Endodontic Regeneration Therapy
The Future of Pulp and Periapical Tissue Healing
Endodontic regeneration therapy represents a paradigm shift in modern dentistry. Instead of merely removing infected pulp tissue and sealing the canal space, regenerative endodontics aims to biologically restore damaged pulp, dentin, and periapical structures. With advances in stem cell biology, tissue engineering, biomaterials, and molecular signaling, clinicians can now move beyond conventional root canal therapy toward true tissue regeneration.
This comprehensive guide explores the biological principles, clinical protocols, stem cell sources, scaffold selection, and emerging technologies shaping regenerative endodontic treatment (RET). Whether you are a clinician, researcher, or dental student, understanding the mechanisms behind pulp and bone regeneration is essential for the future of endodontic care.
What Is Endodontic Regeneration Therapy?
Endodontic regeneration therapy, or Regenerative Endodontic Therapy (RET), is a biologically based procedure designed to replace damaged pulp tissue with viable tissue capable of restoring normal function. Unlike traditional root canal treatment, which focuses on disinfection and obturation, regenerative therapy stimulates the body’s natural healing mechanisms to regenerate pulp-like tissue, dentin formation, and in some cases, continued root development.
RET is particularly valuable in immature permanent teeth with necrotic pulp, where conventional treatment may halt root development and weaken the tooth structure. Through controlled disinfection, scaffold placement, and recruitment or transplantation of stem cells, clinicians can promote tissue repair and regeneration within the root canal system.
Biological Foundation of Pulp and Bone Regeneration
Successful regeneration depends on three fundamental components of tissue engineering:
- Stem cells
- Scaffolds
- Signaling molecules (growth factors)
Dental pulp stem cells (DPSCs), stem cells from the apical papilla (SCAP), and other mesenchymal stem cells possess the ability to differentiate into odontoblast-like cells and produce dentin matrix. These cells also contribute to angiogenesis and neurogenesis, which are essential for restoring vitality.
In cases involving apical periodontitis, regenerative therapy also supports periapical bone healing. Stem cells can differentiate into osteoblast-like cells, contributing to skeletal repair and regeneration of the alveolar bone.
Clinical Indications for Regenerative Endodontic Therapy
RET is primarily indicated for:
- Immature permanent teeth with necrotic pulp
- Apical periodontitis with open apex
- Trauma-related pulp necrosis
- Cases where continued root development is desirable
Emerging research also explores its application in mature teeth, although predictable outcomes are still under investigation. The most consistent success remains in young patients with wide apical foramina that facilitate cell migration and revascularization.
Endodontic Regeneration Therapy Strategies & Solutions
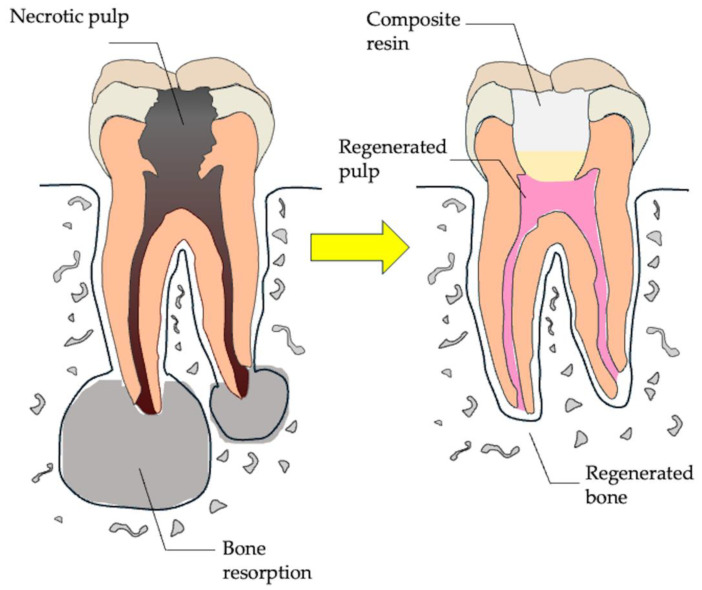
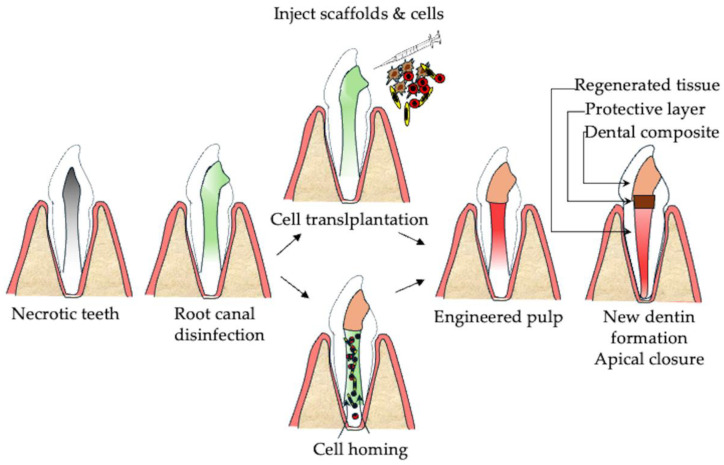
Regeneration therapy for pulpitis and apical periodontitis. Necrotic dental pulp can be treated through pulp regeneration, characterized by reconstruction of the pulpodentinal complex via angiogenesis, neurogenesis, and dentin formation, resolving bone resorption and restoring physiological tooth functions.
