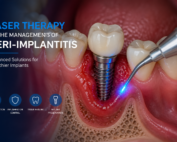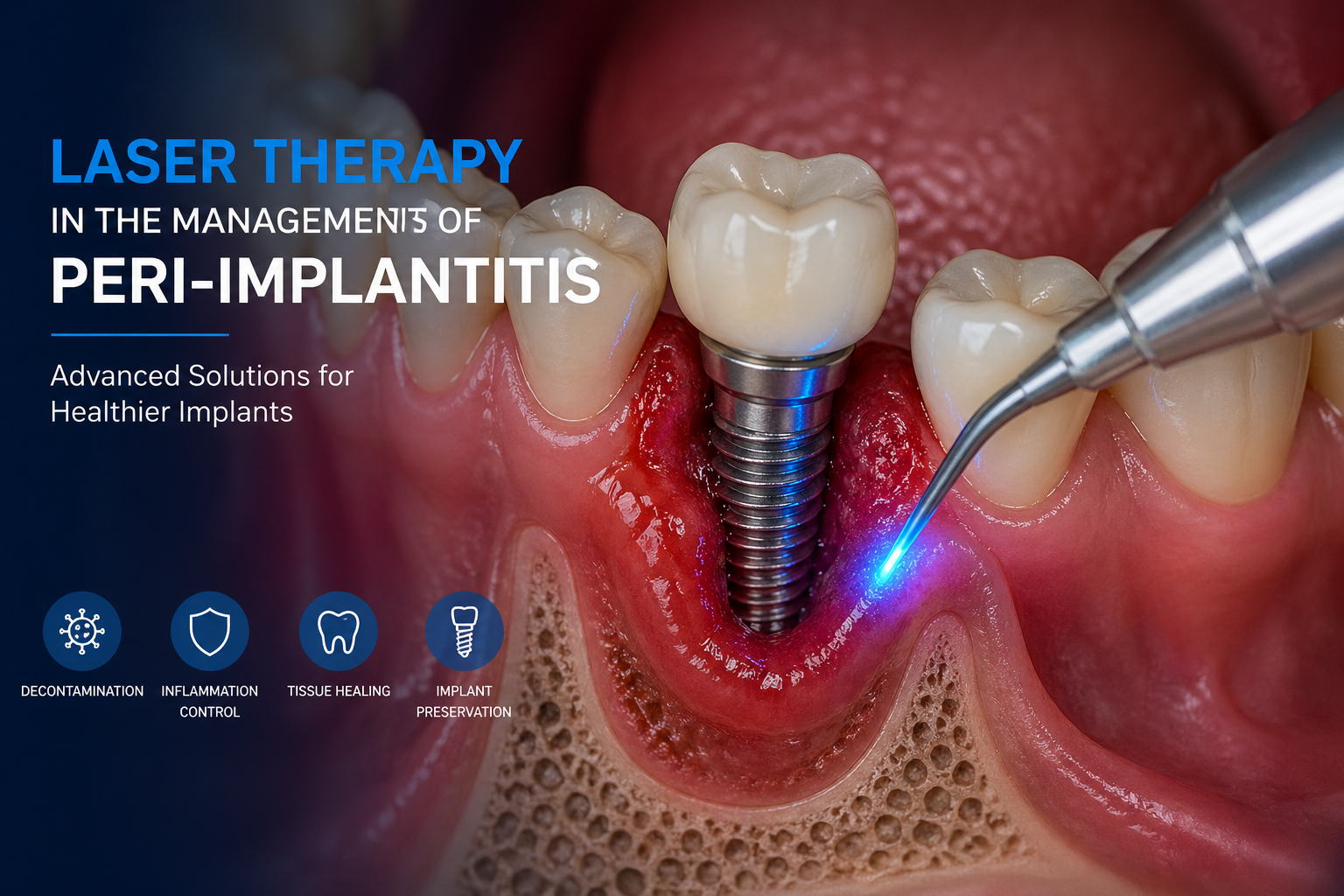
Laser Therapy in the Management of Peri-Implantitis
Laser technology has become an increasingly valuable adjunct in the treatment of peri-implant diseases, particularly peri-implantitis. Its ability to achieve effective bacterial reduction, detoxify implant surfaces, and promote soft tissue healing—while minimizing mechanical trauma—makes it highly attractive in modern implantology. Unlike conventional mechanical debridement alone, lasers provide **photothermal and photobiomodulation effects**, enhancing both antimicrobial efficacy and tissue response.
