USAG-1 and Regenerative Dentistry
Molecular Mechanisms, Clinical Trials, and the Future of Tooth Regeneration
Keywords: USAG-1, SOSTDC1, regenerative dentistry, tooth regeneration therapy, BMP signaling, Wnt signaling pathway, congenital tooth agenesis, monoclonal antibody, third dentition, dental stem cells
Introduction: A Paradigm Shift in Regenerative Dentistry
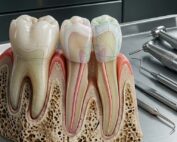
Tooth loss remains one of the most prevalent global health problems. Despite advances in implantology, biomaterials, and prosthodontics, modern dentistry still relies primarily on replacement rather than true biological regeneration. The discovery of Uterine Sensitization-Associated Gene-1 (USAG-1)—also known as SOSTDC1—has redefined the scientific landscape of regenerative dentistry by introducing the possibility of authentic tooth regrowth.
USAG-1 is a dual antagonist of the Bone Morphogenetic Protein (BMP) and Wnt signaling pathways, two master regulators of odontogenesis. By modulating these pathways, USAG1 governs dental morphogenesis, stem cell differentiation, enamel and dentin formation, and epithelial-mesenchymal interactions. Inhibiting USAG1 has demonstrated the capacity to reactivate dormant developmental programs, enabling the formation of supernumerary teeth and functional third dentition in preclinical models.
With monoclonal antibody therapies targeting USAG 1 already entering human clinical trials, regenerative dentistry is transitioning from theoretical biology to translational therapeutics.
Molecular Biology of USAG-1: Central Regulator of BMP and Wnt Signaling
USAG-1 as a Dual Pathway Antagonist
USAG 1 exerts regulatory control over two critical developmental cascades:
BMP signaling pathway
Canonical Wnt/β-catenin signaling pathway
These pathways are indispensable for:
Dental lamina formation
Tooth bud initiation
Odontoblast differentiation
Enamel matrix secretion
Alveolar bone remodeling
USAG 1 prevents excessive mineralization and aberrant morphogenesis by binding and modulating key signaling mediators.
Key Molecular Interactions
High-confidence protein interaction analyses demonstrate that USAG 1 integrates into a broader signaling network involving:
LRP5 – Wnt co-receptor critical for osteoblast proliferation
DKK4 – Fine-tunes Wnt signaling
BMP2 – Induces dentin and bone formation
BMP4 – Essential for tooth morphogenesis
BMP7 – Supports epithelial osteogenesis
Through these interactions, USAG1 maintains developmental balance. However, its inhibition removes molecular brakes on odontogenic signaling, reactivating regenerative capacity.
Single-Cell RNA Sequencing: Cellular Targets in Gingival Tissue
Recent transcriptomic analyses using DISCO v2.4 have provided unprecedented insight into USAG1 cell-type specificity.
Gingival Fibroblast Subpopulations
USAG1 expression is enriched in distinct human gingival fibroblast (HGF) subsets:
CD9⁺ APCDD1⁺ fibroblasts (≈45–50%)
Involved in Wnt pathway modulation
Participate in tissue remodeling and myofibroblast transition
CDH19⁺ LAMA2⁺ fibroblasts (≈30–35%)
Contribute to extracellular matrix composition
Support regenerative scaffolding
These fibroblast populations demonstrate regenerative plasticity and may influence therapeutic outcomes.
Basal Epithelial Cells
Approximately 60% of Krt14⁺ basal epithelial cells express USAG-1. These cells:
Maintain dental epithelial integrity
Exhibit BMP-dependent developmental plasticity
Contribute to tooth and taste bud lineage specification
This cell-specific mapping suggests that USAG-1 inhibition may act locally within gingival niches, influencing epithelial-mesenchymal interactions fundamental to tooth induction.
Preclinical Evidence: Induction of Third Dentition
Multiple murine studies have demonstrated that blocking USAG-1 can:
Restore missing teeth in congenital tooth agenesis models
Induce supernumerary teeth
Produce anatomically complete enamel and dentin
Achieve functional occlusion and jawbone integration
Most notably, anti-USAG-1 monoclonal antibody therapy achieved functional tooth regeneration in 100% of treated mice, with normal enamel and dentin architecture.
