Treating TMJ Arthritis with Collagen Injection
Treating TMJ Arthritis with Collagen Injection
Treating TMJ Arthritis with Collagen Injection
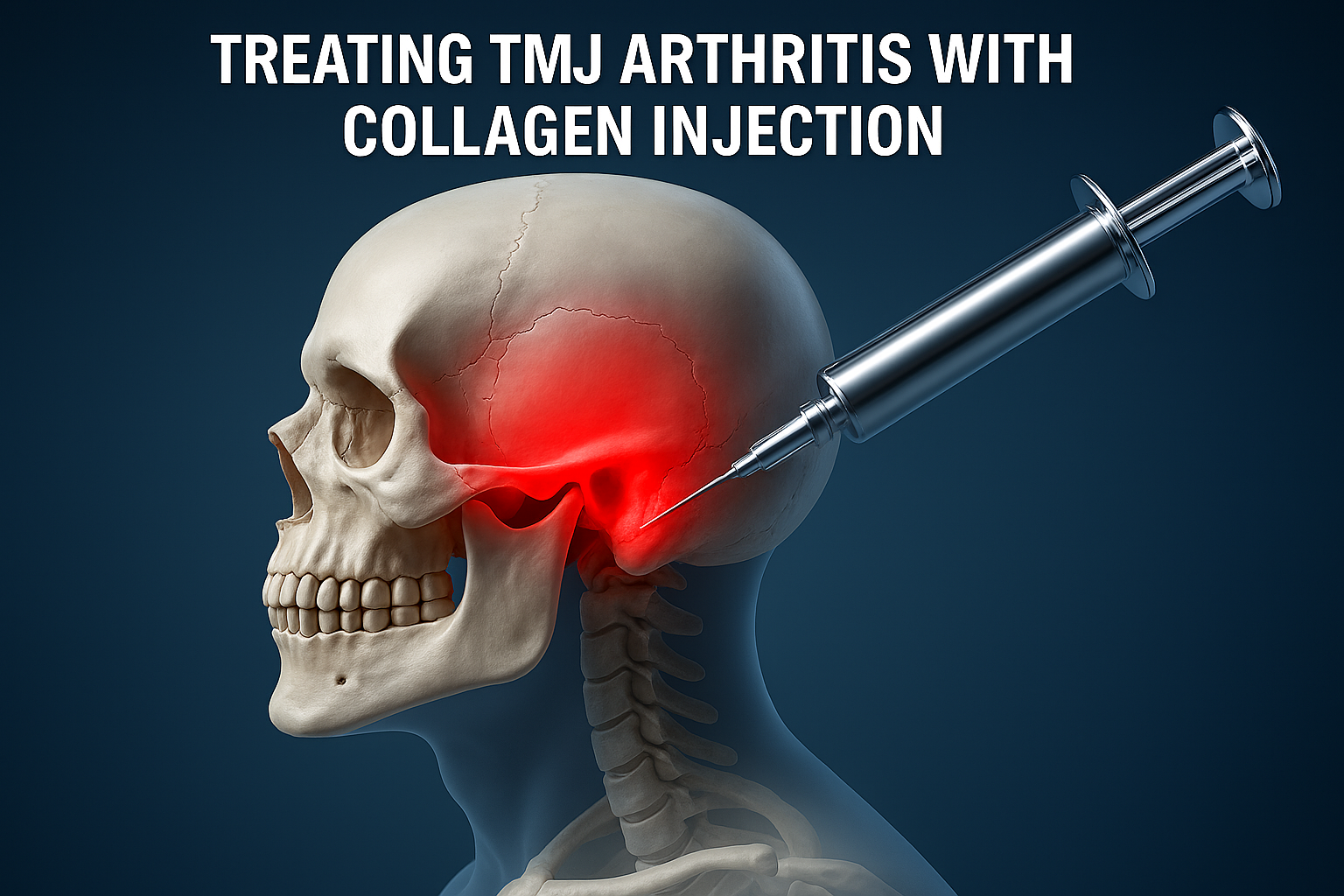
TMJ Arthritis is a painful condition affecting the temporomandibular joint that connects your jaw to your skull, and can significantly impact daily life. It causes jaw stiffness, pain while chewing, and limited mouth movement. While traditional treatments focus on pain management and physiotherapy, recent advances in regenerative medicine are offering promising new solutions. One such innovation is the use of collagen injections to restore joint health, reduce inflammation, and improve mobility in patients suffering from TMJ Arthritis.
