Tubarial Glands: The Nasopharynx Hidden Salivary Glands
Introduction: A Hidden Anatomical Surprise
In 2020, scientists made a discovery that shook the foundations of human anatomy—a previously undocumented pair of salivary glands nestled deep within the nasopharynx. These tubarial glands, located near the torus tubarius, were revealed through advanced imaging techniques and have since become a focal point in discussions about head and neck physiology, cancer treatment, and anatomical classification. Their rediscovery after centuries of anatomical study proves that the human body still holds secrets waiting to be uncovered.
The Discovery of Tubarial Glands: A 300-Year Mystery Solved
The tubarial glands were discovered by researchers at the Netherlands Cancer Institute during prostate cancer imaging using PSMA PET/CT scans (1). This imaging technique, designed to detect prostate-specific membrane antigen (PSMA), unexpectedly highlighted a consistent bilateral structure in the nasopharynx across 100 patients. These hotspots were located near the torus tubarius, an area previously thought to contain only microscopic mucous glands.
Histological analysis confirmed that these structures were mucous-secreting glands with ducts, resembling salivary glands. The discovery was so unexpected that it was described as the first identification of a new salivary gland structure in over 300 years (1).
Tubarial Glands in the Nasopharynx: Anatomy and Function
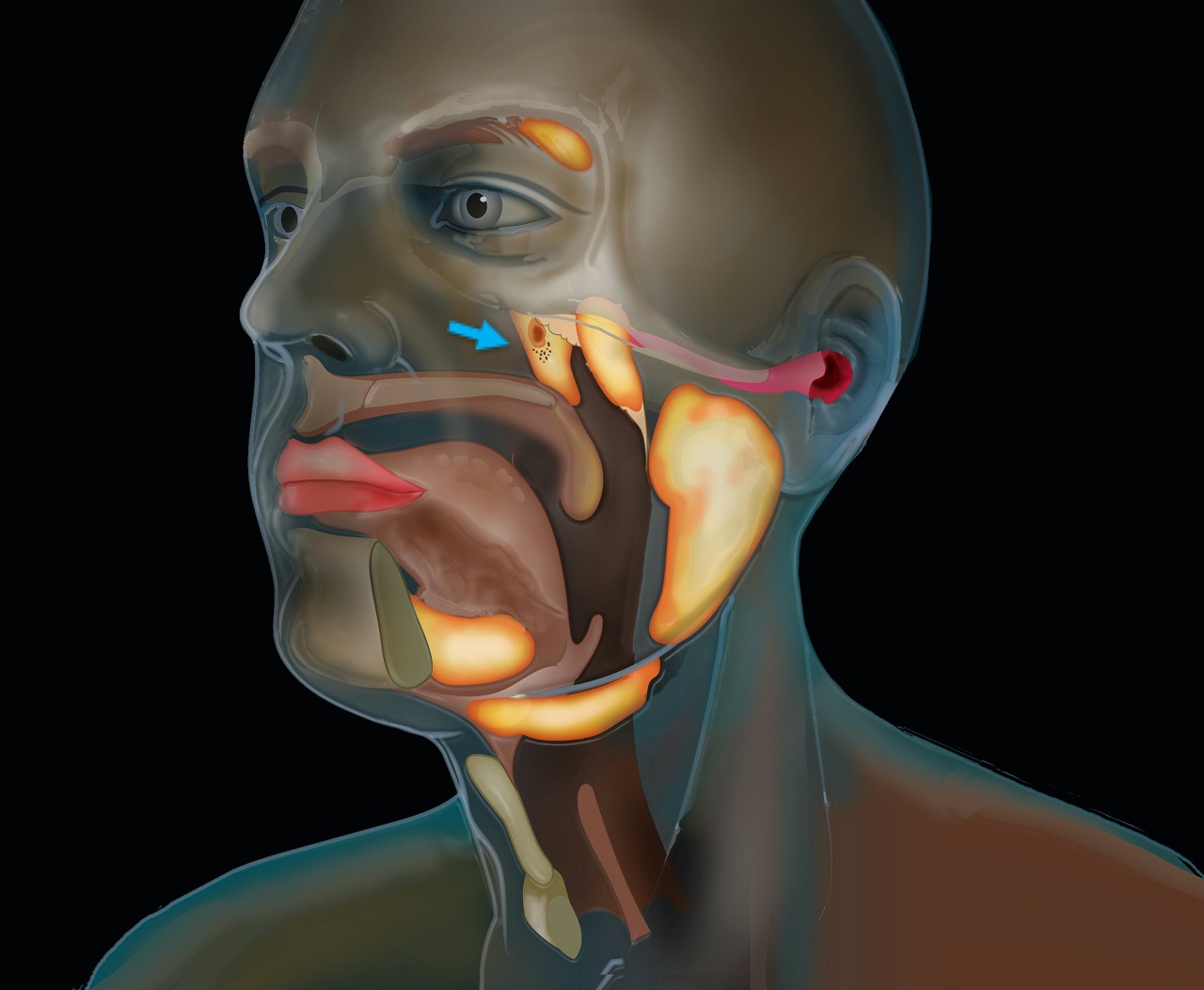
The tubarial glands are bilaterally located in the posterolateral wall of the nasopharynx, just above the soft palate and behind the nasal cavity (2). They are embedded within mucosal tissue and lack a distinct capsule, making them difficult to detect using traditional imaging methods like MRI.