These findings confirm that postnatal mammalian dentition retains latent regenerative potential suppressed by USAG-1 activity.
Clinical Translation: Human Trials and Commercial Outlook
Clinical development has progressed rapidly, particularly in Japan.
A Phase I human trial initiated in 2024 at Kyoto University Hospital is evaluating safety and tolerability of anti-USAG-1 monoclonal antibodies in adults with acquired tooth loss.
Projected clinical pathway:
| Phase | Target Population | Primary Endpoint |
|---|---|---|
| Phase I (2024) | Adults with tooth loss | Safety, tolerability |
| Phase II (2026) | Congenital tooth agenesis | Tooth induction, integration |
| Phase III (2028+) | Broader populations | Long-term durability |
| Commercialization | ~2030 (Projected) | Regulatory approval |
If successful, this therapy may redefine standards of care in restorative dentistry.
Regenerative Scope: Beyond Tooth Crown Formation
Tooth regeneration is not limited to crown development. USAG-1 inhibition appears to influence multiple dental tissues:
1. Dentin and Pulp Regeneration
Enhanced BMP2/4/7 signaling promotes odontoblast differentiation and reparative dentinogenesis.
2. Gingival Repair
Wnt modulation improves fibroblast activity and epithelial proliferation.
3. Alveolar Bone Remodeling
BMP–Wnt crosstalk stimulates osteoblast differentiation and bone homeostasis.
4. SMAD and MAPK/ERK Crosstalk
Emerging evidence suggests downstream modulation of SMAD transcription factors and MAPK/ERK cascades, expanding the therapeutic impact beyond classical BMP–Wnt interactions.
Therapeutic Advantages Over Conventional Dentistry
Current restorative modalities include:
Dental implants
Fixed prostheses
Removable dentures
While effective, these approaches:
Do not restore periodontal ligament
Lack natural proprioception
Require surgical intervention
Risk peri-implantitis
In contrast, USAG-1–targeted therapy aims to:
Regenerate a biologically authentic tooth
Restore natural periodontal attachment
Achieve physiologic load distribution
Eliminate foreign biomaterials
This represents a true paradigm shift in precision regenerative dentistry.
Safety, Specificity, and Delivery Challenges
Despite promising outcomes, critical barriers remain:
1. Off-Target Effects
BMP and Wnt pathways regulate multiple organs, including kidney and bone. Systemic inhibition requires high specificity.
2. Delivery Optimization
Monoclonal antibodies must achieve effective local concentrations without systemic toxicity.
3. Patient Variability
Age, genetic background, dental morphology, and systemic health may influence regenerative outcomes.
4. Long-Term Surveillance
Durability of regenerated teeth and risk of aberrant mineralization must be evaluated over extended follow-up.
Regulatory and Ethical Considerations
Regenerative biologics face complex regulatory landscapes.
In the United States, the Food and Drug Administration regulates monoclonal antibody therapeutics under biologics frameworks. However, regenerative dentistry introduces novel classification challenges.
Global regulatory harmonization is essential to ensure:
Safety
Efficacy
Quality control
Ethical oversight
Additionally, cost and accessibility must be addressed to prevent inequitable distribution of advanced biologic therapies.
Cost and Global Accessibility
Monoclonal antibody production involves:
Recombinant protein engineering
Bioreactor manufacturing
Cold chain logistics
Specialized administration
Without scalable models, regenerative dentistry risks becoming limited to high-income healthcare systems.
International collaboration and health policy reform will be critical for equitable access.
Study Limitations and Knowledge Gaps
Current evidence is primarily derived from:
Murine preclinical models
Early-phase human trials
Unresolved questions include:
Long-term structural stability
Impact on occlusal dynamics
Interaction with orthodontic forces
Regenerative consistency across molars vs incisors
Further randomized clinical trials are necessary before integration into routine dental practice.
Future Directions in Precision Regenerative Dentistry
The convergence of:
Single-cell transcriptomics
Molecular signaling biology
Monoclonal antibody engineering
Translational clinical trials
Positions USAG-1 at the forefront of next-generation dental therapeutics.