Current Endodontic Therapy for Promoting Pulp Wound Healing
Current endodontic therapy for promoting pulp wound healing is determined by the classification of pulpitis—reversible or irreversible—as well as the extent of pulpal inflammation and structural damage. In cases of reversible pulpitis, the pulp is inflamed but retains its healing potential. Management is based on vital pulp therapy (VPT), which aims to eliminate the irritant, control inflammation, and preserve pulp vitality. This is typically achieved through complete caries removal followed by the application of biocompatible pulp-capping materials such as calcium hydroxide or mineral trioxide aggregate (MTA) to stimulate healing of the dentin–pulp complex and encourage reparative dentin formation. In contrast, irreversible pulpitis involves extensive inflammation and permanent pulpal damage, requiring conventional root canal treatment (RCT), where the infected pulp is removed and the canal system is cleaned, disinfected, and obturated to prevent reinfection. Emerging regenerative endodontic therapy (RET) seeks to move beyond repair by aiming to restore functional pulp tissue and enable continued root maturation, particularly in young patients with immature teeth.
1- Vital Pulp Therapy
VPT encompasses procedures such as direct pulp capping, partial pulpotomy, and full pulpotomy, all designed to preserve viable pulp tissue and promote continued root development, apical closure, and dentinal wall thickening—particularly in immature permanent teeth. While advancements, especially the introduction of highly biocompatible materials like MTA, have expanded VPT indications even to certain mature permanent teeth with symptoms suggestive of irreversible pulpitis, histological evidence indicates that these approaches primarily support repair and healing rather than true biological regeneration.
Endodontic Regeneration Therapy Strategies & Solutions 2
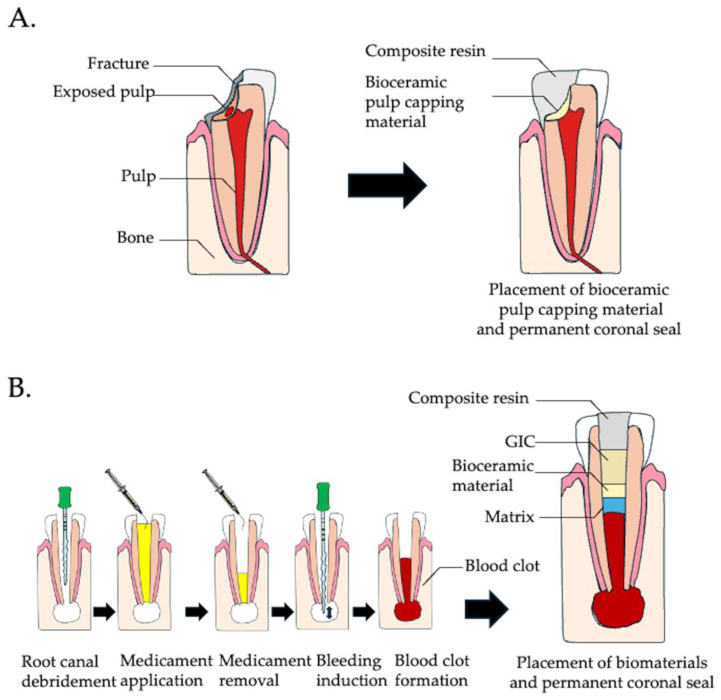
Current regeneration therapy in endodontics. (A) Vital pulp therapy: The diseased or inflamed pulp is removed, and a biocompatible pulp-capping material is applied to promote healing and protect the pulp. (B) Regenerative endodontic procedure for an immature tooth with pulp necrosis or apical periodontitis. The procedure begins with intracanal debridement followed by the application of a medicament. After the medicament is removed, a file is used to induce a blood clot within the canal, facilitating the migration of endogenous cells into the root canal. Once the blood clot is established, a permanent coronal seal is placed to protect and isolate the regenerative site.