Understanding TMJ Arthritis: Causes and Symptoms
TMJ Arthritis is an inflammatory condition that affects the jaw joint and surrounding muscles. It may result from osteoarthritis, rheumatoid arthritis, or trauma to the joint. The inflammation leads to the breakdown of cartilage—the smooth tissue that cushions joint movement—causing friction, stiffness, and pain.
Common symptoms include:
- Clicking or popping sounds when opening the mouth
- Pain radiating to the ear, temple, or neck
- Difficulty chewing or speaking
- Swelling around the jaw joint
- Limited mouth opening
Without early treatment, TMJ Arthritis can cause joint degeneration, bone erosion, and chronic discomfort that affects nutrition, speech, and sleep.
Why Collagen Matters in Joint Health
Collagen is the body’s most abundant protein and a major structural component of cartilage, bones, and connective tissues. In the jaw joint, collagen maintains elasticity, shock absorption, and smooth motion. When inflammation damages the cartilage in TMJ Arthritis, collagen loss accelerates joint wear, leading to pain and stiffness.
Traditional therapies like anti-inflammatory drugs and mouthguards may reduce symptoms, but do not restore lost collagen or repair cartilage. That’s where collagen injections come in—targeting the biological root of joint degradation rather than only managing pain.
How Collagen Injections Treat TMJ Arthritis
Collagen injection therapy involves administering a sterile, biocompatible collagen-based gel directly into the affected temporomandibular joint. The injected collagen serves as a biological scaffold that supports tissue repair and stimulates the body’s own regenerative processes.
Mechanism of action:
- The injected collagen fills microscopic defects in the cartilage surface.
- It promotes cellular migration and the growth of new cartilage tissue.
- The gel also improves joint lubrication, reducing friction and pain.
- Over time, the body absorbs the gel while replacing it with newly regenerated tissue.
In several clinical settings, collagen injections have been shown to decrease joint inflammation, improve mouth opening range, and provide long-term relief for patients with mild to moderate TMJ Arthritis.
Advantages of Collagen Injection Over Traditional TMJ Arthritis Treatments
Unlike invasive surgical procedures such as joint replacement or arthroscopy, collagen injections are minimally invasive and can be performed under local anesthesia. The recovery time is short, and most patients can resume normal activities within 24–48 hours.
Key benefits include:
- Natural tissue regeneration instead of artificial joint replacement
- Reduced inflammation and improved lubrication
- Minimized side effects and faster recovery
- Improved joint flexibility and function
- Potential delay or avoidance of surgical intervention
Recent studies in regenerative dentistry and orthopedics suggest that combining collagen injections with physiotherapy and occlusal balance correction can significantly enhance patient outcomes and comfort levels.
Who Can Benefit from Collagen Injection Therapy for TMJ Arthritis?
Collagen injection therapy is most suitable for patients with early to moderate stages of TMJ Arthritis who experience pain, stiffness, or functional limitation but do not yet require surgery. Candidates typically include:
- Patients with mild joint degeneration
- Individuals unresponsive to conservative therapies (NSAIDs, splints, etc.)
- Those seeking a natural, regenerative alternative to surgery
- Patients with contraindications for invasive surgical interventions
However, patients with severe joint damage or bone fusion may not benefit fully and could require surgical reconstruction. A maxillofacial or TMJ specialist can determine eligibility through clinical evaluation and imaging studies.
The Regenerative Effect of Chondrofiller: Between Facts and Hopes
Recently, a collagen-based injectable material known as chondrofiller has gained attention for its potential to regenerate cartilage in orthopedic and maxillofacial applications. While promotional materials and case reports suggest that it can fill cartilage defects and stimulate natural tissue regeneration, it is essential to approach such claims with scientific caution.
As of now, there are no large-scale, peer-reviewed clinical trials confirming the effectiveness of chondrofiller in treating TMJ Arthritis or regenerating cartilage in the temporomandibular joint. Most available evidence comes from in vitro (lab-based) studies or small case series focused on larger joints such as the knee. Moreover, recent comparative studies have shown no statistically significant difference in clinical outcomes between collagen injections and hyaluronic acid (HA) injections for managing TMJ arthritis. Both materials appear to provide temporary symptomatic relief—mainly by improving joint lubrication and reducing inflammation—rather than demonstrating true cartilage regeneration.