Future innovations may include:
Localized injectable biologics
Scaffold-guided regeneration
Gene-editing approaches
Combination BMP/Wnt modulation therapies
Personalized regenerative strategies based on fibroblast and epithelial cell heterogeneity represent an emerging frontier.
Conclusion: Toward Biologically Authentic Tooth Regeneration
USAG-1 functions as a master regulator of odontogenesis through coordinated modulation of BMP and Wnt signaling networks. Inhibiting this gene has demonstrated the capacity to:
Induce third dentition
Restore congenital tooth agenesis
Regenerate dentin and pulp
Support alveolar bone remodeling
Clinical trials are currently underway, marking a historic transition from restorative substitution to true biological regeneration.
However, widespread clinical adoption requires:
Rigorous safety validation
Optimized delivery systems
Regulatory clarity
Ethical accessibility frameworks
If these challenges are addressed successfully, USAG-1–based therapies may redefine the future of dental medicine—transforming regenerative dentistry from aspiration to clinical reality.
Frequently Asked Questions (FAQ) About USAG-1 and Tooth Regeneration Therapy
1. What is USAG-1 treatment?
USAG-1 treatment refers to an experimental regenerative dental therapy that targets Uterine Sensitization-Associated Gene-1 (USAG-1), also known as SOSTDC1, using monoclonal antibodies. By inhibiting USAG-1, this therapy aims to reactivate dormant tooth-forming pathways in adults.
The treatment is currently being evaluated in early-phase human clinical trials, including those initiated at Kyoto University Hospital. The goal is to stimulate biologically authentic tooth regeneration rather than relying on prosthetics or implants.
2. What is the function of USAG-1?
USAG-1 functions as a dual antagonist of two major developmental signaling pathways:
Bone Morphogenetic Protein (BMP) signaling
Wnt/β-catenin signaling
These pathways regulate odontogenesis, stem cell differentiation, enamel formation, dentinogenesis, and alveolar bone remodeling.
By inhibiting BMP2, BMP4, BMP7, and Wnt co-receptors such as LRP5, USAG-1 maintains developmental balance and prevents excessive tooth formation.
3. What happens if you block USAG-1 protein?
Blocking USAG-1 removes its inhibitory effect on BMP and Wnt signaling. Preclinical studies demonstrate that this leads to:
Reactivation of tooth bud formation
Induction of supernumerary teeth
Regeneration of functional enamel and dentin
Restoration of missing teeth in congenital models
In murine experiments, anti–USAG-1 monoclonal antibodies resulted in fully formed, integrated teeth with normal morphology.
4. What is USAG protein?
USAG protein is the protein product of the USAG-1 gene (SOSTDC1). It is a secreted glycoprotein expressed in:
Kidney
Gingiva
Developing dental tissues
Salivary glands
Its biological role is to regulate tissue morphogenesis by modulating BMP and Wnt signaling pathways during embryonic development and postnatal tissue homeostasis.
5. Is USAG-1 therapy approved for dental use?
No. USAG-1–targeted therapies are still in clinical trial phases. Phase I human trials began in 2024 to evaluate safety and tolerability. Regulatory approval will depend on long-term efficacy and safety data.
Projected commercialization is anticipated around 2030, pending successful Phase II and III trials.
6. Can USAG-1 treatment regrow teeth in adults?
Preclinical evidence strongly suggests that USAG-1 inhibition can stimulate third dentition even in mature organisms. Human trials are currently assessing whether similar regenerative responses occur in adults with acquired tooth loss.
If successful, this would represent the first biologically authentic tooth regeneration therapy in dentistry.
7. How is USAG-1 therapy administered?
Current investigational approaches involve monoclonal antibody injections targeting USAG-1. The delivery method is designed to:
Achieve localized biological activation
Minimize systemic side effects
Precisely modulate BMP and Wnt pathways
The optimal dosage, frequency, and route of administration are still under investigation.
8. Is blocking USAG-1 safe?
So far, animal studies report minimal adverse effects. However, because BMP and Wnt pathways regulate multiple organs—including kidney and bone—long-term human safety data are essential.