Functionally, these glands are believed to lubricate and moisten the upper airway, aiding in swallowing, speech, and maintaining mucosal health (1). Their mucinous secretions may also help regulate pH and provide immune protection in the nasopharyngeal region.
Tubarial Glands and Radiotherapy: A New Organ at Risk?
One of the most significant implications of the tubarial glands' discovery lies in radiotherapy for head and neck cancers. Radiation-induced damage to salivary glands often leads to xerostomia (dry mouth) and dysphagia (difficulty swallowing). Until recently, the nasopharynx was not considered a site of major salivary gland activity, and radiation plans did not account for glandular preservation in this region (1).
A retrospective study of over 700 cancer patients revealed that radiation exposure to the tubarial glands correlated with increased treatment complications, including difficulty speaking and swallowing (1). This has prompted oncologists to reconsider treatment protocols and explore ways to spare the tubarial glands during radiotherapy, potentially improving patient outcomes and quality of life.
Tubarial Glands: Major or Minor Salivary Glands?
Despite their visibility on PSMA PET/CT scans and functional similarities to other salivary glands, the classification of tubarial glands remains debated. Traditionally, salivary glands are divided into three major pairs—parotid, submandibular, and sublingual—and hundreds of minor glands scattered throughout the mucosa.
Histological studies show that tubarial glands resemble minor salivary glands in structure, with densely packed mucinous acini and fewer ducts (2). Their lack of encapsulation and limited ductal branching further supports their categorization as minor glands. While some researchers proposed classifying them as a "fourth major salivary gland," this is not yet supported by anatomical consensus (2).
Sex-Based Differences in Tubarial Glands: What the Research Shows
Recent studies have uncovered sex-based differences in the structure and function of tubarial glands. A comprehensive histological analysis revealed that male tubarial glands had larger mucinous acini compared to females (2). This suggests potential differences in glandular secretion and function between sexes, which could influence treatment outcomes in radiotherapy.
Understanding these differences is crucial for personalized medicine, especially in tailoring radiation doses and predicting side effects. As imaging and histological techniques improve, further research may uncover additional sex-specific anatomical variations in salivary gland function.
Embryological Origin of Tubarial Glands: Still a Mystery
The embryological origin of tubarial glands remains unclear. Most salivary glands develop from epithelial buds in the oral cavity during the sixth to eighth week of gestation (3). Whether tubarial glands share this developmental pathway or arise from a distinct lineage is still under investigation.
Some researchers suggest that these glands may originate from endodermal tissue, similar to other minor salivary glands (3). However, due to their unique location and structure, more embryological studies are needed to determine their developmental timeline and lineage.
Tubarial Glands in Clinical Practice: Future Directions
The discovery of the tubarial glands has opened new avenues for research and clinical practice. Their role in salivary gland tumors, radiation toxicity, and nasopharyngeal lubrication is being actively explored. Clinicians are now considering these glands in radiation planning, and anatomists are reevaluating their place in the salivary gland classification system.
Future studies may focus on:
- Mapping their neural and vascular supply
- Investigating their role in immune responses
- Exploring their potential involvement in nasopharyngeal diseases
As our understanding deepens, the tubarial glands may become a key anatomical and clinical consideration in head and neck medicine.
FAQs About Tubarial Glands
Q1: Are tubarial glands a newly discovered organ?
Not exactly. While they were first described over a century ago as minor glands, they were rediscovered in 2020 using PSMA PET/CT imaging. Their consistent visibility and structure led to renewed interest and recognition (1).