These findings emphasize that while collagen-based fillers like Chondrofiller are biocompatible and safe, their regenerative potential remains unproven. The complex biomechanics and limited vascularization of the TMJ make it a particularly challenging target for tissue engineering. Future research should include randomized controlled trials with imaging and histological validation to determine whether these biomaterials can achieve genuine structural regeneration or primarily serve as temporary supportive matrices.
In conclusion, while chondrofiller and similar collagen products represent an exciting frontier in regenerative dentistry and orthopedics, current evidence should be interpreted as preliminary and hopeful, rather than conclusive. Clinicians are encouraged to rely on established, evidence-based therapies and remain attentive to forthcoming scientific evaluations.
The Future of Regenerative Treatments for TMJ Arthritis
Collagen-based therapies represent a growing area of research within regenerative dentistry and orthopedic medicine. Advanced formulations are being developed that combine collagen with stem cells, hyaluronic acid, or growth factors to further enhance tissue regeneration.
Germany, for example, has pioneered collagen gel technologies used in orthopedic cartilage repair, and similar approaches are now being adapted for the temporomandibular joint. As clinical trials expand, these innovations could become standard treatment options in the next decade—offering hope for millions living with chronic jaw pain and joint degeneration.
Integrating collagen therapy with preventive dental care, posture correction, and stress management could provide a holistic approach to managing TMJ Arthritis sustainably and effectively.
Final Thoughts
The evolution of regenerative medicine has opened new doors for managing complex joint conditions like TMJ Arthritis. Collagen injection therapy stands at the forefront of these innovations, offering a natural and minimally invasive alternative that not only relieves pain but promotes genuine tissue healing. As research progresses, it holds the potential to redefine how dental and medical professionals approach joint care—focusing not just on symptom control, but on true regeneration.
FAQs About Treating TMJ Arthritis with Collagen Injection
1. Is collagen injection safe for TMJ Arthritis?
Yes. Collagen injections use biocompatible materials similar to the body’s natural collagen. When administered by a trained dental or maxillofacial professional, the procedure is safe with minimal risks.
2. How long do results from collagen injections last?
Many patients experience relief for 6 to 18 months, depending on the severity of joint damage and individual healing responses. Repeat treatments may be needed to maintain long-term benefits.
3. Does the procedure hurt?
The treatment is typically performed under local anesthesia. Most patients report mild discomfort or temporary soreness at the injection site, which subsides within a few days.
4. How is this different from hyaluronic acid injections?
While hyaluronic acid primarily improves joint lubrication, collagen injections focus on tissue regeneration—stimulating the body’s ability to repair damaged cartilage and restore structure.
5. Are collagen injections approved for TMJ use?
Collagen-based injectables are approved for various medical uses in Europe and are under evaluation in TMJ applications. Always consult a certified specialist for safe and evidence-based treatment options.
References
- Meidrix Biomedicals. “ChondroFiller®: Collagen-Based Matrix for Cartilage Repair.”
- A New Frontier in Temporomandibular Joint Osteoarthritis – Regenerative Medicine Approaches (Frontiers in Bioengineering and Biotechnology, 2022)
- “Temporomandibular Joint Disorders: A Review of Etiology…” (Murphy MK et al., 2013) — PMC
- Sciencedirect. “Injectable Hydrogels for Cartilage Tissue Engineering.” ScienceDirect, 2023.
- American Academy of Orofacial Pain. “Management of Temporomandibular Disorders and Occlusion.” 2022 Guidelines.
- A comparative intra-articular injection study (Koca et al., 2023) related to TMJ OA
Recent Articles
TMJ Arthritis is a painful condition affecting the temporomandibular joint that connects your jaw to your skull, and can significantly impact daily life. It causes jaw stiffness, pain while chewing, and limited mouth movement. While traditional treatments focus on pain management and physiotherapy, recent advances in regenerative medicine are offering promising new solutions. One such innovation is the use of collagen injections to restore joint health, reduce inflammation, and improve mobility in patients suffering from TMJ Arthritis.
Understanding TMJ Arthritis: Causes and Symptoms
TMJ Arthritis is an inflammatory condition that affects the jaw joint and surrounding muscles. It may result from osteoarthritis, rheumatoid arthritis, or trauma to the joint. The inflammation leads to the breakdown of cartilage—the smooth tissue that cushions joint movement—causing friction, stiffness, and pain.
