Enamel Demineralization in Orthodontic Treatment
Enamel demineralization in orthodontic treatment is a well-documented clinical complication characterized by mineral loss from the enamel surface, frequently presenting as white spot lesions (WSL). These opaque, chalky areas represent the earliest visible stage of dental caries and can compromise both oral health and post-treatment aesthetics. Given that comprehensive orthodontic therapy often spans 2–3 years—or longer in complex cases—the cumulative risk of enamel demineralization increases significantly without structured prevention and monitoring.
This article provides a clinically grounded overview of enamel demineralization in orthodontic treatment, including etiology, diagnosis, risk assessment, prevention strategies, and contemporary management approaches.
Understanding Enamel Demineralization in Orthodontic Treatment
Enamel demineralization occurs when the balance between mineral loss and mineral gain at the tooth surface is disrupted. Around orthodontic brackets, bands, and archwires, plaque retention increases due to irregular surfaces that hinder effective oral hygiene. Acidogenic bacteria—particularly Streptococcus mutans—metabolize fermentable carbohydrates, producing acids that lower plaque pH below the critical threshold (~5.5). This acidic environment dissolves hydroxyapatite crystals within enamel.
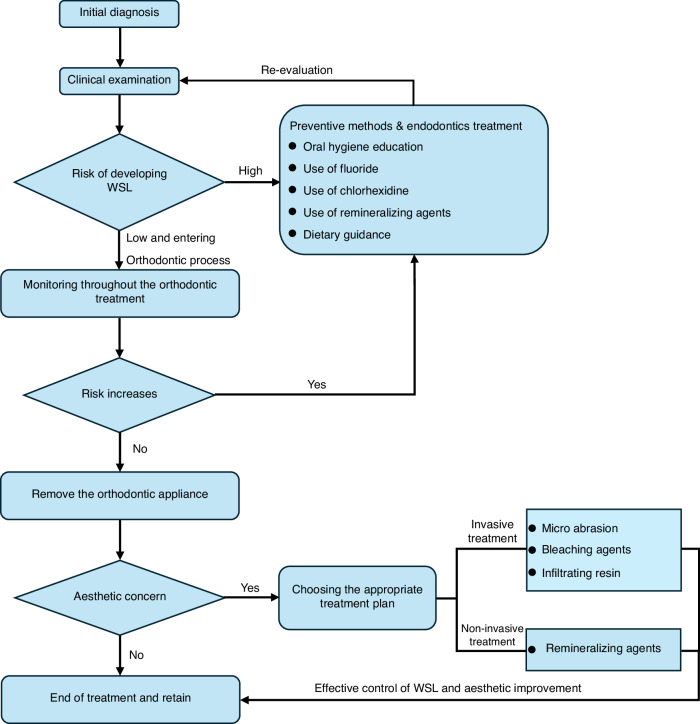
Mineral loss typically occurs beneath a relatively intact surface layer, increasing enamel porosity. As light refracts differently through porous enamel, a chalky white appearance develops—clinically recognized as white spot lesions. When left unmanaged, surface collapse may occur, progressing to cavitated caries, pulp involvement, and even tooth loss.
Prevalence rates of WSL during orthodontic therapy range from 23% to over 70%, depending on detection methods. Patients treated with clear aligners generally exhibit lower incidence compared to those with fixed appliances, although lesion morphology differs. Fixed appliances tend to produce smaller but deeper lesions, whereas aligners may result in larger yet shallower demineralized areas.
Etiology and Risk Factors
Multiple biological and behavioral variables influence the development of enamel demineralization during orthodontic treatment:
- Poor baseline oral hygiene
- Deterioration of hygiene during treatment
- Preexisting white spot lesions
- Extended orthodontic duration (>36 months)
- High-frequency carbohydrate consumption
- Reduced salivary flow
- Systemic conditions such as diabetes or Sjögren’s syndrome
Among these, the most significant predictor is the presence of preexisting WSL before orthodontic appliance placement. The orthodontic environment exacerbates plaque accumulation and shifts the oral microbiome toward acidogenic species, intensifying mineral dissolution.
Diagnosis of Enamel Demineralization in Orthodontic Treatment
Early and accurate detection is essential to prevent lesion progression. The International Caries Detection and Assessment System (ICDAS) recognizes visual inspection and tactile assessment as foundational diagnostic methods. However, adjunctive technologies enhance sensitivity and documentation.
1. Visual and Probing Examination
The enamel surface must be cleaned and dried for at least 5 seconds. Active lesions appear matte and rough, whereas inactive lesions appear smooth and glossy. Probing assesses surface texture but should be gentle to avoid structural damage.