Regulatory oversight from agencies such as the Food and Drug Administration will determine safety standards before approval.
9. Could USAG-1 therapy replace dental implants?
Potentially, yes. Unlike implants, USAG-1 therapy aims to regenerate a natural tooth complete with periodontal ligament, dentin, enamel, and pulp.
If proven effective, this could reduce reliance on prosthetic solutions and eliminate risks such as peri-implantitis.
However, implants remain the gold standard until regenerative therapies are clinically validated.
10. Who might benefit from USAG-1 treatment?
Future candidates may include:
Patients with congenital tooth agenesis
Adults with traumatic tooth loss
Individuals with developmental dental defects
Patients seeking biologic alternatives to prosthetics
Expanded trials will determine eligibility criteria across age groups and clinical scenarios.
Reference:
Recent Articles
Keywords: USAG-1, SOSTDC1, regenerative dentistry, tooth regeneration therapy, BMP signaling, Wnt signaling pathway, congenital tooth agenesis, monoclonal antibody, third dentition, dental stem cells
Introduction: A Paradigm Shift in Regenerative Dentistry
Tooth loss remains one of the most prevalent global health problems. Despite advances in implantology, biomaterials, and prosthodontics, modern dentistry still relies primarily on replacement rather than true biological regeneration. The discovery of Uterine Sensitization-Associated Gene-1 (USAG-1)—also known as SOSTDC1—has redefined the scientific landscape of regenerative dentistry by introducing the possibility of authentic tooth regrowth.
USAG-1 is a dual antagonist of the Bone Morphogenetic Protein (BMP) and Wnt signaling pathways, two master regulators of odontogenesis. By modulating these pathways, USAG1 governs dental morphogenesis, stem cell differentiation, enamel and dentin formation, and epithelial-mesenchymal interactions. Inhibiting USAG1 has demonstrated the capacity to reactivate dormant developmental programs, enabling the formation of supernumerary teeth and functional third dentition in preclinical models.
With monoclonal antibody therapies targeting USAG 1 already entering human clinical trials, regenerative dentistry is transitioning from theoretical biology to translational therapeutics.
Molecular Biology of USAG-1: Central Regulator of BMP and Wnt Signaling
USAG-1 as a Dual Pathway Antagonist
USAG 1 exerts regulatory control over two critical developmental cascades:
BMP signaling pathway
Canonical Wnt/β-catenin signaling pathway
These pathways are indispensable for:
Dental lamina formation
Tooth bud initiation
Odontoblast differentiation
Enamel matrix secretion
Alveolar bone remodeling
USAG 1 prevents excessive mineralization and aberrant morphogenesis by binding and modulating key signaling mediators.
Key Molecular Interactions
High-confidence protein interaction analyses demonstrate that USAG 1 integrates into a broader signaling network involving:
LRP5 – Wnt co-receptor critical for osteoblast proliferation
DKK4 – Fine-tunes Wnt signaling
BMP2 – Induces dentin and bone formation
BMP4 – Essential for tooth morphogenesis
BMP7 – Supports epithelial osteogenesis
Through these interactions, USAG1 maintains developmental balance. However, its inhibition removes molecular brakes on odontogenic signaling, reactivating regenerative capacity.
Single-Cell RNA Sequencing: Cellular Targets in Gingival Tissue
Recent transcriptomic analyses using DISCO v2.4 have provided unprecedented insight into USAG1 cell-type specificity.
Gingival Fibroblast Subpopulations
USAG1 expression is enriched in distinct human gingival fibroblast (HGF) subsets:
CD9⁺ APCDD1⁺ fibroblasts (≈45–50%)
Involved in Wnt pathway modulation
Participate in tissue remodeling and myofibroblast transition
CDH19⁺ LAMA2⁺ fibroblasts (≈30–35%)
Contribute to extracellular matrix composition
Support regenerative scaffolding
These fibroblast populations demonstrate regenerative plasticity and may influence therapeutic outcomes.