Common symptoms include:
- Clicking or popping sounds when opening the mouth
- Pain radiating to the ear, temple, or neck
- Difficulty chewing or speaking
- Swelling around the jaw joint
- Limited mouth opening
Without early treatment, TMJ Arthritis can cause joint degeneration, bone erosion, and chronic discomfort that affects nutrition, speech, and sleep.
Why Collagen Matters in Joint Health
Collagen is the body’s most abundant protein and a major structural component of cartilage, bones, and connective tissues. In the jaw joint, collagen maintains elasticity, shock absorption, and smooth motion. When inflammation damages the cartilage in TMJ Arthritis, collagen loss accelerates joint wear, leading to pain and stiffness.
Traditional therapies like anti-inflammatory drugs and mouthguards may reduce symptoms, but do not restore lost collagen or repair cartilage. That’s where collagen injections come in—targeting the biological root of joint degradation rather than only managing pain.
How Collagen Injections Treat TMJ Arthritis
Collagen injection therapy involves administering a sterile, biocompatible collagen-based gel directly into the affected temporomandibular joint. The injected collagen serves as a biological scaffold that supports tissue repair and stimulates the body’s own regenerative processes.
Mechanism of action:
- The injected collagen fills microscopic defects in the cartilage surface.
- It promotes cellular migration and the growth of new cartilage tissue.
- The gel also improves joint lubrication, reducing friction and pain.
- Over time, the body absorbs the gel while replacing it with newly regenerated tissue.
In several clinical settings, collagen injections have been shown to decrease joint inflammation, improve mouth opening range, and provide long-term relief for patients with mild to moderate TMJ Arthritis.
Advantages of Collagen Injection Over Traditional TMJ Arthritis Treatments
Unlike invasive surgical procedures such as joint replacement or arthroscopy, collagen injections are minimally invasive and can be performed under local anesthesia. The recovery time is short, and most patients can resume normal activities within 24–48 hours.
Key benefits include:
- Natural tissue regeneration instead of artificial joint replacement
- Reduced inflammation and improved lubrication
- Minimized side effects and faster recovery
- Improved joint flexibility and function
- Potential delay or avoidance of surgical intervention
Recent studies in regenerative dentistry and orthopedics suggest that combining collagen injections with physiotherapy and occlusal balance correction can significantly enhance patient outcomes and comfort levels.
Who Can Benefit from Collagen Injection Therapy for TMJ Arthritis?
Collagen injection therapy is most suitable for patients with early to moderate stages of TMJ Arthritis who experience pain, stiffness, or functional limitation but do not yet require surgery. Candidates typically include:
- Patients with mild joint degeneration
- Individuals unresponsive to conservative therapies (NSAIDs, splints, etc.)
- Those seeking a natural, regenerative alternative to surgery
- Patients with contraindications for invasive surgical interventions
However, patients with severe joint damage or bone fusion may not benefit fully and could require surgical reconstruction. A maxillofacial or TMJ specialist can determine eligibility through clinical evaluation and imaging studies.
The Regenerative Effect of Chondrofiller: Between Facts and Hopes
Recently, a collagen-based injectable material known as chondrofiller has gained attention for its potential to regenerate cartilage in orthopedic and maxillofacial applications. While promotional materials and case reports suggest that it can fill cartilage defects and stimulate natural tissue regeneration, it is essential to approach such claims with scientific caution.
As of now, there are no large-scale, peer-reviewed clinical trials confirming the effectiveness of chondrofiller in treating TMJ Arthritis or regenerating cartilage in the temporomandibular joint. Most available evidence comes from in vitro (lab-based) studies or small case series focused on larger joints such as the knee. Moreover, recent comparative studies have shown no statistically significant difference in clinical outcomes between collagen injections and hyaluronic acid (HA) injections for managing TMJ arthritis. Both materials appear to provide temporary symptomatic relief—mainly by improving joint lubrication and reducing inflammation—rather than demonstrating true cartilage regeneration.
These findings emphasize that while collagen-based fillers like Chondrofiller are biocompatible and safe, their regenerative potential remains unproven. The complex biomechanics and limited vascularization of the TMJ make it a particularly challenging target for tissue engineering. Future research should include randomized controlled trials with imaging and histological validation to determine whether these biomaterials can achieve genuine structural regeneration or primarily serve as temporary supportive matrices.
In conclusion, while chondrofiller and similar collagen products represent an exciting frontier in regenerative dentistry and orthopedics, current evidence should be interpreted as preliminary and hopeful, rather than conclusive. Clinicians are encouraged to rely on established, evidence-based therapies and remain attentive to forthcoming scientific evaluations.