2- Regenerative Endodontics
Regenerative endodontics focuses on restoring the structure and function of the dental pulp rather than merely repairing it. The ultimate objectives are to regenerate viable pulp tissue, re-establish sensory nerve responses, promote secondary dentin formation, and extend the long-term survival of the tooth. There are three main strategies for regenerative endodontic treatment: the cell-free approach, the cell-based approach, and the cell-homing approach. The cell-free approach, also known as revascularization, stimulates the ingrowth of vascularized tissue into the root canal system by encouraging proliferation from periapical tissues or inducing bleeding from the root apex, thereby creating a natural scaffold for tissue regeneration.
Step-by-Step Regenerative Endodontic Procedure
Although protocols vary, a standard regenerative procedure typically includes:
1. Conservative Disinfection
The root canal is gently irrigated using low-concentration sodium hypochlorite to minimize cytotoxicity to stem cells. Intracanal medicaments such as calcium hydroxide or low-dose antibiotic paste may be placed to eliminate infection while preserving stem cell viability.
2. Induction of Bleeding
After removing medicaments, bleeding is induced by over-instrumentation beyond the apex. The resulting blood clot serves as a natural scaffold rich in stem cells and growth factors.
3. Scaffold Formation
The blood clot or platelet-rich fibrin (PRF) acts as a biological scaffold. This matrix supports cell migration, proliferation, and differentiation.
4. Coronal Seal
A biocompatible material such as mineral trioxide aggregate (MTA) or bioceramic cement is placed over the scaffold to provide a hermetic seal and prevent reinfection.
Cell-Based vs. Cell-Homing Approaches
Regenerative strategies are divided into two major categories:
Cell-Based Therapy
This method involves the transplantation of ex vivo expanded stem cells into the canal space. DPSCs cultured in T-flasks (such as T-25, T-75, T-150, or T-225) are expanded to achieve sufficient cell numbers for therapeutic dosing.
Larger flasks such as T-225 provide higher cell yields suitable for clinical-scale research. However, for pilot studies or laboratory investigations, smaller flasks like T-25 or T-75 may be adequate for initial expansion phases.
Cell-Homing Therapy
This technique relies on recruiting endogenous stem cells from periapical tissues through signaling molecules and scaffold placement. It is less complex and more clinically feasible at present.
Endodontic Regeneration Therapy Strategies & Solutions 3
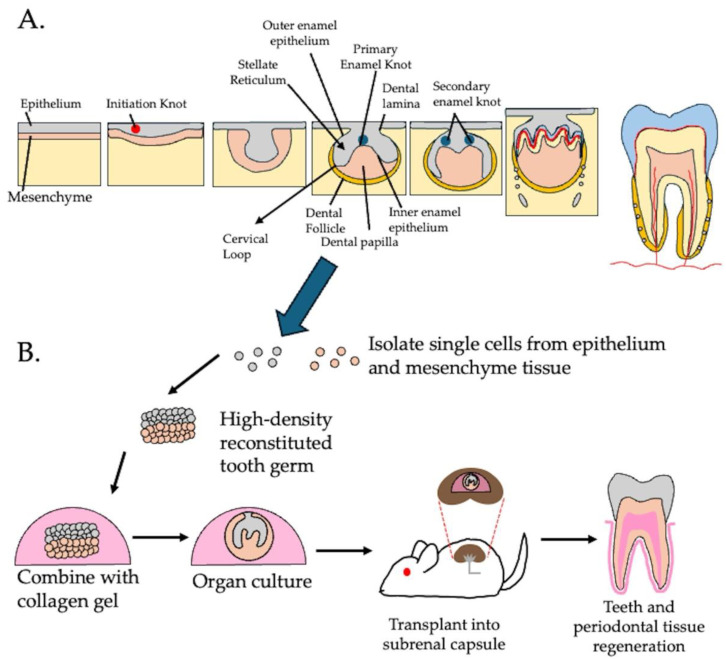
Bioengineered tooth germ technology based on tooth germ development. (A) Stages of tooth development; dental placode formation, bud stage, cap stage and bell stage. Following the bell stage, the dental follicle and enamel organ continue to develop and differentiate into a mature tooth. (B) Bioengineered tooth germ technology based on reconstruction of dental mesenchyme and dental epithelium.