Basal Epithelial Cells
Approximately 60% of Krt14⁺ basal epithelial cells express USAG-1. These cells:
Maintain dental epithelial integrity
Exhibit BMP-dependent developmental plasticity
Contribute to tooth and taste bud lineage specification
This cell-specific mapping suggests that USAG-1 inhibition may act locally within gingival niches, influencing epithelial-mesenchymal interactions fundamental to tooth induction.
Preclinical Evidence: Induction of Third Dentition
Multiple murine studies have demonstrated that blocking USAG-1 can:
Restore missing teeth in congenital tooth agenesis models
Induce supernumerary teeth
Produce anatomically complete enamel and dentin
Achieve functional occlusion and jawbone integration
Most notably, anti-USAG-1 monoclonal antibody therapy achieved functional tooth regeneration in 100% of treated mice, with normal enamel and dentin architecture.
These findings confirm that postnatal mammalian dentition retains latent regenerative potential suppressed by USAG-1 activity.
Clinical Translation: Human Trials and Commercial Outlook
Clinical development has progressed rapidly, particularly in Japan.
A Phase I human trial initiated in 2024 at Kyoto University Hospital is evaluating safety and tolerability of anti-USAG-1 monoclonal antibodies in adults with acquired tooth loss.
Projected clinical pathway:
| Phase | Target Population | Primary Endpoint |
|---|---|---|
| Phase I (2024) | Adults with tooth loss | Safety, tolerability |
| Phase II (2026) | Congenital tooth agenesis | Tooth induction, integration |
| Phase III (2028+) | Broader populations | Long-term durability |
| Commercialization | ~2030 (Projected) | Regulatory approval |
If successful, this therapy may redefine standards of care in restorative dentistry.
Regenerative Scope: Beyond Tooth Crown Formation
Tooth regeneration is not limited to crown development. USAG-1 inhibition appears to influence multiple dental tissues:
1. Dentin and Pulp Regeneration
Enhanced BMP2/4/7 signaling promotes odontoblast differentiation and reparative dentinogenesis.
2. Gingival Repair
Wnt modulation improves fibroblast activity and epithelial proliferation.
3. Alveolar Bone Remodeling
BMP–Wnt crosstalk stimulates osteoblast differentiation and bone homeostasis.
4. SMAD and MAPK/ERK Crosstalk
Emerging evidence suggests downstream modulation of SMAD transcription factors and MAPK/ERK cascades, expanding the therapeutic impact beyond classical BMP–Wnt interactions.
Therapeutic Advantages Over Conventional Dentistry
Current restorative modalities include:
Dental implants
Fixed prostheses
Removable dentures
While effective, these approaches:
Do not restore periodontal ligament
Lack natural proprioception
Require surgical intervention
Risk peri-implantitis
In contrast, USAG-1–targeted therapy aims to:
Regenerate a biologically authentic tooth
Restore natural periodontal attachment
Achieve physiologic load distribution
Eliminate foreign biomaterials
This represents a true paradigm shift in precision regenerative dentistry.
Safety, Specificity, and Delivery Challenges
Despite promising outcomes, critical barriers remain:
1. Off-Target Effects
BMP and Wnt pathways regulate multiple organs, including kidney and bone. Systemic inhibition requires high specificity.
2. Delivery Optimization
Monoclonal antibodies must achieve effective local concentrations without systemic toxicity.
3. Patient Variability
Age, genetic background, dental morphology, and systemic health may influence regenerative outcomes.
4. Long-Term Surveillance
Durability of regenerated teeth and risk of aberrant mineralization must be evaluated over extended follow-up.
Regulatory and Ethical Considerations
Regenerative biologics face complex regulatory landscapes.
In the United States, the Food and Drug Administration regulates monoclonal antibody therapeutics under biologics frameworks. However, regenerative dentistry introduces novel classification challenges.
Global regulatory harmonization is essential to ensure:
Safety
Efficacy
Quality control
Ethical oversight
Additionally, cost and accessibility must be addressed to prevent inequitable distribution of advanced biologic therapies.
Cost and Global Accessibility
Monoclonal antibody production involves:
Recombinant protein engineering
Bioreactor manufacturing
Cold chain logistics
Specialized administration
Without scalable models, regenerative dentistry risks becoming limited to high-income healthcare systems.
