgium)
MyBone® is one of the most recognized commercial examples of a 3D-printed hydroxyapatite patient-specific implant for maxillofacial and craniofacial reconstruction.
Key Features:
Medical-grade porous hydroxyapatite
Fully patient-specific design based on CT imaging
Optimized pore architecture for vascularization and bone ingrowth
CE-marked under the European Medical Device Regulation (MDR)
Manufactured under ISO 13485 quality standards
Clinical case series have demonstrated excellent implant stability, absence of infection or displacement, and progressive osteointegration over follow-up periods.
BioCranium® and Custom HA Implants (3DCeram, France)
3DCeram provides advanced 3D-printed ceramic implants, including hydroxyapatite-based solutions for cranial and facial reconstruction. Their technology focuses on high-precision ceramic additive manufacturing with controlled micro- and macro-porosity.
These implants are typically used in complex cranio-maxillofacial defects where traditional materials may compromise biological integration or aesthetics.
Hydroxyapatite Materials for Custom Manufacturing
In addition to finished implants, medical-grade hydroxyapatite powders are supplied by specialized biomaterials companies. These materials are used by manufacturers, research institutions, and hospital-based 3D printing centers to develop custom scaffolds, composite implants, and experimental devices.
LithaBone HA Hydroxyapatite ( Lithoz, Austria)
LithaBone HA is an advanced, 3D-printable form of hydroxyapatite specifically engineered for the fabrication of patient-specific ceramic bone implants. Hydroxyapatite is a naturally occurring mineral and the primary inorganic component of human bone, which makes it exceptionally compatible with the body. Its high biocompatibility and osteoconductive behavior allow bone cells to adhere, proliferate, and gradually grow through the implant structure after implantation.
Advantages of LithaBone
One of the key advantages of hydroxyapatite is its controlled resorption profile. Once implanted, the material is slowly resorbed by the body while new natural bone is formed simultaneously. This process eliminates the need for secondary surgery to remove the implant and significantly reduces patient trauma and overall treatment costs. Compared to other bone substitute materials, hydroxyapatite resorbs at a slower rate, providing sufficient mechanical support and healing time, particularly in critical-sized bone defects that cannot heal on their own.
LithaBone HA has been optimized for additive manufacturing, offering high geometric freedom, tunable microporosity, and strong mechanical performance while remaining easy to handle during processing. Lithoz exclusively uses hydroxyapatite powders that comply with ASTM F1185 standards for surgical implants, ensuring high purity and controlled heavy metal content. The sintered ceramic exhibits excellent density, high bending strength, and proven biocompatibility in accordance with ISO 10993-5, making it a reliable solution for advanced bone regeneration applications.
Clinical Evidence and Outcomes
Published Case Series and Studies
Multiple peer-reviewed clinical reports have evaluated 3D-printed hydroxyapatite implants in maxillofacial reconstruction. Across these studies, key findings include:
High rates of implant survival
Low incidence of infection or inflammatory response
Progressive radiographic bone integration
Reduced need for intraoperative modification
Favorable aesthetic and functional outcomes
Surgeons consistently report improved surgical workflow due to precise preoperative planning and reduced operative time.
Advantages Over Traditional Materials
Biological Integration
Unlike titanium or polymer implants, hydroxyapatite actively bonds with host bone, creating a biological interface rather than a mechanical one.
Anatomical Precision
Patient-specific design ensures optimal fit, reduced dead space, and improved load distribution.
Reduced Donor Site Morbidity
By minimizing or eliminating the need for autologous bone grafts, HA implants reduce postoperative pain and complication risk.
Improved Aesthetics
Precise contour replication is especially important in visible facial regions, such as the zygoma and orbital rim.
Limitations and Considerations
Despite their advantages, 3D-printed hydroxyapatite implants have important limitations that must be considered.
Mechanical Strength
Hydroxyapatite is a brittle ceramic material, particularly when designed with high porosity. It is generally not suitable for high load-bearing applications without structural reinforcement or a hybrid design.
Cost and Production Time
Custom design, regulatory compliance, and specialized manufacturing increase cost compared to off-the-shelf implants.
Limited Long-Term Data
While short- and mid-term clinical outcomes are promising, large-scale, long-term comparative studies are still limited.
Future Directions and Innovations
Ongoing research aims to overcome current limitations and expand clinical indications. Key areas of development include:
Composite implants combining HA with polymers or bioresorbable materials
Doped hydroxyapatite (e.g., silicon- or magnesium-substituted HA) for enhanced bioactivity
Hybrid metal-ceramic designs for improved mechanical performance
Integration of growth factors or stem-cell-friendly surfaces
As these technologies mature, 3D-printed hydroxyapatite implants are expected to play a growing role in personalized maxillofacial surgery.