However, the clinical success of laser therapy depends heavily on selecting the appropriate wavelength, understanding tissue interaction, and applying correct protocols. Each wavelength operates within a specific absorption spectrum, targeting different chromophores such as water, hemoglobin, melanin, or bacterial pigments.
1. 450nm (Blue Laser): Precision Soft Tissue Surgery
The 450nm blue laser has emerged as a highly advanced tool in soft tissue management around implants. Its wavelength exhibits strong absorption in hemoglobin and melanin, making it exceptionally effective for **vascular soft tissue procedures**.
Clinical Characteristics
- Ultra-precise incision capability
- High affinity for hemoglobin → excellent hemostasis
- Minimal penetration depth → reduced collateral damage
- “Cold cutting” effect compared to traditional diode lasers
Applications in Peri-Implantitis
In peri-implantitis cases, the 450nm laser is particularly useful for:
- Removal of inflamed peri-implant soft tissue
- Granulation tissue excision during open flap procedures
- Soft tissue contouring around implants
Clinical Advantages
The key advantage lies in its ability to perform **atraumatic soft tissue surgery**. The minimal thermal diffusion reduces the risk of damaging surrounding bone and implant surfaces. This is critical in peri-implantitis, where preserving remaining bone is essential.
Additionally, patients benefit from:
- Reduced postoperative pain
- Minimal swelling
- Faster healing due to limited necrosis
2. 980nm (Near-Infrared Laser): Decontamination & Bacterial Reduction
The 980nm diode laser is one of the most widely used wavelengths in dentistry, particularly in periodontics and implantology. Its absorption in both water and hemoglobin allows for **deep penetration into soft tissues**, making it highly effective for bacterial reduction.
Mechanism of Action
- Photothermal effect → bacterial cell wall destruction
- Coagulation → reduces bleeding and improves visibility
- Moderate penetration → targets subgingival pathogens
Role in Peri-Implantitis Treatment
In peri-implantitis management, the 980nm laser is primarily used for:
- Disinfection of peri-implant pockets
- Reduction of anaerobic bacterial load
- Adjunctive therapy following mechanical debridement
Its ability to penetrate deeper than shorter wavelengths makes it effective in reaching bacteria located within micro-rough implant surfaces and surrounding tissues.
Additional Clinical Applications
- Activation of hydrogen peroxide-based whitening gels
- Soft tissue curettage
- Pocket sterilization in periodontal therapy
Limitations
Despite its effectiveness, excessive energy settings can lead to thermal damage to implant surfaces or surrounding bone. لذلك، precise calibration and controlled movement are essential.
3. 650nm (Red Laser): Low-Level Laser Therapy (LLLT)
The 650nm red laser operates at low power levels and is primarily used for **photobiomodulation therapy (PBMT)** rather than cutting or ablation. It plays a supportive role in peri-implantitis treatment by enhancing the body’s natural healing processes.
Biological Effects
- Stimulates mitochondrial activity → increased ATP production
- Enhances fibroblast proliferation
- Promotes collagen synthesis
- Reduces inflammatory mediators
Clinical Benefits in Peri-Implantitis
LLLT is particularly valuable in the post-treatment phase, حيث يساعد على:
- Accelerating soft tissue healing
- Reducing postoperative pain
- Minimizing inflammation
- Improving patient comfort
Use Cases
- After surgical peri-implantitis treatment
- Following laser or mechanical debridement
- Management of peri-implant mucositis
Although it does not directly eliminate bacteria, its regenerative effect significantly enhances overall treatment outcomes.
4. 2940nm Er:YAG Laser: Gold Standard for Hard Tissue & Implant Surface Decontamination
The 2940nm Er:YAG laser is widely considered one of the most effective laser systems for peri-implantitis treatment due to its **high absorption in water and hydroxyapatite**. This makes it uniquely capable of interacting with both soft and hard tissues without excessive الحرارة.
Mechanism of Action
- Micro-explosive ablation (photomechanical effect)
- Efficient removal of biofilm and calculus
- Minimal thermal penetration
Applications in Peri-Implantitis
- Implant surface decontamination
- Removal of granulation tissue
- Bone defect debridement
- Preparation for regenerative procedures
Key Advantages
The Er:YAG laser stands out because it can safely clean implant surfaces without altering their microstructure. This is critical for maintaining re-osseointegration potential.