International collaboration and health policy reform will be critical for equitable access.
Study Limitations and Knowledge Gaps
Current evidence is primarily derived from:
Murine preclinical models
Early-phase human trials
Unresolved questions include:
Long-term structural stability
Impact on occlusal dynamics
Interaction with orthodontic forces
Regenerative consistency across molars vs incisors
Further randomized clinical trials are necessary before integration into routine dental practice.
Future Directions in Precision Regenerative Dentistry
The convergence of:
Single-cell transcriptomics
Molecular signaling biology
Monoclonal antibody engineering
Translational clinical trials
Positions USAG-1 at the forefront of next-generation dental therapeutics.
Future innovations may include:
Localized injectable biologics
Scaffold-guided regeneration
Gene-editing approaches
Combination BMP/Wnt modulation therapies
Personalized regenerative strategies based on fibroblast and epithelial cell heterogeneity represent an emerging frontier.
Conclusion: Toward Biologically Authentic Tooth Regeneration
USAG-1 functions as a master regulator of odontogenesis through coordinated modulation of BMP and Wnt signaling networks. Inhibiting this gene has demonstrated the capacity to:
Induce third dentition
Restore congenital tooth agenesis
Regenerate dentin and pulp
Support alveolar bone remodeling
Clinical trials are currently underway, marking a historic transition from restorative substitution to true biological regeneration.
However, widespread clinical adoption requires:
Rigorous safety validation
Optimized delivery systems
Regulatory clarity
Ethical accessibility frameworks
If these challenges are addressed successfully, USAG-1–based therapies may redefine the future of dental medicine—transforming regenerative dentistry from aspiration to clinical reality.
Frequently Asked Questions (FAQ) About USAG-1 and Tooth Regeneration Therapy
1. What is USAG-1 treatment?
USAG-1 treatment refers to an experimental regenerative dental therapy that targets Uterine Sensitization-Associated Gene-1 (USAG-1), also known as SOSTDC1, using monoclonal antibodies. By inhibiting USAG-1, this therapy aims to reactivate dormant tooth-forming pathways in adults.
The treatment is currently being evaluated in early-phase human clinical trials, including those initiated at Kyoto University Hospital. The goal is to stimulate biologically authentic tooth regeneration rather than relying on prosthetics or implants.
2. What is the function of USAG-1?
USAG-1 functions as a dual antagonist of two major developmental signaling pathways:
Bone Morphogenetic Protein (BMP) signaling
Wnt/β-catenin signaling
These pathways regulate odontogenesis, stem cell differentiation, enamel formation, dentinogenesis, and alveolar bone remodeling.
By inhibiting BMP2, BMP4, BMP7, and Wnt co-receptors such as LRP5, USAG-1 maintains developmental balance and prevents excessive tooth formation.
3. What happens if you block USAG-1 protein?
Blocking USAG-1 removes its inhibitory effect on BMP and Wnt signaling. Preclinical studies demonstrate that this leads to:
Reactivation of tooth bud formation
Induction of supernumerary teeth
Regeneration of functional enamel and dentin
Restoration of missing teeth in congenital models
In murine experiments, anti–USAG-1 monoclonal antibodies resulted in fully formed, integrated teeth with normal morphology.
4. What is USAG protein?
USAG protein is the protein product of the USAG-1 gene (SOSTDC1). It is a secreted glycoprotein expressed in:
Kidney
Gingiva
Developing dental tissues
Salivary glands
Its biological role is to regulate tissue morphogenesis by modulating BMP and Wnt signaling pathways during embryonic development and postnatal tissue homeostasis.
5. Is USAG-1 therapy approved for dental use?
No. USAG-1–targeted therapies are still in clinical trial phases. Phase I human trials began in 2024 to evaluate safety and tolerability. Regulatory approval will depend on long-term efficacy and safety data.
Projected commercialization is anticipated around 2030, pending successful Phase II and III trials.