Q2: Do tubarial glands affect cancer treatment?
Yes. Radiation therapy targeting the nasopharynx can damage these glands, resulting in side effects such as dry mouth and difficulty swallowing. Sparing them during treatment may improve patient outcomes (1).
Q3: Are tubarial glands present in everyone?
Studies show that all 100 patients scanned during the initial discovery had these glands, suggesting they are a universal anatomical feature (1).
Q4: Can tubarial glands be classified as major salivary glands?
Currently, no. Despite their size and visibility, they lack the structural complexity and encapsulation of major glands. They are best classified as minor salivary glands (2).
Q5: Do men and women have different tubarial glands?
Yes. Research indicates sex-based differences in gland size and mucinous acini structure, which may influence gland function and treatment response (2).
Final Thoughts
The rediscovery of the tubarial glands is a powerful reminder that even in the age of advanced medicine, the human body continues to surprise us. These glands, hidden in plain sight, may hold the key to improving cancer care and enhancing our understanding of nasopharyngeal physiology. As research continues, their role in anatomy, pathology, and clinical practice will become clearer—potentially reshaping how we treat and understand diseases of the head and neck.
References:
2- A comprehensive analysis of the tubarial glands.
3- Embryological Development Of Salivary Glands
Recent Articles
Introduction: A Hidden Anatomical Surprise
In 2020, scientists made a discovery that shook the foundations of human anatomy—a previously undocumented pair of salivary glands nestled deep within the nasopharynx. These tubarial glands, located near the torus tubarius, were revealed through advanced imaging techniques and have since become a focal point in discussions about head and neck physiology, cancer treatment, and anatomical classification. Their rediscovery after centuries of anatomical study proves that the human body still holds secrets waiting to be uncovered.
The Discovery of Tubarial Glands: A 300-Year Mystery Solved
The tubarial glands were discovered by researchers at the Netherlands Cancer Institute during prostate cancer imaging using PSMA PET/CT scans (1). This imaging technique, designed to detect prostate-specific membrane antigen (PSMA), unexpectedly highlighted a consistent bilateral structure in the nasopharynx across 100 patients. These hotspots were located near the torus tubarius, an area previously thought to contain only microscopic mucous glands.
Histological analysis confirmed that these structures were mucous-secreting glands with ducts, resembling salivary glands. The discovery was so unexpected that it was described as the first identification of a new salivary gland structure in over 300 years (1).
Tubarial Glands in the Nasopharynx: Anatomy and Function
The tubarial glands are bilaterally located in the posterolateral wall of the nasopharynx, just above the soft palate and behind the nasal cavity (2). They are embedded within mucosal tissue and lack a distinct capsule, making them difficult to detect using traditional imaging methods like MRI.
Functionally, these glands are believed to lubricate and moisten the upper airway, aiding in swallowing, speech, and maintaining mucosal health (1). Their mucinous secretions may also help regulate pH and provide immune protection in the nasopharyngeal region.
Tubarial Glands and Radiotherapy: A New Organ at Risk?
One of the most significant implications of the tubarial glands' discovery lies in radiotherapy for head and neck cancers. Radiation-induced damage to salivary glands often leads to xerostomia (dry mouth) and dysphagia (difficulty swallowing). Until recently, the nasopharynx was not considered a site of major salivary gland activity, and radiation plans did not account for glandular preservation in this region (1).
A retrospective study of over 700 cancer patients revealed that radiation exposure to the tubarial glands correlated with increased treatment complications, including difficulty speaking and swallowing (1). This has prompted oncologists to reconsider treatment protocols and explore ways to spare the tubarial glands during radiotherapy, potentially improving patient outcomes and quality of life.
Tubarial Glands: Major or Minor Salivary Glands?
Despite their visibility on PSMA PET/CT scans and functional similarities to other salivary glands, the classification of tubarial glands remains debated. Traditionally, salivary glands are divided into three major pairs—parotid, submandibular, and sublingual—and hundreds of minor glands scattered throughout the mucosa.
Histological studies show that tubarial glands resemble minor salivary glands in structure, with densely packed mucinous acini and fewer ducts (2). Their lack of encapsulation and limited ductal branching further supports their categorization as minor glands. While some researchers proposed classifying them as a "fourth major salivary gland," this is not yet supported by anatomical consensus (2).
Sex-Based Differences in Tubarial Glands: What the Research Shows
Recent studies have uncovered sex-based differences in the structure and function of tubarial glands. A comprehensive histological analysis revealed that male tubarial glands had larger mucinous acini compared to females (2). This suggests potential differences in glandular secretion and function between sexes, which could influence treatment outcomes in radiotherapy.