2. Digital Photography
High-resolution macro photography allows longitudinal documentation and grayscale analysis of lesion severity. It improves interdisciplinary consultation among orthodontists, restorative dentists, and preventive specialists.
3. Fluorescence-Based Systems
Devices such as KaVo’s DIAGNOdent use laser fluorescence to quantify mineral loss. Quantitative Light-Induced Fluorescence (QLF) assesses lesion size and density. While useful as adjunctive tools, fluorescence methods are not yet considered the gold standard due to false positives from stains or restorations.
4. Fiber-Optic and Near-Infrared Transillumination
Demineralized enamel scatters light differently from sound enamel. Near-infrared transillumination enhances contrast and detects subsurface lesions with high sensitivity.
5. Artificial Intelligence Integration
Deep learning models, particularly convolutional neural networks (CNNs), have demonstrated up to 95% diagnostic accuracy in caries detection from digital images. AI systems show promise for chairside lesion monitoring, although they remain supplementary to clinical judgment.
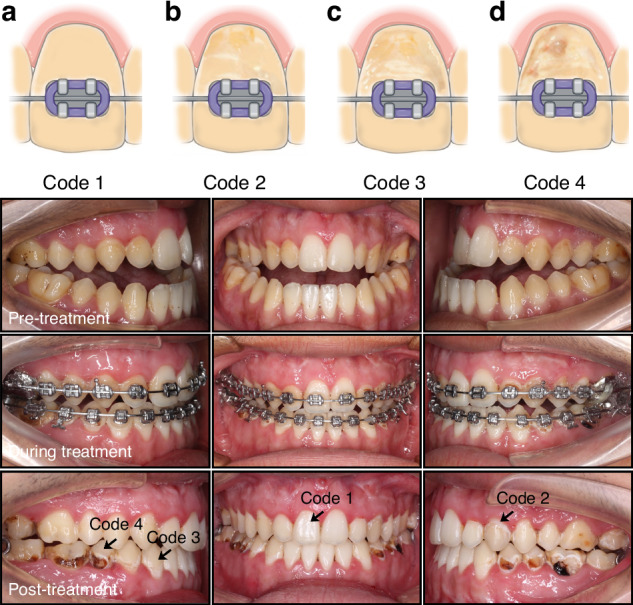
Risk Assessment Before Orthodontic Treatment
Comprehensive risk evaluation should precede appliance placement. This assessment includes:
- Past caries history
- Oral hygiene status
- Dietary patterns
- Fluoride exposure
- Salivary function
- Systemic health factors
Patients identified as high risk require preventive intervention before initiating orthodontic therapy. Treatment should only proceed once demineralization risk is adequately controlled.
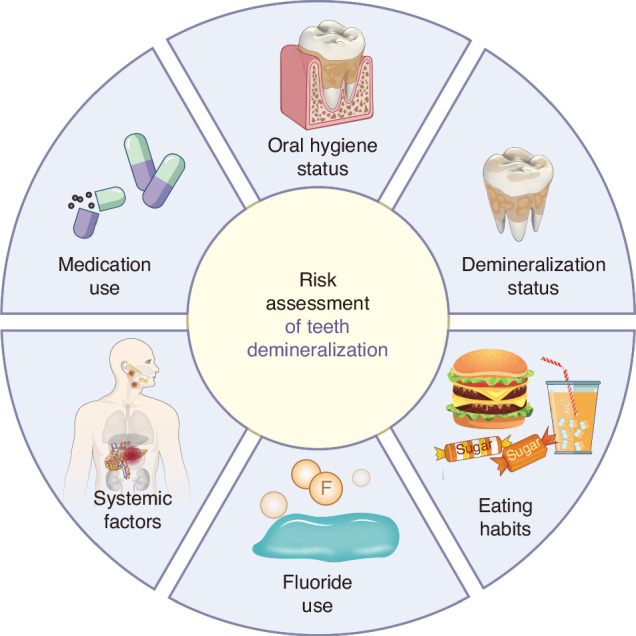
Preventive Strategies for Enamel Demineralization in Orthodontic Treatment
Prevention remains the most predictable strategy in managing enamel demineralization in orthodontic treatment. A structured preventive protocol includes behavioral, chemical, and mechanical interventions.
Oral Hygiene Education
Patients must brush at least three times daily using proper orthodontic brushing techniques. Interdental brushes and orthodontic floss threaders are essential for plaque control around brackets.