Scaffold Materials in Regenerative Endodontics
Scaffolds provide structural support for stem cells and guide tissue formation. Common scaffold options include:
- Blood clot (natural scaffold)
- Platelet-rich fibrin (PRF)
- Collagen matrices
- Hydrogels
- Synthetic biodegradable polymers
Ideal scaffold materials must be biocompatible, biodegradable, and capable of delivering growth factors in a controlled manner.
Growth Factors and Molecular Signaling
Growth factors play a critical role in directing stem cell differentiation and tissue formation. Key signaling molecules include:
- Transforming growth factor beta (TGF-β)
- Bone morphogenetic proteins (BMPs)
- Vascular endothelial growth factor (VEGF)
- Platelet-derived growth factor (PDGF)
These molecules promote angiogenesis, odontoblastic differentiation, and mineralized tissue formation, which are essential for true pulp regeneration.
Endodontic Regeneration Therapy Strategies & Solutions 4
Bioengineered tooth germ technology based on tooth germ development. (A) Stages of tooth development; dental placode formation, bud stage, cap stage and bell stage. Following the bell stage, the dental follicle and enamel organ continue to develop and differentiate into a mature tooth. (B) Bioengineered tooth germ technology based on reconstruction of dental mesenchyme and dental epithelium.
Bone Regeneration in Apical Periodontitis
Regenerative endodontic therapy does not only target pulp tissue. In cases of apical periodontitis, inflammatory bone loss occurs around the root apex. Successful RET stimulates osteogenic differentiation and promotes periapical bone regeneration.
Stem cells contribute to bone matrix deposition and remodeling, restoring the integrity of the alveolar bone. Radiographic evidence often shows progressive reduction of periapical radiolucency over follow-up periods.
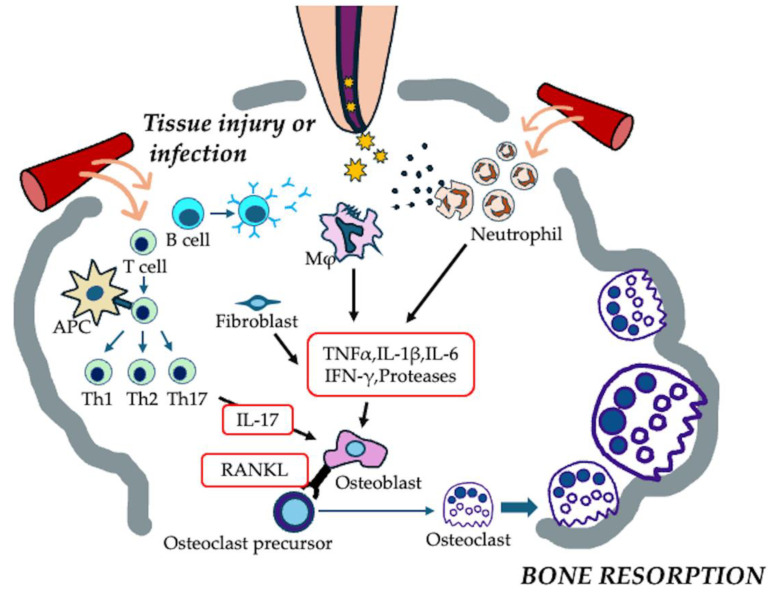
Endodontic Regeneration Therapy Strategies & Solutions 5
Pathogenesis of apical periodontitis. Microbial infection or tissue injury within the root canal system triggers an acute inflammatory response, leading to the recruitment of immune cells, primarily neutrophils, macrophages, and lymphocytes. These immune cells release pro-inflammatory cytokines, including TNF-α, IL-1β, IL-6, IL-17, and RANKL, which stimulate osteoclast formation and activation, ultimately resulting in bone resorption at the root apex.
Advantages of Regenerative Endodontics
- Continued root development in immature teeth
- Thickening of dentinal walls
- Improved fracture resistance
- Biological restoration of vitality
- Potential immune defense restoration
Compared to apexification procedures, regenerative therapy offers superior long-term structural outcomes.
Limitations and Challenges
Despite promising results, several limitations exist:
- Unpredictable tissue type formation
- Tooth discoloration risk
- Technique sensitivity
- Limited evidence in mature teeth
- Regulatory challenges for cell-based therapies
Further randomized clinical trials and long-term studies are necessary to standardize protocols and improve predictability.
Future Directions in Dental Tissue Engineering
The future of regenerative endodontics lies in advanced biomaterials, gene therapy, 3D bioprinting, and nanotechnology. Research is exploring injectable hydrogel systems containing stem cells and bioactive molecules capable of forming organized pulp-dentin complexes.