6. Can USAG-1 treatment regrow teeth in adults?
Preclinical evidence strongly suggests that USAG-1 inhibition can stimulate third dentition even in mature organisms. Human trials are currently assessing whether similar regenerative responses occur in adults with acquired tooth loss.
If successful, this would represent the first biologically authentic tooth regeneration therapy in dentistry.
7. How is USAG-1 therapy administered?
Current investigational approaches involve monoclonal antibody injections targeting USAG-1. The delivery method is designed to:
Achieve localized biological activation
Minimize systemic side effects
Precisely modulate BMP and Wnt pathways
The optimal dosage, frequency, and route of administration are still under investigation.
8. Is blocking USAG-1 safe?
So far, animal studies report minimal adverse effects. However, because BMP and Wnt pathways regulate multiple organs—including kidney and bone—long-term human safety data are essential.
Regulatory oversight from agencies such as the Food and Drug Administration will determine safety standards before approval.
9. Could USAG-1 therapy replace dental implants?
Potentially, yes. Unlike implants, USAG-1 therapy aims to regenerate a natural tooth complete with periodontal ligament, dentin, enamel, and pulp.
If proven effective, this could reduce reliance on prosthetic solutions and eliminate risks such as peri-implantitis.
However, implants remain the gold standard until regenerative therapies are clinically validated.
10. Who might benefit from USAG-1 treatment?
Future candidates may include:
Patients with congenital tooth agenesis
Adults with traumatic tooth loss
Individuals with developmental dental defects
Patients seeking biologic alternatives to prosthetics
Expanded trials will determine eligibility criteria across age groups and clinical scenarios.
Reference:
Recent Articles
Pulsed Electromagnetic Field (PEMF) Use in Implant Dentistry
Pulsed Electromagnetic Field (PEMF) Use in Implant Dentistry Abstract and Historical Background Pulsed Electromagnetic Field (PEMF) therapy refers to the application of low-frequency electromagnetic [...]
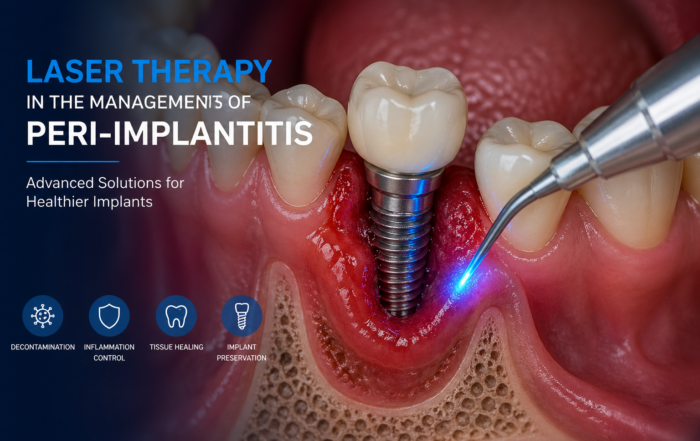
Laser Therapy in the Management of Peri-Implantitis
Laser Therapy in the Management of Peri-Implantitis Laser technology has become an increasingly valuable adjunct in the treatment of peri-implant diseases, particularly peri-implantitis. Its [...]
Magnetically Guided Dental Nanobots (CalBots) Are Real
Magnetically Guided Dental Nanobots (CalBots) Are Real The concept of nanobots in dentistry has long been associated with futuristic speculation. However, recent peer-reviewed research [...]
Peri-Implantitis Treatment & Prevention Methods
Peri-Implantitis Treatment & Prevention Methods Peri-implantitis remains one of the most significant biological complications affecting dental implants, posing a serious threat to long-term implant [...]
Latest Sinus Lifting Techniques in Modern Implant Dentistry
Latest Sinus Lifting Techniques in Modern Implant Dentistry A Comprehensive Clinical Review Introduction to Sinus Lifting in Implantology Sinus lifting, or maxillary sinus floor [...]
Biomechanics of the Triple Abutment & BOPiT Concept
Dental Biomechanics · Implant Science · Clinical Evidence Biomechanics of the Triple Abutment & BOPiT Concept How a saddle-shaped mathematical surface is rewriting the rules of load distribution [...]