Conclusion
3D-printed hydroxyapatite implants represent a significant advancement in biologically driven, patient-specific maxillofacial reconstruction. By combining the osteoconductive properties of hydroxyapatite with the precision of additive manufacturing, these implants address many of the limitations of traditional reconstruction methods.
While challenges remain—particularly in mechanical strength and long-term clinical data—the current evidence and expanding commercial availability suggest that hydroxyapatite-based 3D-printed implants will become an increasingly important tool in modern maxillofacial surgery.
References
Dorozhkin SV. Calcium orthophosphates in nature, biology, and medicine. Materials.
Campana V, Milano G, Pagano E, et al. Bone substitutes in orthopaedic surgery: from basic science to clinical practice. J Mater Sci Mater Med.
Mangano C, Bianchi A, Mangano FG, et al. Custom-made 3D printed hydroxyapatite scaffolds for bone regeneration. J Craniofac Surg.
Cerhum SA. MyBone® Custom Hydroxyapatite Implants – Technical and Clinical Documentation.
3DCeram Sinto. Biomedical ceramic additive manufacturing solutions.
ISO 13485: Medical devices – Quality management systems.
European Union Medical Device Regulation (EU MDR 2017/745).
Frequently Asked Questions (FAQ)
Are 3D-printed hydroxyapatite implants safe?
Yes. When manufactured under certified medical device standards and used in appropriate indications, they demonstrate excellent biocompatibility and safety.
Do hydroxyapatite implants resorb over time?
Pure hydroxyapatite is slowly remodeled rather than rapidly resorbed. It integrates with native bone and may persist long-term as part of the skeletal structure.
Can these implants replace titanium plates?
In non-load-bearing or contour-focused applications, they may be a superior alternative. For high-mechanical-load scenarios, titanium or hybrid solutions may still be necessary.
Are they suitable for supporting dental implants?
In selected cases, HA implants may be used for bone augmentation; however, careful planning and case selection are essential.
Recent Articles
Introduction
Maxillofacial surgery often involves the reconstruction of complex bone defects caused by trauma, tumor resection, congenital deformities, or severe infections. Traditional reconstruction methods, such as autologous bone grafts, titanium plates, and polymer-based implants, have long been the standard of care. However, these approaches present well-known challenges, including donor site morbidity, limited anatomical precision, risk of long-term foreign body reactions, and suboptimal biological integration.
In recent years, 3D-printed hydroxyapatite (HA) implants have emerged as a promising, biologically driven alternative. By combining additive manufacturing with a bone-mimicking bioceramic, these implants offer patient-specific geometry, enhanced osteointegration, and improved aesthetic and functional outcomes. As clinical evidence grows and regulatory approvals expand, 3D-printed hydroxyapatite implants are increasingly viewed as a next-generation solution for maxillofacial reconstruction.
This article provides a comprehensive, SEO-optimized overview of the technology, material science, clinical applications, commercially available products, advantages and limitations, and future outlook of 3D-printed hydroxyapatite implants in maxillofacial surgery.
Understanding Hydroxyapatite as a Biomaterial
What Is Hydroxyapatite?
Hydroxyapatite (chemical formula: Ca₁₀(PO₄)₆(OH)₂) is a naturally occurring calcium phosphate mineral that constitutes approximately 60–70% of human bone by weight and nearly 90% of dental enamel. Because of this close chemical and structural similarity to native bone, hydroxyapatite has been widely used in orthopedics, dentistry, and cranio-maxillofacial surgery for decades.
Key Biological Properties
Hydroxyapatite is valued in implantology due to several critical characteristics:
Excellent biocompatibility, with minimal inflammatory or immune response
Osteoconductivity, allowing bone cells to migrate along its surface
Bioactivity, enabling direct chemical bonding between the implant and the host bone
Surface affinity for proteins and osteoblasts, promoting bone regeneration
Unlike inert materials such as titanium or PEEK, hydroxyapatite does not simply occupy space; it actively participates in the bone healing process.
The Role of 3D Printing in Maxillofacial Implants
Additive Manufacturing and Patient-Specific Implants
3D printing, also known as additive manufacturing, enables the production of patient-specific implants (PSIs) based on CT or CBCT imaging data. Using digital planning software, surgeons and biomedical engineers can design implants that precisely replicate the patient’s anatomy and defect geometry.
For maxillofacial surgery, where millimeter-level accuracy affects occlusion, facial symmetry, and orbital support, this level of customization represents a major clinical advantage.