Additionally, scaffold-free cell sheets and exosome-based therapies are being investigated to enhance regenerative potential while minimizing immunogenic risks.
Conclusion
Endodontic regeneration therapy marks a transformative advancement in dentistry. By integrating stem cell biology, biomaterials science, and molecular engineering, clinicians can now aim for true biological restoration rather than mechanical repair.
Although challenges remain, the clinical success of regenerative procedures in immature necrotic teeth demonstrates the immense potential of this field. As research continues to refine protocols and materials, regenerative endodontics is expected to become a cornerstone of biologically driven dental care.
Reference:
Endodontic Regeneration Therapy: Current Strategies and Tissue Engineering Solutions
Moe Sandar Kyaw 1, Yuya Kamano 1,*, Yoshio Yahata 1, Toshinori Tanaka 1, Nobuya Sato 1, Fusami Toyama 1, Tomose Noguchi 1, Marina Saito 1, Masato Nakano 1, Futaba Harada 1, Masahiro Saito 1
All images in the article belong to the above-mentioned source.
Frequently Asked Questions (FAQ) About Endodontic Regeneration Therapy
1. Is there any commercial DPSC injection available for clinical purchase?
Currently, there is no widely approved, commercially available dental pulp stem cell (DPSC) injection product for routine clinical endodontic use. Most DPSC applications remain in the research or clinical trial phase. Regenerative endodontic procedures performed in daily practice rely primarily on cell-homing approaches rather than commercially prepared stem cell injections.
2. What is the difference between T-25, T-75, T-150, and T-225 flasks?
These designations refer to the surface area (in cm²) of cell culture flasks used for stem cell expansion. The larger the surface area, the greater the potential cell yield. T-25 is used for very small-scale expansion, T-75 for initial or small batches, T-150 for moderate expansion, and T-225 for high-yield expansion suitable for clinical-scale dosing or advanced research.
3. What is the approximate expanded cell yield for each flask type?
Based on standard laboratory expansion ranges:
- T-25: ~0.5–2 × 10⁶ cells (early-stage expansion)
- T-75: ~1–5 × 10⁶ cells (initial expansion, small batches)
- T-150: ~3–10 × 10⁶ cells (moderate expansion)
- T-225: ~10–20 × 10⁶ cells (high-yield, clinical-scale research)
4. Which flask size is best to replicate a stem cell–based regenerative study?
The optimal flask size depends on the required therapeutic cell dose. For pilot or in vitro studies, T-25 or T-75 flasks are often sufficient. However, for studies aiming to simulate clinical-scale dosing or injectable stem cell delivery models, T-150 or T-225 flasks are generally more appropriate due to their higher expansion capacity.
5. What are the key biological components required for successful endodontic regeneration?
Successful regenerative endodontic therapy depends on three essential components of tissue engineering: stem cells, scaffolds, and signaling molecules (growth factors). Stem cells such as DPSCs or SCAP provide the regenerative potential, scaffolds such as blood clot or platelet-rich fibrin offer structural support, and growth factors like TGF-β, BMPs, and VEGF guide cell differentiation and angiogenesis. The absence of any of these components can significantly reduce regenerative predictability.
6. Is regenerative endodontic therapy effective in mature permanent teeth?
Regenerative endodontic therapy has shown the most predictable success in immature permanent teeth with open apices, where stem cell migration and revascularization are more favorable. In mature teeth with closed apices, outcomes are less consistent due to limited blood supply and reduced stem cell recruitment. While ongoing research explores protocol modifications to improve success rates in mature teeth, current evidence supports its primary indication in immature necrotic cases.
Recent Articles
Endodontic regeneration therapy represents a paradigm shift in modern dentistry. Instead of merely removing infected pulp tissue and sealing the canal space, regenerative endodontics aims to biologically restore damaged pulp, dentin, and periapical structures. With advances in stem cell biology, tissue engineering, biomaterials, and molecular signaling, clinicians can now move beyond conventional root canal therapy toward true tissue regeneration.
This comprehensive guide explores the biological principles, clinical protocols, stem cell sources, scaffold selection, and emerging technologies shaping regenerative endodontic treatment (RET). Whether you are a clinician, researcher, or dental student, understanding the mechanisms behind pulp and bone regeneration is essential for the future of endodontic care.
What Is Endodontic Regeneration Therapy?