Fluoride Therapy
Fluoride remains the cornerstone of demineralization prevention. Its mechanisms include:
- Formation of fluorapatite (lower solubility than hydroxyapatite)
- Promotion of remineralization
- Inhibition of bacterial metabolism
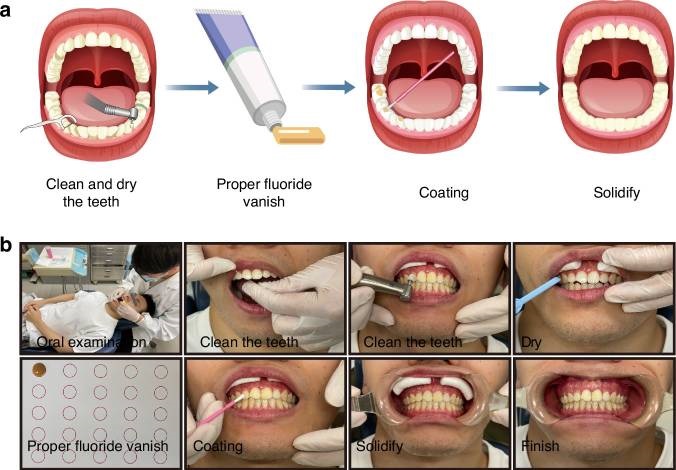
The American Academy of Pediatric Dentistry recommends 5% fluoride varnish (22,600 ppm) at least twice yearly for children and more frequently in high-risk cases.
Topical fluoride applications prolong enamel exposure and significantly reduce WSL incidence when used consistently during orthodontic care.
Remineralizing Agents (CPP-ACP)
Casein phosphopeptide–amorphous calcium phosphate stabilizes calcium and phosphate ions in a bioavailable form, facilitating subsurface remineralization. When combined with fluoride, synergistic mineral deposition occurs.
Chlorhexidine Varnish
Chlorhexidine reduces Streptococcus mutans levels and biofilm formation. Varnish formulations provide sustained antimicrobial effects, although staining and taste alteration may occur.
Dietary Modification
Reducing intake of sticky, sugary, and acidic foods minimizes acid challenges. Patients should avoid consuming fermentable carbohydrates while wearing aligners and maintain oral cleansing before reinsertion.
Management of Active White Spot Lesions
When enamel demineralization develops despite preventive efforts, management depends on lesion severity.
1. Non-Invasive Remineralization
For early lesions (Gorelick score ≤3):
- Fluoride varnish
- CPP-ACP applications
- Antibiofilm biomaterials under investigation
- Laser-assisted enamel modification (CO₂ and Er:YAG lasers show promising acid-resistance enhancement)
2. Resin Infiltration
Low-viscosity resin infiltrates porous enamel via capillary action, sealing microporosities and improving refractive index matching. This approach halts progression and significantly improves aesthetics without substantial enamel removal.
3. Microabrasion
A controlled mixture of acid and abrasive slurry removes superficial enamel irregularities. Effective for shallow lesions but involves minimal enamel loss.
4. Bleaching
Whitening agents may camouflage WSL but do not restore mineral content. Clinical evidence for long-term benefit remains limited.
5. Veneers (Severe Cases)
For advanced structural defects, minimally invasive ceramic veneers restore aesthetics. However, this approach involves irreversible enamel reduction and should be reserved for refractory cases.
Special Considerations in Pediatric and Adolescent Orthodontics
Children and adolescents present an elevated risk due to incomplete enamel maturation and inconsistent hygiene compliance. Parental education is critical. Preventive strategies should include:
- Fluoridated toothpaste
- Pit and fissure sealants
- Routine plaque disclosure
- Close monitoring at follow-up visits
If lesion progression becomes uncontrollable, appliance modification or temporary treatment suspension may be necessary.
Future Perspectives in Enamel Demineralization Management
Emerging research focuses on biomimetic remineralization technologies that simulate natural enamel mineralization pathways. Polymer-based delivery systems aim to stabilize amorphous calcium phosphate and promote hydroxyapatite crystal growth within lesion bodies.
AI-driven monitoring systems may soon enable personalized prediction of lesion progression, integrating clinical data, imaging, and risk profiles to optimize preventive timing.
Nonetheless, technology supplements—but does not replace—clinical expertise. Orthodontists must maintain vigilance in early detection and proactive intervention.
Conclusion
Enamel demineralization in orthodontic treatment represents a dynamic interplay between pathological demineralization and protective remineralization processes. White spot lesions are not merely cosmetic concerns—they are early indicators of caries progression.
Effective management requires:
- Pre-treatment risk assessment
- Continuous monitoring during orthodontic therapy
- Emphasis on prevention over restoration
- Conservative intervention before irreversible damage occurs
By integrating preventive dentistry principles into orthodontic care, clinicians can preserve enamel integrity, enhance aesthetic outcomes, and improve overall patient satisfaction following appliance removal.