The Future of Regenerative Treatments for TMJ Arthritis
Collagen-based therapies represent a growing area of research within regenerative dentistry and orthopedic medicine. Advanced formulations are being developed that combine collagen with stem cells, hyaluronic acid, or growth factors to further enhance tissue regeneration.
Germany, for example, has pioneered collagen gel technologies used in orthopedic cartilage repair, and similar approaches are now being adapted for the temporomandibular joint. As clinical trials expand, these innovations could become standard treatment options in the next decade—offering hope for millions living with chronic jaw pain and joint degeneration.
Integrating collagen therapy with preventive dental care, posture correction, and stress management could provide a holistic approach to managing TMJ Arthritis sustainably and effectively.
Final Thoughts
The evolution of regenerative medicine has opened new doors for managing complex joint conditions like TMJ Arthritis. Collagen injection therapy stands at the forefront of these innovations, offering a natural and minimally invasive alternative that not only relieves pain but promotes genuine tissue healing. As research progresses, it holds the potential to redefine how dental and medical professionals approach joint care—focusing not just on symptom control, but on true regeneration.
FAQs About Treating TMJ Arthritis with Collagen Injection
1. Is collagen injection safe for TMJ Arthritis?
Yes. Collagen injections use biocompatible materials similar to the body’s natural collagen. When administered by a trained dental or maxillofacial professional, the procedure is safe with minimal risks.
2. How long do results from collagen injections last?
Many patients experience relief for 6 to 18 months, depending on the severity of joint damage and individual healing responses. Repeat treatments may be needed to maintain long-term benefits.
3. Does the procedure hurt?
The treatment is typically performed under local anesthesia. Most patients report mild discomfort or temporary soreness at the injection site, which subsides within a few days.
4. How is this different from hyaluronic acid injections?
While hyaluronic acid primarily improves joint lubrication, collagen injections focus on tissue regeneration—stimulating the body’s ability to repair damaged cartilage and restore structure.
5. Are collagen injections approved for TMJ use?
Collagen-based injectables are approved for various medical uses in Europe and are under evaluation in TMJ applications. Always consult a certified specialist for safe and evidence-based treatment options.
References
- Meidrix Biomedicals. “ChondroFiller®: Collagen-Based Matrix for Cartilage Repair.”
- A New Frontier in Temporomandibular Joint Osteoarthritis – Regenerative Medicine Approaches (Frontiers in Bioengineering and Biotechnology, 2022)
- “Temporomandibular Joint Disorders: A Review of Etiology…” (Murphy MK et al., 2013) — PMC
- Sciencedirect. “Injectable Hydrogels for Cartilage Tissue Engineering.” ScienceDirect, 2023.
- American Academy of Orofacial Pain. “Management of Temporomandibular Disorders and Occlusion.” 2022 Guidelines.
- A comparative intra-articular injection study (Koca et al., 2023) related to TMJ OA
Recent Articles
Peri-Implantitis Treatment & Prevention Methods
Peri-Implantitis Treatment & Prevention Methods Peri-implantitis remains one of the most significant biological complications affecting dental implants, posing a serious threat to long-term implant [...]
Latest Sinus Lifting Techniques in Modern Implant Dentistry
Latest Sinus Lifting Techniques in Modern Implant Dentistry A Comprehensive Clinical Review Introduction to Sinus Lifting in Implantology Sinus lifting, or maxillary sinus floor [...]
Biomechanics of the Triple Abutment & BOPiT Concept
Dental Biomechanics · Implant Science · Clinical Evidence Biomechanics of the Triple Abutment & BOPiT Concept How a saddle-shaped mathematical surface is rewriting the rules of load distribution [...]
The Woman Who Proved One Implant Could Hold Three Crowns
The Woman Who Proved One Implant Could Hold Three Crowns While the dental establishment looked away, Dr. Luciana Colepícolo spent 12 years building the [...]
ENPP1, The Molecular Brake That Limits Tissue Healing
ENPP1, The Molecular Brake That Limits Tissue Healing Introduction: A New Biological Barrier to Dental Regeneration Meet ENPP1—a protein most dentists have never heard [...]
The Rise of Self‑Healing Dental Biomaterials
The Rise of Self‑Healing Dental Biomaterials Introduction In modern restorative dentistry, durability and longevity of materials remain among the greatest clinical challenges. Traditional dental [...]