Endodontic regeneration therapy, or Regenerative Endodontic Therapy (RET), is a biologically based procedure designed to replace damaged pulp tissue with viable tissue capable of restoring normal function. Unlike traditional root canal treatment, which focuses on disinfection and obturation, regenerative therapy stimulates the body’s natural healing mechanisms to regenerate pulp-like tissue, dentin formation, and in some cases, continued root development.
RET is particularly valuable in immature permanent teeth with necrotic pulp, where conventional treatment may halt root development and weaken the tooth structure. Through controlled disinfection, scaffold placement, and recruitment or transplantation of stem cells, clinicians can promote tissue repair and regeneration within the root canal system.
Biological Foundation of Pulp and Bone Regeneration
Successful regeneration depends on three fundamental components of tissue engineering:
- Stem cells
- Scaffolds
- Signaling molecules (growth factors)
Dental pulp stem cells (DPSCs), stem cells from the apical papilla (SCAP), and other mesenchymal stem cells possess the ability to differentiate into odontoblast-like cells and produce dentin matrix. These cells also contribute to angiogenesis and neurogenesis, which are essential for restoring vitality.
In cases involving apical periodontitis, regenerative therapy also supports periapical bone healing. Stem cells can differentiate into osteoblast-like cells, contributing to skeletal repair and regeneration of the alveolar bone.
Clinical Indications for Regenerative Endodontic Therapy
RET is primarily indicated for:
- Immature permanent teeth with necrotic pulp
- Apical periodontitis with open apex
- Trauma-related pulp necrosis
- Cases where continued root development is desirable
Emerging research also explores its application in mature teeth, although predictable outcomes are still under investigation. The most consistent success remains in young patients with wide apical foramina that facilitate cell migration and revascularization.

Endodontic Regeneration Therapy Strategies & Solutions
Regeneration therapy for pulpitis and apical periodontitis. Necrotic dental pulp can be treated through pulp regeneration, characterized by reconstruction of the pulpodentinal complex via angiogenesis, neurogenesis, and dentin formation, resolving bone resorption and restoring physiological tooth functions.
Current Endodontic Therapy for Promoting Pulp Wound Healing
Current endodontic therapy for promoting pulp wound healing is determined by the classification of pulpitis—reversible or irreversible—as well as the extent of pulpal inflammation and structural damage. In cases of reversible pulpitis, the pulp is inflamed but retains its healing potential. Management is based on vital pulp therapy (VPT), which aims to eliminate the irritant, control inflammation, and preserve pulp vitality. This is typically achieved through complete caries removal followed by the application of biocompatible pulp-capping materials such as calcium hydroxide or mineral trioxide aggregate (MTA) to stimulate healing of the dentin–pulp complex and encourage reparative dentin formation. In contrast, irreversible pulpitis involves extensive inflammation and permanent pulpal damage, requiring conventional root canal treatment (RCT), where the infected pulp is removed and the canal system is cleaned, disinfected, and obturated to prevent reinfection. Emerging regenerative endodontic therapy (RET) seeks to move beyond repair by aiming to restore functional pulp tissue and enable continued root maturation, particularly in young patients with immature teeth.
1- Vital Pulp Therapy
VPT encompasses procedures such as direct pulp capping, partial pulpotomy, and full pulpotomy, all designed to preserve viable pulp tissue and promote continued root development, apical closure, and dentinal wall thickening—particularly in immature permanent teeth. While advancements, especially the introduction of highly biocompatible materials like MTA, have expanded VPT indications even to certain mature permanent teeth with symptoms suggestive of irreversible pulpitis, histological evidence indicates that these approaches primarily support repair and healing rather than true biological regeneration.

Endodontic Regeneration Therapy Strategies & Solutions 2
Current regeneration therapy in endodontics. (A) Vital pulp therapy: The diseased or inflamed pulp is removed, and a biocompatible pulp-capping material is applied to promote healing and protect the pulp. (B) Regenerative endodontic procedure for an immature tooth with pulp necrosis or apical periodontitis. The procedure begins with intracanal debridement followed by the application of a medicament. After the medicament is removed, a file is used to induce a blood clot within the canal, facilitating the migration of endogenous cells into the root canal. Once the blood clot is established, a permanent coronal seal is placed to protect and isolate the regenerative site.
2- Regenerative Endodontics
Regenerative endodontics focuses on restoring the structure and function of the dental pulp rather than merely repairing it. The ultimate objectives are to regenerate viable pulp tissue, re-establish sensory nerve responses, promote secondary dentin formation, and extend the long-term survival of the tooth. There are three main strategies for regenerative endodontic treatment: the cell-free approach, the cell-based approach, and the cell-homing approach. The cell-free approach, also known as revascularization, stimulates the ingrowth of vascularized tissue into the root canal system by encouraging proliferation from periapical tissues or inducing bleeding from the root apex, thereby creating a natural scaffold for tissue regeneration.