In contemporary orthodontics, success is measured not only by alignment but by the preservation of healthy, intact enamel.
Reference:
Expert consensus on the prevention and treatment of enamel demineralization in orthodontic treatment
PMCID: PMC11871012 PMID: 40021614
Recent Articles
Enamel demineralization in orthodontic treatment is a well-documented clinical complication characterized by mineral loss from the enamel surface, frequently presenting as white spot lesions (WSL). These opaque, chalky areas represent the earliest visible stage of dental caries and can compromise both oral health and post-treatment aesthetics. Given that comprehensive orthodontic therapy often spans 2–3 years—or longer in complex cases—the cumulative risk of enamel demineralization increases significantly without structured prevention and monitoring.
This article provides a clinically grounded overview of enamel demineralization in orthodontic treatment, including etiology, diagnosis, risk assessment, prevention strategies, and contemporary management approaches.
Understanding Enamel Demineralization in Orthodontic Treatment
Enamel demineralization occurs when the balance between mineral loss and mineral gain at the tooth surface is disrupted. Around orthodontic brackets, bands, and archwires, plaque retention increases due to irregular surfaces that hinder effective oral hygiene. Acidogenic bacteria—particularly Streptococcus mutans—metabolize fermentable carbohydrates, producing acids that lower plaque pH below the critical threshold (~5.5). This acidic environment dissolves hydroxyapatite crystals within enamel.
Mineral loss typically occurs beneath a relatively intact surface layer, increasing enamel porosity. As light refracts differently through porous enamel, a chalky white appearance develops—clinically recognized as white spot lesions. When left unmanaged, surface collapse may occur, progressing to cavitated caries, pulp involvement, and even tooth loss.
Prevalence rates of WSL during orthodontic therapy range from 23% to over 70%, depending on detection methods. Patients treated with clear aligners generally exhibit lower incidence compared to those with fixed appliances, although lesion morphology differs. Fixed appliances tend to produce smaller but deeper lesions, whereas aligners may result in larger yet shallower demineralized areas.
Etiology and Risk Factors
Multiple biological and behavioral variables influence the development of enamel demineralization during orthodontic treatment:
- Poor baseline oral hygiene
- Deterioration of hygiene during treatment
- Preexisting white spot lesions
- Extended orthodontic duration (>36 months)
- High-frequency carbohydrate consumption
- Reduced salivary flow
- Systemic conditions such as diabetes or Sjögren’s syndrome
Among these, the most significant predictor is the presence of preexisting WSL before orthodontic appliance placement. The orthodontic environment exacerbates plaque accumulation and shifts the oral microbiome toward acidogenic species, intensifying mineral dissolution.

Diagnosis of Enamel Demineralization in Orthodontic Treatment
Early and accurate detection is essential to prevent lesion progression. The International Caries Detection and Assessment System (ICDAS) recognizes visual inspection and tactile assessment as foundational diagnostic methods. However, adjunctive technologies enhance sensitivity and documentation.
1. Visual and Probing Examination
The enamel surface must be cleaned and dried for at least 5 seconds. Active lesions appear matte and rough, whereas inactive lesions appear smooth and glossy. Probing assesses surface texture but should be gentle to avoid structural damage.
2. Digital Photography
High-resolution macro photography allows longitudinal documentation and grayscale analysis of lesion severity. It improves interdisciplinary consultation among orthodontists, restorative dentists, and preventive specialists.
3. Fluorescence-Based Systems
Devices such as KaVo’s DIAGNOdent use laser fluorescence to quantify mineral loss. Quantitative Light-Induced Fluorescence (QLF) assesses lesion size and density. While useful as adjunctive tools, fluorescence methods are not yet considered the gold standard due to false positives from stains or restorations.
4. Fiber-Optic and Near-Infrared Transillumination
Demineralized enamel scatters light differently from sound enamel. Near-infrared transillumination enhances contrast and detects subsurface lesions with high sensitivity.
5. Artificial Intelligence Integration
Deep learning models, particularly convolutional neural networks (CNNs), have demonstrated up to 95% diagnostic accuracy in caries detection from digital images. AI systems show promise for chairside lesion monitoring, although they remain supplementary to clinical judgment.

Risk Assessment Before Orthodontic Treatment
Comprehensive risk evaluation should precede appliance placement. This assessment includes:
- Past caries history
- Oral hygiene status
- Dietary patterns
- Fluoride exposure
- Salivary function
- Systemic health factors
Patients identified as high risk require preventive intervention before initiating orthodontic therapy. Treatment should only proceed once demineralization risk is adequately controlled.