Understanding these differences is crucial for personalized medicine, especially in tailoring radiation doses and predicting side effects. As imaging and histological techniques improve, further research may uncover additional sex-specific anatomical variations in salivary gland function.
Embryological Origin of Tubarial Glands: Still a Mystery
The embryological origin of tubarial glands remains unclear. Most salivary glands develop from epithelial buds in the oral cavity during the sixth to eighth week of gestation (3). Whether tubarial glands share this developmental pathway or arise from a distinct lineage is still under investigation.
Some researchers suggest that these glands may originate from endodermal tissue, similar to other minor salivary glands (3). However, due to their unique location and structure, more embryological studies are needed to determine their developmental timeline and lineage.
Tubarial Glands in Clinical Practice: Future Directions
The discovery of the tubarial glands has opened new avenues for research and clinical practice. Their role in salivary gland tumors, radiation toxicity, and nasopharyngeal lubrication is being actively explored. Clinicians are now considering these glands in radiation planning, and anatomists are reevaluating their place in the salivary gland classification system.
Future studies may focus on:
- Mapping their neural and vascular supply
- Investigating their role in immune responses
- Exploring their potential involvement in nasopharyngeal diseases
As our understanding deepens, the tubarial glands may become a key anatomical and clinical consideration in head and neck medicine.
FAQs About Tubarial Glands
Q1: Are tubarial glands a newly discovered organ?
Not exactly. While they were first described over a century ago as minor glands, they were rediscovered in 2020 using PSMA PET/CT imaging. Their consistent visibility and structure led to renewed interest and recognition (1).
Q2: Do tubarial glands affect cancer treatment?
Yes. Radiation therapy targeting the nasopharynx can damage these glands, resulting in side effects such as dry mouth and difficulty swallowing. Sparing them during treatment may improve patient outcomes (1).
Q3: Are tubarial glands present in everyone?
Studies show that all 100 patients scanned during the initial discovery had these glands, suggesting they are a universal anatomical feature (1).
Q4: Can tubarial glands be classified as major salivary glands?
Currently, no. Despite their size and visibility, they lack the structural complexity and encapsulation of major glands. They are best classified as minor salivary glands (2).
Q5: Do men and women have different tubarial glands?
Yes. Research indicates sex-based differences in gland size and mucinous acini structure, which may influence gland function and treatment response (2).
Final Thoughts
The rediscovery of the tubarial glands is a powerful reminder that even in the age of advanced medicine, the human body continues to surprise us. These glands, hidden in plain sight, may hold the key to improving cancer care and enhancing our understanding of nasopharyngeal physiology. As research continues, their role in anatomy, pathology, and clinical practice will become clearer—potentially reshaping how we treat and understand diseases of the head and neck.
References:
2- A comprehensive analysis of the tubarial glands.
3- Embryological Development Of Salivary Glands
Recent Articles
Peri-Implantitis Treatment & Prevention Methods
Peri-Implantitis Treatment & Prevention Methods Peri-implantitis remains one of the most significant biological complications affecting dental implants, posing a serious threat to long-term implant [...]
Latest Sinus Lifting Techniques in Modern Implant Dentistry
Latest Sinus Lifting Techniques in Modern Implant Dentistry A Comprehensive Clinical Review Introduction to Sinus Lifting in Implantology Sinus lifting, or maxillary sinus floor [...]
Biomechanics of the Triple Abutment & BOPiT Concept
Dental Biomechanics · Implant Science · Clinical Evidence Biomechanics of the Triple Abutment & BOPiT Concept How a saddle-shaped mathematical surface is rewriting the rules of load distribution [...]
The Woman Who Proved One Implant Could Hold Three Crowns
The Woman Who Proved One Implant Could Hold Three Crowns While the dental establishment looked away, Dr. Luciana Colepícolo spent 12 years building the [...]
ENPP1, The Molecular Brake That Limits Tissue Healing
ENPP1, The Molecular Brake That Limits Tissue Healing Introduction: A New Biological Barrier to Dental Regeneration Meet ENPP1—a protein most dentists have never heard [...]
The Rise of Self‑Healing Dental Biomaterials
The Rise of Self‑Healing Dental Biomaterials Introduction In modern restorative dentistry, durability and longevity of materials remain among the greatest clinical challenges. Traditional dental [...]