Step-by-Step Regenerative Endodontic Procedure
Although protocols vary, a standard regenerative procedure typically includes:
1. Conservative Disinfection
The root canal is gently irrigated using low-concentration sodium hypochlorite to minimize cytotoxicity to stem cells. Intracanal medicaments such as calcium hydroxide or low-dose antibiotic paste may be placed to eliminate infection while preserving stem cell viability.
2. Induction of Bleeding
After removing medicaments, bleeding is induced by over-instrumentation beyond the apex. The resulting blood clot serves as a natural scaffold rich in stem cells and growth factors.
3. Scaffold Formation
The blood clot or platelet-rich fibrin (PRF) acts as a biological scaffold. This matrix supports cell migration, proliferation, and differentiation.
4. Coronal Seal
A biocompatible material such as mineral trioxide aggregate (MTA) or bioceramic cement is placed over the scaffold to provide a hermetic seal and prevent reinfection.
Cell-Based vs. Cell-Homing Approaches
Regenerative strategies are divided into two major categories:
Cell-Based Therapy
This method involves the transplantation of ex vivo expanded stem cells into the canal space. DPSCs cultured in T-flasks (such as T-25, T-75, T-150, or T-225) are expanded to achieve sufficient cell numbers for therapeutic dosing.
Larger flasks such as T-225 provide higher cell yields suitable for clinical-scale research. However, for pilot studies or laboratory investigations, smaller flasks like T-25 or T-75 may be adequate for initial expansion phases.
Cell-Homing Therapy
This technique relies on recruiting endogenous stem cells from periapical tissues through signaling molecules and scaffold placement. It is less complex and more clinically feasible at present.

Endodontic Regeneration Therapy Strategies & Solutions 3
Bioengineered tooth germ technology based on tooth germ development. (A) Stages of tooth development; dental placode formation, bud stage, cap stage and bell stage. Following the bell stage, the dental follicle and enamel organ continue to develop and differentiate into a mature tooth. (B) Bioengineered tooth germ technology based on reconstruction of dental mesenchyme and dental epithelium.
Scaffold Materials in Regenerative Endodontics
Scaffolds provide structural support for stem cells and guide tissue formation. Common scaffold options include:
- Blood clot (natural scaffold)
- Platelet-rich fibrin (PRF)
- Collagen matrices
- Hydrogels
- Synthetic biodegradable polymers
Ideal scaffold materials must be biocompatible, biodegradable, and capable of delivering growth factors in a controlled manner.
Growth Factors and Molecular Signaling
Growth factors play a critical role in directing stem cell differentiation and tissue formation. Key signaling molecules include:
- Transforming growth factor beta (TGF-β)
- Bone morphogenetic proteins (BMPs)
- Vascular endothelial growth factor (VEGF)
- Platelet-derived growth factor (PDGF)
These molecules promote angiogenesis, odontoblastic differentiation, and mineralized tissue formation, which are essential for true pulp regeneration.

Endodontic Regeneration Therapy Strategies & Solutions 4
Bioengineered tooth germ technology based on tooth germ development. (A) Stages of tooth development; dental placode formation, bud stage, cap stage and bell stage. Following the bell stage, the dental follicle and enamel organ continue to develop and differentiate into a mature tooth. (B) Bioengineered tooth germ technology based on reconstruction of dental mesenchyme and dental epithelium.
Bone Regeneration in Apical Periodontitis
Regenerative endodontic therapy does not only target pulp tissue. In cases of apical periodontitis, inflammatory bone loss occurs around the root apex. Successful RET stimulates osteogenic differentiation and promotes periapical bone regeneration.
Stem cells contribute to bone matrix deposition and remodeling, restoring the integrity of the alveolar bone. Radiographic evidence often shows progressive reduction of periapical radiolucency over follow-up periods.

Endodontic Regeneration Therapy Strategies & Solutions 5
Pathogenesis of apical periodontitis. Microbial infection or tissue injury within the root canal system triggers an acute inflammatory response, leading to the recruitment of immune cells, primarily neutrophils, macrophages, and lymphocytes. These immune cells release pro-inflammatory cytokines, including TNF-α, IL-1β, IL-6, IL-17, and RANKL, which stimulate osteoclast formation and activation, ultimately resulting in bone resorption at the root apex.