- No carbonization or melting of titanium surface
- Effective biofilm removal from micro-rough surfaces
- Reduced need for aggressive mechanical instrumentation
Clinical Outcomes
Studies have shown that Er:YAG laser therapy can:
- Reduce probing depth
- Improve clinical attachment levels
- Enhance bone regeneration when combined with grafting
Clinical Integration Strategy
Optimal peri-implantitis management often involves a **combined laser approach**, rather than relying on a single wavelength:
- 450nm: Precise soft tissue surgery
- 980nm: Deep bacterial decontamination
- 650nm: Healing and pain modulation
- 2940nm Er:YAG: Implant surface cleaning and hard tissue management
This multimodal protocol allows clinicians to address all aspects of the disease: infection, inflammation, and tissue regeneration.
Conclusion
Laser therapy represents a paradigm shift in peri-implantitis treatment, offering minimally invasive, highly targeted, and biologically favorable outcomes. While no single wavelength can address all clinical needs, understanding the unique properties of each laser type allows clinicians to design comprehensive, evidence-based treatment protocols.
When integrated correctly, lasers not only improve decontamination efficiency but also enhance healing, reduce patient morbidity, and ultimately increase implant survival rates.
Recent Articles
Laser technology has become an increasingly valuable adjunct in the treatment of peri-implant diseases, particularly peri-implantitis. Its ability to achieve effective bacterial reduction, detoxify implant surfaces, and promote soft tissue healing—while minimizing mechanical trauma—makes it highly attractive in modern implantology. Unlike conventional mechanical debridement alone, lasers provide **photothermal and photobiomodulation effects**, enhancing both antimicrobial efficacy and tissue response.
However, the clinical success of laser therapy depends heavily on selecting the appropriate wavelength, understanding tissue interaction, and applying correct protocols. Each wavelength operates within a specific absorption spectrum, targeting different chromophores such as water, hemoglobin, melanin, or bacterial pigments.
1. 450nm (Blue Laser): Precision Soft Tissue Surgery
The 450nm blue laser has emerged as a highly advanced tool in soft tissue management around implants. Its wavelength exhibits strong absorption in hemoglobin and melanin, making it exceptionally effective for **vascular soft tissue procedures**.
Clinical Characteristics
- Ultra-precise incision capability
- High affinity for hemoglobin → excellent hemostasis
- Minimal penetration depth → reduced collateral damage
- “Cold cutting” effect compared to traditional diode lasers
Applications in Peri-Implantitis
In peri-implantitis cases, the 450nm laser is particularly useful for:
- Removal of inflamed peri-implant soft tissue
- Granulation tissue excision during open flap procedures
- Soft tissue contouring around implants
Clinical Advantages
The key advantage lies in its ability to perform **atraumatic soft tissue surgery**. The minimal thermal diffusion reduces the risk of damaging surrounding bone and implant surfaces. This is critical in peri-implantitis, where preserving remaining bone is essential.
Additionally, patients benefit from:
- Reduced postoperative pain
- Minimal swelling
- Faster healing due to limited necrosis
2. 980nm (Near-Infrared Laser): Decontamination & Bacterial Reduction
The 980nm diode laser is one of the most widely used wavelengths in dentistry, particularly in periodontics and implantology. Its absorption in both water and hemoglobin allows for **deep penetration into soft tissues**, making it highly effective for bacterial reduction.
Mechanism of Action
- Photothermal effect → bacterial cell wall destruction
- Coagulation → reduces bleeding and improves visibility
- Moderate penetration → targets subgingival pathogens
Role in Peri-Implantitis Treatment
In peri-implantitis management, the 980nm laser is primarily used for:
- Disinfection of peri-implant pockets
- Reduction of anaerobic bacterial load
- Adjunctive therapy following mechanical debridement
Its ability to penetrate deeper than shorter wavelengths makes it effective in reaching bacteria located within micro-rough implant surfaces and surrounding tissues.
Additional Clinical Applications
- Activation of hydrogen peroxide-based whitening gels
- Soft tissue curettage
- Pocket sterilization in periodontal therapy
Limitations
Despite its effectiveness, excessive energy settings can lead to thermal damage to implant surfaces or surrounding bone. لذلك، precise calibration and controlled movement are essential.