Preventive Strategies for Enamel Demineralization in Orthodontic Treatment
Prevention remains the most predictable strategy in managing enamel demineralization in orthodontic treatment. A structured preventive protocol includes behavioral, chemical, and mechanical interventions.
Oral Hygiene Education
Patients must brush at least three times daily using proper orthodontic brushing techniques. Interdental brushes and orthodontic floss threaders are essential for plaque control around brackets.
Fluoride Therapy
Fluoride remains the cornerstone of demineralization prevention. Its mechanisms include:
- Formation of fluorapatite (lower solubility than hydroxyapatite)
- Promotion of remineralization
- Inhibition of bacterial metabolism
The American Academy of Pediatric Dentistry recommends 5% fluoride varnish (22,600 ppm) at least twice yearly for children and more frequently in high-risk cases.
Topical fluoride applications prolong enamel exposure and significantly reduce WSL incidence when used consistently during orthodontic care.

Remineralizing Agents (CPP-ACP)
Casein phosphopeptide–amorphous calcium phosphate stabilizes calcium and phosphate ions in a bioavailable form, facilitating subsurface remineralization. When combined with fluoride, synergistic mineral deposition occurs.
Chlorhexidine Varnish
Chlorhexidine reduces Streptococcus mutans levels and biofilm formation. Varnish formulations provide sustained antimicrobial effects, although staining and taste alteration may occur.
Dietary Modification
Reducing intake of sticky, sugary, and acidic foods minimizes acid challenges. Patients should avoid consuming fermentable carbohydrates while wearing aligners and maintain oral cleansing before reinsertion.
Management of Active White Spot Lesions
When enamel demineralization develops despite preventive efforts, management depends on lesion severity.
1. Non-Invasive Remineralization
For early lesions (Gorelick score ≤3):
- Fluoride varnish
- CPP-ACP applications
- Antibiofilm biomaterials under investigation
- Laser-assisted enamel modification (CO₂ and Er:YAG lasers show promising acid-resistance enhancement)
2. Resin Infiltration
Low-viscosity resin infiltrates porous enamel via capillary action, sealing microporosities and improving refractive index matching. This approach halts progression and significantly improves aesthetics without substantial enamel removal.
3. Microabrasion
A controlled mixture of acid and abrasive slurry removes superficial enamel irregularities. Effective for shallow lesions but involves minimal enamel loss.
4. Bleaching
Whitening agents may camouflage WSL but do not restore mineral content. Clinical evidence for long-term benefit remains limited.
5. Veneers (Severe Cases)
For advanced structural defects, minimally invasive ceramic veneers restore aesthetics. However, this approach involves irreversible enamel reduction and should be reserved for refractory cases.
Special Considerations in Pediatric and Adolescent Orthodontics
Children and adolescents present an elevated risk due to incomplete enamel maturation and inconsistent hygiene compliance. Parental education is critical. Preventive strategies should include:
- Fluoridated toothpaste
- Pit and fissure sealants
- Routine plaque disclosure
- Close monitoring at follow-up visits
If lesion progression becomes uncontrollable, appliance modification or temporary treatment suspension may be necessary.
Future Perspectives in Enamel Demineralization Management
Emerging research focuses on biomimetic remineralization technologies that simulate natural enamel mineralization pathways. Polymer-based delivery systems aim to stabilize amorphous calcium phosphate and promote hydroxyapatite crystal growth within lesion bodies.
AI-driven monitoring systems may soon enable personalized prediction of lesion progression, integrating clinical data, imaging, and risk profiles to optimize preventive timing.
Nonetheless, technology supplements—but does not replace—clinical expertise. Orthodontists must maintain vigilance in early detection and proactive intervention.
Conclusion
Enamel demineralization in orthodontic treatment represents a dynamic interplay between pathological demineralization and protective remineralization processes. White spot lesions are not merely cosmetic concerns—they are early indicators of caries progression.
Effective management requires:
- Pre-treatment risk assessment
- Continuous monitoring during orthodontic therapy
- Emphasis on prevention over restoration
- Conservative intervention before irreversible damage occurs
By integrating preventive dentistry principles into orthodontic care, clinicians can preserve enamel integrity, enhance aesthetic outcomes, and improve overall patient satisfaction following appliance removal.
In contemporary orthodontics, success is measured not only by alignment but by the preservation of healthy, intact enamel.
Reference:
Expert consensus on the prevention and treatment of enamel demineralization in orthodontic treatment
PMCID: PMC11871012 PMID: 40021614