Advantages of Regenerative Endodontics
- Continued root development in immature teeth
- Thickening of dentinal walls
- Improved fracture resistance
- Biological restoration of vitality
- Potential immune defense restoration
Compared to apexification procedures, regenerative therapy offers superior long-term structural outcomes.
Limitations and Challenges
Despite promising results, several limitations exist:
- Unpredictable tissue type formation
- Tooth discoloration risk
- Technique sensitivity
- Limited evidence in mature teeth
- Regulatory challenges for cell-based therapies
Further randomized clinical trials and long-term studies are necessary to standardize protocols and improve predictability.
Future Directions in Dental Tissue Engineering
The future of regenerative endodontics lies in advanced biomaterials, gene therapy, 3D bioprinting, and nanotechnology. Research is exploring injectable hydrogel systems containing stem cells and bioactive molecules capable of forming organized pulp-dentin complexes.
Additionally, scaffold-free cell sheets and exosome-based therapies are being investigated to enhance regenerative potential while minimizing immunogenic risks.
Conclusion
Endodontic regeneration therapy marks a transformative advancement in dentistry. By integrating stem cell biology, biomaterials science, and molecular engineering, clinicians can now aim for true biological restoration rather than mechanical repair.
Although challenges remain, the clinical success of regenerative procedures in immature necrotic teeth demonstrates the immense potential of this field. As research continues to refine protocols and materials, regenerative endodontics is expected to become a cornerstone of biologically driven dental care.
Reference:
Endodontic Regeneration Therapy: Current Strategies and Tissue Engineering Solutions
Moe Sandar Kyaw 1, Yuya Kamano 1,*, Yoshio Yahata 1, Toshinori Tanaka 1, Nobuya Sato 1, Fusami Toyama 1, Tomose Noguchi 1, Marina Saito 1, Masato Nakano 1, Futaba Harada 1, Masahiro Saito 1
All images in the article belong to the above-mentioned source.
Frequently Asked Questions (FAQ) About Endodontic Regeneration Therapy
1. Is there any commercial DPSC injection available for clinical purchase?
Currently, there is no widely approved, commercially available dental pulp stem cell (DPSC) injection product for routine clinical endodontic use. Most DPSC applications remain in the research or clinical trial phase. Regenerative endodontic procedures performed in daily practice rely primarily on cell-homing approaches rather than commercially prepared stem cell injections.
2. What is the difference between T-25, T-75, T-150, and T-225 flasks?
These designations refer to the surface area (in cm²) of cell culture flasks used for stem cell expansion. The larger the surface area, the greater the potential cell yield. T-25 is used for very small-scale expansion, T-75 for initial or small batches, T-150 for moderate expansion, and T-225 for high-yield expansion suitable for clinical-scale dosing or advanced research.
3. What is the approximate expanded cell yield for each flask type?
Based on standard laboratory expansion ranges:
- T-25: ~0.5–2 × 10⁶ cells (early-stage expansion)
- T-75: ~1–5 × 10⁶ cells (initial expansion, small batches)
- T-150: ~3–10 × 10⁶ cells (moderate expansion)
- T-225: ~10–20 × 10⁶ cells (high-yield, clinical-scale research)
4. Which flask size is best to replicate a stem cell–based regenerative study?
The optimal flask size depends on the required therapeutic cell dose. For pilot or in vitro studies, T-25 or T-75 flasks are often sufficient. However, for studies aiming to simulate clinical-scale dosing or injectable stem cell delivery models, T-150 or T-225 flasks are generally more appropriate due to their higher expansion capacity.
5. What are the key biological components required for successful endodontic regeneration?
Successful regenerative endodontic therapy depends on three essential components of tissue engineering: stem cells, scaffolds, and signaling molecules (growth factors). Stem cells such as DPSCs or SCAP provide the regenerative potential, scaffolds such as blood clot or platelet-rich fibrin offer structural support, and growth factors like TGF-β, BMPs, and VEGF guide cell differentiation and angiogenesis. The absence of any of these components can significantly reduce regenerative predictability.
6. Is regenerative endodontic therapy effective in mature permanent teeth?
Regenerative endodontic therapy has shown the most predictable success in immature permanent teeth with open apices, where stem cell migration and revascularization are more favorable. In mature teeth with closed apices, outcomes are less consistent due to limited blood supply and reduced stem cell recruitment. While ongoing research explores protocol modifications to improve success rates in mature teeth, current evidence supports its primary indication in immature necrotic cases.