Controlled Porosity and Internal Architecture
One of the most important benefits of 3D printing hydroxyapatite is the ability to control internal porosity and pore interconnectivity. These structural features are essential for:
Vascular ingrowth
Nutrient diffusion
Bone cell migration
Long-term osteointegration
Well-designed porous HA implants function as three-dimensional scaffolds, gradually becoming integrated with living bone rather than remaining as isolated foreign bodies.
Clinical Applications in Maxillofacial Surgery
3D-printed hydroxyapatite implants are primarily used in non-load-bearing or moderately load-bearing maxillofacial reconstructions, where biological integration and anatomical accuracy are priorities.
Common Indications
Mandibular and maxillary bone defects following tumor resection
Zygomatic and midface reconstruction after trauma
Orbital floor and orbital wall reconstruction
Facial contour restoration for aesthetic and functional rehabilitation
Bone augmentation before dental implant placement (select cases)
In many of these scenarios, HA implants reduce or eliminate the need for autologous bone harvesting, thereby avoiding donor site complications.
Commercially Available 3D-Printed Hydroxyapatite Implants
Although still an emerging segment of the implant market, several clinically approved products and solutions are already available.
MyBone® Custom Implants (Cerhum, Belgium)
MyBone® is one of the most recognized commercial examples of a 3D-printed hydroxyapatite patient-specific implant for maxillofacial and craniofacial reconstruction.
Key Features:
Medical-grade porous hydroxyapatite
Fully patient-specific design based on CT imaging
Optimized pore architecture for vascularization and bone ingrowth
CE-marked under the European Medical Device Regulation (MDR)
Manufactured under ISO 13485 quality standards
Clinical case series have demonstrated excellent implant stability, absence of infection or displacement, and progressive osteointegration over follow-up periods.
BioCranium® and Custom HA Implants (3DCeram, France)
3DCeram provides advanced 3D-printed ceramic implants, including hydroxyapatite-based solutions for cranial and facial reconstruction. Their technology focuses on high-precision ceramic additive manufacturing with controlled micro- and macro-porosity.
These implants are typically used in complex cranio-maxillofacial defects where traditional materials may compromise biological integration or aesthetics.
Hydroxyapatite Materials for Custom Manufacturing
In addition to finished implants, medical-grade hydroxyapatite powders are supplied by specialized biomaterials companies. These materials are used by manufacturers, research institutions, and hospital-based 3D printing centers to develop custom scaffolds, composite implants, and experimental devices.
LithaBone HA Hydroxyapatite ( Lithoz, Austria)
LithaBone HA is an advanced, 3D-printable form of hydroxyapatite specifically engineered for the fabrication of patient-specific ceramic bone implants. Hydroxyapatite is a naturally occurring mineral and the primary inorganic component of human bone, which makes it exceptionally compatible with the body. Its high biocompatibility and osteoconductive behavior allow bone cells to adhere, proliferate, and gradually grow through the implant structure after implantation.
Advantages of LithaBone
One of the key advantages of hydroxyapatite is its controlled resorption profile. Once implanted, the material is slowly resorbed by the body while new natural bone is formed simultaneously. This process eliminates the need for secondary surgery to remove the implant and significantly reduces patient trauma and overall treatment costs. Compared to other bone substitute materials, hydroxyapatite resorbs at a slower rate, providing sufficient mechanical support and healing time, particularly in critical-sized bone defects that cannot heal on their own.
LithaBone HA has been optimized for additive manufacturing, offering high geometric freedom, tunable microporosity, and strong mechanical performance while remaining easy to handle during processing. Lithoz exclusively uses hydroxyapatite powders that comply with ASTM F1185 standards for surgical implants, ensuring high purity and controlled heavy metal content. The sintered ceramic exhibits excellent density, high bending strength, and proven biocompatibility in accordance with ISO 10993-5, making it a reliable solution for advanced bone regeneration applications.
Clinical Evidence and Outcomes
Published Case Series and Studies
Multiple peer-reviewed clinical reports have evaluated 3D-printed hydroxyapatite implants in maxillofacial reconstruction. Across these studies, key findings include:
High rates of implant survival
Low incidence of infection or inflammatory response
Progressive radiographic bone integration
Reduced need for intraoperative modification
Favorable aesthetic and functional outcomes
Surgeons consistently report improved surgical workflow due to precise preoperative planning and reduced operative time.
Advantages Over Traditional Materials
Biological Integration
Unlike titanium or polymer implants, hydroxyapatite actively bonds with host bone, creating a biological interface rather than a mechanical one.
Anatomical Precision
Patient-specific design ensures optimal fit, reduced dead space, and improved load distribution.
Reduced Donor Site Morbidity
By minimizing or eliminating the need for autologous bone grafts, HA implants reduce postoperative pain and complication risk.