3. 650nm (Red Laser): Low-Level Laser Therapy (LLLT)
The 650nm red laser operates at low power levels and is primarily used for **photobiomodulation therapy (PBMT)** rather than cutting or ablation. It plays a supportive role in peri-implantitis treatment by enhancing the body’s natural healing processes.
Biological Effects
- Stimulates mitochondrial activity → increased ATP production
- Enhances fibroblast proliferation
- Promotes collagen synthesis
- Reduces inflammatory mediators
Clinical Benefits in Peri-Implantitis
LLLT is particularly valuable in the post-treatment phase, حيث يساعد على:
- Accelerating soft tissue healing
- Reducing postoperative pain
- Minimizing inflammation
- Improving patient comfort
Use Cases
- After surgical peri-implantitis treatment
- Following laser or mechanical debridement
- Management of peri-implant mucositis
Although it does not directly eliminate bacteria, its regenerative effect significantly enhances overall treatment outcomes.
4. 2940nm Er:YAG Laser: Gold Standard for Hard Tissue & Implant Surface Decontamination
The 2940nm Er:YAG laser is widely considered one of the most effective laser systems for peri-implantitis treatment due to its **high absorption in water and hydroxyapatite**. This makes it uniquely capable of interacting with both soft and hard tissues without excessive الحرارة.
Mechanism of Action
- Micro-explosive ablation (photomechanical effect)
- Efficient removal of biofilm and calculus
- Minimal thermal penetration
Applications in Peri-Implantitis
- Implant surface decontamination
- Removal of granulation tissue
- Bone defect debridement
- Preparation for regenerative procedures
Key Advantages
The Er:YAG laser stands out because it can safely clean implant surfaces without altering their microstructure. This is critical for maintaining re-osseointegration potential.
- No carbonization or melting of titanium surface
- Effective biofilm removal from micro-rough surfaces
- Reduced need for aggressive mechanical instrumentation
Clinical Outcomes
Studies have shown that Er:YAG laser therapy can:
- Reduce probing depth
- Improve clinical attachment levels
- Enhance bone regeneration when combined with grafting
Clinical Integration Strategy
Optimal peri-implantitis management often involves a **combined laser approach**, rather than relying on a single wavelength:
- 450nm: Precise soft tissue surgery
- 980nm: Deep bacterial decontamination
- 650nm: Healing and pain modulation
- 2940nm Er:YAG: Implant surface cleaning and hard tissue management
This multimodal protocol allows clinicians to address all aspects of the disease: infection, inflammation, and tissue regeneration.
Conclusion
Laser therapy represents a paradigm shift in peri-implantitis treatment, offering minimally invasive, highly targeted, and biologically favorable outcomes. While no single wavelength can address all clinical needs, understanding the unique properties of each laser type allows clinicians to design comprehensive, evidence-based treatment protocols.
When integrated correctly, lasers not only improve decontamination efficiency but also enhance healing, reduce patient morbidity, and ultimately increase implant survival rates.
Recent Articles
Magnetically Guided Dental Nanobots (CalBots) Are Real
Magnetically Guided Dental Nanobots (CalBots) Are Real The concept of nanobots in dentistry has long been associated with futuristic speculation. However, recent peer-reviewed research [...]
Peri-Implantitis Treatment & Prevention Methods
Peri-Implantitis Treatment & Prevention Methods Peri-implantitis remains one of the most significant biological complications affecting dental implants, posing a serious threat to long-term implant [...]
Latest Sinus Lifting Techniques in Modern Implant Dentistry
Latest Sinus Lifting Techniques in Modern Implant Dentistry A Comprehensive Clinical Review Introduction to Sinus Lifting in Implantology Sinus lifting, or maxillary sinus floor [...]
Biomechanics of the Triple Abutment & BOPiT Concept
Dental Biomechanics · Implant Science · Clinical Evidence Biomechanics of the Triple Abutment & BOPiT Concept How a saddle-shaped mathematical surface is rewriting the rules of load distribution [...]
The Woman Who Proved One Implant Could Hold Three Crowns
The Woman Who Proved One Implant Could Hold Three Crowns While the dental establishment looked away, Dr. Luciana Colepícolo spent 12 years building the [...]
ENPP1, The Molecular Brake That Limits Tissue Healing
ENPP1, The Molecular Brake That Limits Tissue Healing Introduction: A New Biological Barrier to Dental Regeneration Meet ENPP1—a protein most dentists have never heard [...]