Improved Aesthetics
Precise contour replication is especially important in visible facial regions, such as the zygoma and orbital rim.
Limitations and Considerations
Despite their advantages, 3D-printed hydroxyapatite implants have important limitations that must be considered.
Mechanical Strength
Hydroxyapatite is a brittle ceramic material, particularly when designed with high porosity. It is generally not suitable for high load-bearing applications without structural reinforcement or a hybrid design.
Cost and Production Time
Custom design, regulatory compliance, and specialized manufacturing increase cost compared to off-the-shelf implants.
Limited Long-Term Data
While short- and mid-term clinical outcomes are promising, large-scale, long-term comparative studies are still limited.
Future Directions and Innovations
Ongoing research aims to overcome current limitations and expand clinical indications. Key areas of development include:
Composite implants combining HA with polymers or bioresorbable materials
Doped hydroxyapatite (e.g., silicon- or magnesium-substituted HA) for enhanced bioactivity
Hybrid metal-ceramic designs for improved mechanical performance
Integration of growth factors or stem-cell-friendly surfaces
As these technologies mature, 3D-printed hydroxyapatite implants are expected to play a growing role in personalized maxillofacial surgery.
Conclusion
3D-printed hydroxyapatite implants represent a significant advancement in biologically driven, patient-specific maxillofacial reconstruction. By combining the osteoconductive properties of hydroxyapatite with the precision of additive manufacturing, these implants address many of the limitations of traditional reconstruction methods.
While challenges remain—particularly in mechanical strength and long-term clinical data—the current evidence and expanding commercial availability suggest that hydroxyapatite-based 3D-printed implants will become an increasingly important tool in modern maxillofacial surgery.
References
Dorozhkin SV. Calcium orthophosphates in nature, biology, and medicine. Materials.
Campana V, Milano G, Pagano E, et al. Bone substitutes in orthopaedic surgery: from basic science to clinical practice. J Mater Sci Mater Med.
Mangano C, Bianchi A, Mangano FG, et al. Custom-made 3D printed hydroxyapatite scaffolds for bone regeneration. J Craniofac Surg.
Cerhum SA. MyBone® Custom Hydroxyapatite Implants – Technical and Clinical Documentation.
3DCeram Sinto. Biomedical ceramic additive manufacturing solutions.
ISO 13485: Medical devices – Quality management systems.
European Union Medical Device Regulation (EU MDR 2017/745).
Frequently Asked Questions (FAQ)
Are 3D-printed hydroxyapatite implants safe?
Yes. When manufactured under certified medical device standards and used in appropriate indications, they demonstrate excellent biocompatibility and safety.
Do hydroxyapatite implants resorb over time?
Pure hydroxyapatite is slowly remodeled rather than rapidly resorbed. It integrates with native bone and may persist long-term as part of the skeletal structure.
Can these implants replace titanium plates?
In non-load-bearing or contour-focused applications, they may be a superior alternative. For high-mechanical-load scenarios, titanium or hybrid solutions may still be necessary.
Are they suitable for supporting dental implants?
In selected cases, HA implants may be used for bone augmentation; however, careful planning and case selection are essential.
Recent Articles
Peri-Implantitis Treatment & Prevention Methods
Peri-Implantitis Treatment & Prevention Methods Peri-implantitis remains one of the most significant biological complications affecting dental implants, posing a serious threat to long-term implant [...]
Latest Sinus Lifting Techniques in Modern Implant Dentistry
Latest Sinus Lifting Techniques in Modern Implant Dentistry A Comprehensive Clinical Review Introduction to Sinus Lifting in Implantology Sinus lifting, or maxillary sinus floor [...]
Biomechanics of the Triple Abutment & BOPiT Concept
Dental Biomechanics · Implant Science · Clinical Evidence Biomechanics of the Triple Abutment & BOPiT Concept How a saddle-shaped mathematical surface is rewriting the rules of load distribution [...]
The Woman Who Proved One Implant Could Hold Three Crowns
The Woman Who Proved One Implant Could Hold Three Crowns While the dental establishment looked away, Dr. Luciana Colepícolo spent 12 years building the [...]
ENPP1, The Molecular Brake That Limits Tissue Healing
ENPP1, The Molecular Brake That Limits Tissue Healing Introduction: A New Biological Barrier to Dental Regeneration Meet ENPP1—a protein most dentists have never heard [...]
The Rise of Self‑Healing Dental Biomaterials
The Rise of Self‑Healing Dental Biomaterials Introduction In modern restorative dentistry, durability and longevity of materials remain among the greatest clinical challenges. Traditional dental [...]